A weekly podcast on the latest medical, science and telehealth news.
Tag Archives: Doctors
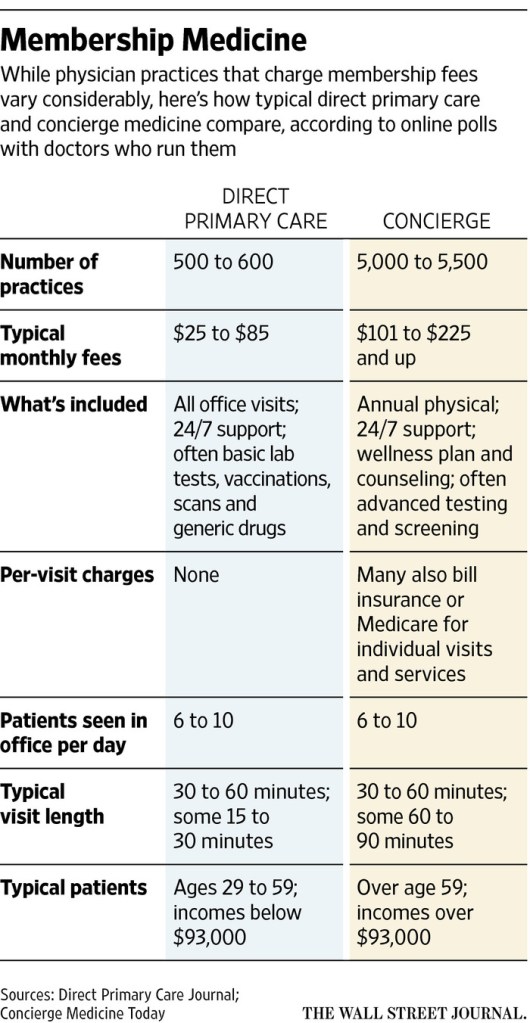
DR. C’S JOURNAL: THE RISE OF ‘CONCIERGE MEDICINE’
I am a physician. I believe that the modern medical care system is broken. It used to be that the patient selected the doctor because of her reputation, and the doctor was motivated for excellence. Now the doctor is apportioned by the insurance system, and the doctor is motivated to be “efficient” (to see more people in less time).
Coupled with electronics surveillance of doctors, requirement for electronic medical records, the expansion of patients in a doctors practice to quadruple the number it used to be, plus increasingly technological surgery ( I consider such doctors as technicians more than physicians ), a system of payment that favors such surgery,
With the “disease” model of medicine still dominant over the “health” model, it is difficult for the doctor to take patient’s phone calls, inform patients of their laboratory results, counsel them in nutrition, exercise, sleep, and other health benefits, or even see them the same day as their illness. Thus “go to the emergency room“ is the default advice.
The concierge doctor attempts to remedy some or or most of these deficiencies, which characterize the usual modern medical practice. Concierge medicine is so different from regular medicine as to draw the interest of Congress in preventing such discriminatory behavior.
Of course, the concierge doctor charges a periodic fee to deliver these services; there in lies it’s “unfairness”. I have even heard of super concierge doctors who meet your injured child at the emergency room with the chief of orthopedics , or fly with you to the Sloan Kettering Institute if you need consultation there. They, of course, charge tens of thousands of dollars annually for such service.
We already have multiple tier medical systems in America. The original concierge Idea modeled the care delivered to professional athletes, who must stay healthy in order to play.
Of course, there are still good doctors out there if you look hard enough and are lucky. Some family practitioners and internists still manage to practice quality medicine. Otherwise, my advice is to find a concierge doctor you can afford.
–Dr. C
HEALTHCARE: OLDER ADULTS PREFER CONVENIENCE OVER REPUTATION IN PHYSICIANS
A new study by a team from the University of Michigan Institute for Healthcare Policy and Innovation shows that adults over age 50 place more importance on convenience-related factors, rather than reputation, when choosing a doctor.
The study, based on data from IHPI’s National Poll on Healthy Aging supported by AARP and Michigan Medicine, still shows that online ratings and reviews of physicians play an important role, and should receive attention from providers and policymakers.
