Yale Medicine (March 12, 2023) – As we age, are melatonin starts rising at an earlier hour in the night, thus we may tend to go to sleep earlier than when we were younger. We still require the same number of hours of sleep (7-9 hours on average), so we may also rise earlier. Our sleep is more likely to be disturbed by medical conditions, medications, or substance use.
Tag Archives: Older Adults
Reviews: The Top 5 Articles On Healthy Aging In 2022
National Institute on Aging – As 2022 comes to a close, NIA invites you to explore some of the most popular health information topics from this past year:
High Blood Pressure and Older Adults
— High blood pressure, or hypertension, is common in older adults. The good news is that blood pressure can be controlled in most people.
What Is Menopause?
— Menopause is a normal part of aging for women, but it affects every woman differently.
Memory, Forgetfulness, and Aging: What’s Normal and What’s Not?
— As you age, you may wonder about the difference between normal, age-related forgetfulness and a serious memory problem, such as dementia.
Shingles
— Shingles is a disease that triggers a painful skin rash. About one in three people will get shingles, but there is a vaccine for older adults to help prevent the disease.
Vitamins and Minerals for Older Adults
— Vitamins and minerals are types of nutrients that your body needs to survive and stay healthy.
Telemedicine: Elderly Are Most Satisfied Study Finds
“Our study showed that the highest level of patient satisfaction within telemedicine visits was actually among patients within the 65 to 79-year-old age range—which has been an age group often seen as resistant to this mode of care,” says Bart Demaerschalk, M.D., a Mayo Clinic neurologist and senior author. “These findings show how important it is that health care organizations don’t exclusively target telemedicine to their younger, more tech-savvy patients.”
Mayo Clinic, November 3, 2022 – In one of the largest studies to date of its kind, Mayo Clinic researchers found patient satisfaction ratings to be equivalent for video telemedicine visits and in-person clinic visits. These findings highlight the potential for the use of telemedicine across a variety of patient populations.
The study, published in the Patient Experience Journal, evaluated patient satisfaction scores from over 300,000 patients treated either in-person or via video telemedicine during the COVID-19 pandemic.
While researchers found that patient satisfaction ratings were overall equivalent across the two modes of care, they did observe several interesting trends within certain age groups, genders, and races, which countered historical perceptions of telemedicine and represent opportunities for future study.
Regenerative Medicine: How It Slows Down Aging
“Diverse aging populations, vulnerable to chronic disease, are at the cusp of a promising future. Indeed, growing regenerative options offer opportunities to boost innate healing, and address aging-associated decline. The outlook for an extended well-being strives to achieve health for all,”
Andre Terzic, M.D., Ph.D., a Mayo Clinic cardiologist
Regenerative medicine could slow the clock on degenerative diseases that often ravage the golden years, a Mayo Clinic study finds. Life span has nearly doubled since the 1950s, but health span — the number of disease-free years — has not kept pace. According to a paper published in NPJ Regenerative Medicine., people are generally living longer, but the last decade of life is often racked with chronic, age-related diseases that diminish quality of life. These final years come with a great cost burden to society.
Researchers contend that new solutions for increasing health span lie at the intersection of regenerative medicine research, anti-senescent investigation, clinical care and societal supports. A regenerative approach offers hope of extending the longevity of good health, so a person’s final years can be lived to the fullest.
Osteoarthritis: Increased Walking Lowers Knee Pain
People with knee osteoarthritis may reduce their risk of knee pain by walking more, according to a study published online June 8, 2022, by Arthritis & Rheumatology.

Researchers looked at the walking habits of more than 1,200 people with knee osteoarthritis (average age 63, 45% men). They were asked how often they walked for exercise since age 50 and whether they had frequent knee pain. X-rays were done to assess structural knee damage.
The investigators first looked at participants who did not report regular knee pain. They found that among this group, those who walked for exercise were less likely to later develop knee pain (26%) at the follow-up eight years later compared with those who did not walk for exercise (37%).
Infographics: Chronic Wounds In Older Adults
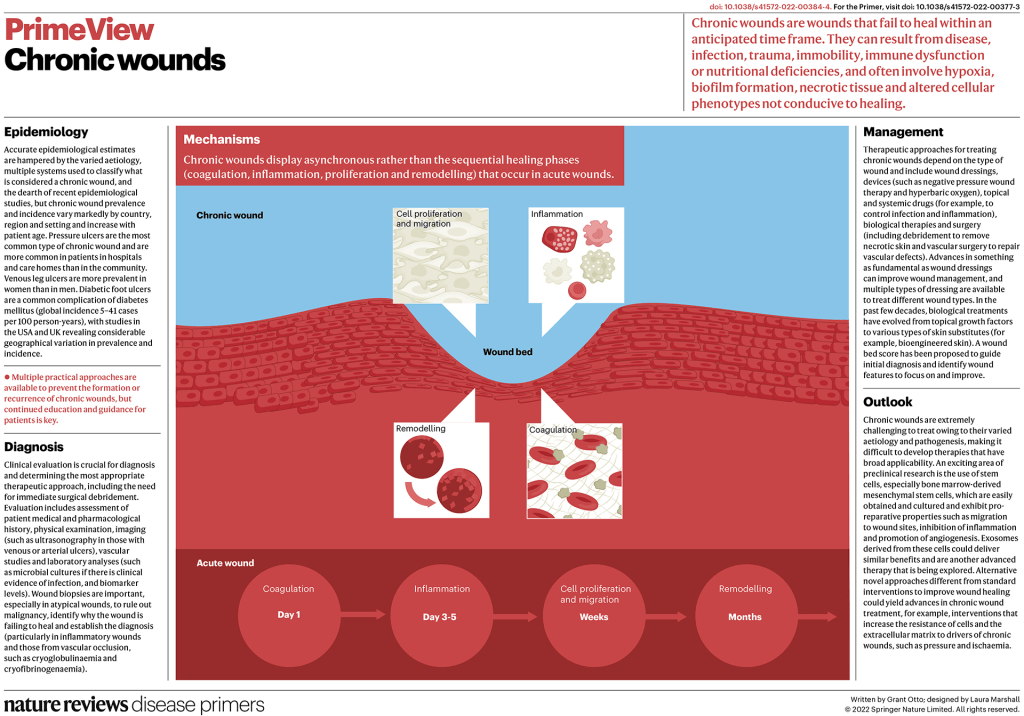
- •Chronic wounds are common, costly, and are more likely to affect older adults.
- •Venous ulcers, neuropathic ulcers, ischemic ulcers, and pressure injuries each necessitate unique prevention and treatment strategies.
- •With the evidence and pragmatic guidance provided herein, providers will have the working knowledge to successfully manage chronic wounds.
Appropriate prevention, diagnosis, and treatment of chronic wounds is important for providers across specialties. Wounds affect patients in all care settings and result in significant cost and morbidity. The burden of this condition falls largely on older adults, for whom the incidence of chronic wounds far exceeds that of younger populations.
Medicare costs for wound care in 2014 were estimated at greater than $28 billion, and the prevalence for most wound types was greatest in patients aged 75 or older.
Venous ulcers are the most common lower extremity wound type, comprising 45% to 60% of all wounds, followed by neuropathic ulcers (15% to 25%), ischemic ulcers (10% to 20%), and mixed ulcers (10% to 15%).
Fortunately, new wound-treatment modalities continue to emerge. This review summarizes the latest information regarding prevention, identification, classification, and treatment of chronic wounds. Guidance on management of major wound types and pearls regarding dressing selection are provided.
‘HARVARD MEDICINE’: THE AGING ISSUE – AUTUMN 2021
COVID-19 INFOGRAPHIC: MENTAL HEALTH AMONG OLDER ADULTS AGE 50-80
HEALTHCARE: OLDER ADULTS PREFER CONVENIENCE OVER REPUTATION IN PHYSICIANS
A new study by a team from the University of Michigan Institute for Healthcare Policy and Innovation shows that adults over age 50 place more importance on convenience-related factors, rather than reputation, when choosing a doctor.
The study, based on data from IHPI’s National Poll on Healthy Aging supported by AARP and Michigan Medicine, still shows that online ratings and reviews of physicians play an important role, and should receive attention from providers and policymakers.
Dr. Jeffrey Kullgren, a U-M primary care physician and lead author of the study, describes the findings.
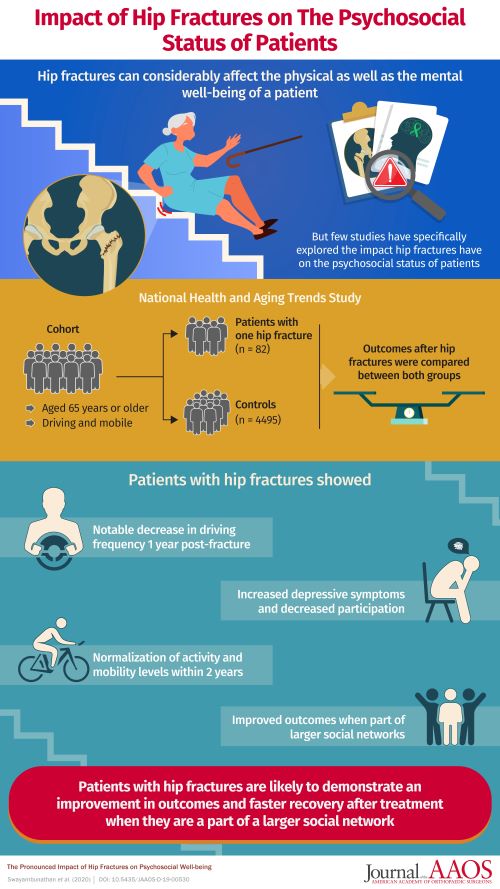
INFOGRAPHIC: PHYSICAL & MENTAL IMPACT OF HIP FRACTURES ON THE ELDERLY