Dr. Jeffrey Kullgren, a U-M primary care physician and lead author of the study, describes the findings.
DOCTORS PODCAST: MEDICAL & TELEHEALTH NEWS (FEB 22)
A bi-weekly podcast on the latest medical, science and telehealth news.
TELEMEDICINE: “HEAL PASS” – PHYSICIAN “HOUSE CALLS” FOR FIXED MONTHLY FEE
By providing house calls and telemedicine from physicians at a fixed monthly fee with no copays, no deductibles, and no insurance required, Heal Pass is making affordable healthcare possible for the estimated 27 million Americans who recently lost their health insurance along with their jobs because of COVID-19.
- Heal patients can register now for the new service starting at $49 per month.
- Adults can add members of their household to their Heal Pass account for an additional $10 per person each month and may register up to six people to the account.
- Patients spend an average of $800 out of pocket each year, in addition to $2,000 for an emergency room visit.
- With Heal Pass, a family of four would receive up to 36 total appointments at an average cost of less than $27.
- Individual patients can save up to $1,100 per year and the average family can save up to $2,200 per year.
Uninsured individuals and their families are fearful of getting sick and accumulating high medical bills during this time of economic uncertainty.
Heal Pass is not health insurance, but it is health assurance, giving the uninsured the comfort of knowing they can get the care they need at a fixed, low fee with no surprise bills or out of pocket costs.
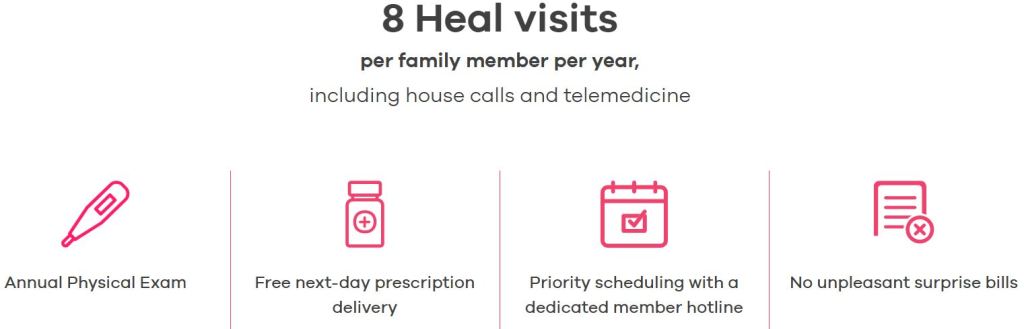
The new program allows up to eight house calls or telemedicine appointments per member each year in addition to an annual physical, helping with patients’ most common needs, including primary care, preventive care, non-emergency urgent care and chronic disease management.
It also includes free next day delivery of medications prescribed by a Heal doctor. Heal doctors are highly qualified and deliver house calls and care in a way that keeps patients safe from COVID-19 exposure as the country sees a pronounced second spike with 58,618 cases per day on average over the last seven days.
COMMENTARY
Telemedicine and Covid 19 are fermenting together and creating some new ideas for medical care.
Safety is a concern, and what could be better than your own home, using telemedicine, or a futuristic telemedicine booth located at convenient locations for the busy traveler?
Convenience is another attraction, with a PREPAID aliquot of healthcare; this idea was featured by Forward Health, reviewed a couple of weeks ago, which offered a package of remote monitors and 24/7 access for $149 per month.
Now, Heal pass offers 24/7 access they call “house calls” for $49. a month, with a blizzard of statistics on what you will save. We will see.
You usually get what you pay for.
The Onmed station sounds doable, and has the advantage of self-contained units that may be available to you at the right place and time. You could conceivably even wind up with a prescription as you exit the booth.
—Dr. C.
THE HEALING POWERS OF YOUR POSITIVE ATTITUDE
Do not go gentle into that good night,
Old age should burn and rave at close of day;
Rage, rage against the dying of the light.
From “Do Not Go Gentle Into That Good Night” by Dylan Thomas
My brother recently sent me a video featuring a confident man with a famous last name and a winning message: You beat Covid by fighting it. I would like to comment on several recommendations in his inspiring speech.
It is usually best to approach a problem with a POSITIVE ATTITUDE and a PLAN (1). This is particularly true with the ravages of old age (my area of expertise). Memory loss? Try to memorize poems. Balance loss? Practice standing on one leg. However………….
One person’s good experience is not a medical study. Medicine calls it a testimonial. This applies to my individual experiences as well. Going forward, I will be recounting many personal experiences with common diseases and conditions. Be careful about applying my solutions to your condition.. EXERCISE CRITICAL THINKING.
Be especially careful not to equate fame with medical expertise.
Mr. Cuomo’s result, if indeed the outcome was changed by his efforts, was most likely influenced by a powerful PLACEBO effect (2) which can be associated with striking outcomes, as we know from countless inspiring testimonials of “hopeless” cancer and other terminal conditions.
Even if we KNOW a treatment is likely due to the placebo effect, it remains effective. I don’t believe I’m doing harm with my speculations.
A couple of generations ago, confidence in doctors was much greater than it is now. We had fewer effective treatments, but surprisingly good results. As medical information of various quality proliferates and medicine loses prestige, it it is losing a valuable tool. Still, we have the placebo effect.
Mr. Cuomo was fortunate to have a good, positive doctor, and to believe in him. Positive affect is powerful.
FEVER is not the virus incarnate, but the bodies RESPONSE to the virus. Fever survived the culling of evolution because it confers a survival advantage, and is helpful.(3) Viruses replicate less rapidly at higher body temperatures.
I always told my patients: “ if you are stuck with the infection, enjoy the fever”. Of course high fevers, above 104 degrees F should be reduced.
I’m not sure that Covid patients should hold their breaths to “fight the virus”, although the length of time you can hold your breath is a good measure of breathing difficulty. Blood CO2, the main driver of dyspnea (shortness of breath), must not be allowed to accumulate. The accompanying hypoxemia (low blood oxygen ) is not desirable either.
I agree with most of the advice quoted by Mr. Cuomo. Lying on the back has proven dangerous in severe Covid. Taking deep breaths (even if painful) will help keep the alveoli (air sacs) expanded. Change of position is important for the same reason, and adequate fluids, including water, is always beneficial.
So educate yourself as much as you can about your condition. Pick out the best doctor you can find (the subject of a future opinion piece) and place yourself in her care. Enjoy a sense of relief and confidence. Even physicians need the objectivity and support of their own doctor.
Finally, armed with a positive attitude, make the most of whatever placebo effect you are accorded.
—Dr. C.
TELECONSULTING: “DEEP BREATH IN” – THE BMJ LAUNCHES A NEW PODCAST
The BMJ’s new podcast aims to help doctors feel more connected, heard, and supported
“Deep breath in … and out. Again, deep breath in … and out.”
We tune in to patients’ breath sounds, seeking confirmation of a diagnosis—one more supporting piece of evidence to reassure anxious patients or to narrow the differential.
But since the SARS-CoV-2 pandemic arrived, saying “deep breath in” has been replaced by the need to take one ourselves: before looking at the morning news, before venturing out (or logging on) to work each morning, and before ringing the next patient on your list with the ominous note alongside their name: “fever and cough for a week, now feeling breathless.” Although chosen in what seems like a different era, the name for The BMJ’s new podcast for general practitioners—Deep Breath In—seems fitting for our troubled times.
Rebooting general practice
Before anyone in Wuhan fell ill, GPs had already been feeling the strain. In the UK, despite government promises of 5000 new practising GPs by 2020, there were 6.2% fewer full time equivalent GPs in 2019 than in 2015.1 Similarly, physicians in the US have been compensating for an estimated shortfall of some 14 500 primary care doctors since 2017.2 Recent attempts to take the strain off GPs in England by funding allied health professionals have faltered because of onerous new demands on fledgling primary care networks.3 Turning it off and switching it back on again is often the only thing that works when your computer grinds to a halt. Perhaps coronavirus will do the same for primary care.
COMMENTARY
Primary Care Physicians are a vanishing species [1]. This is unfortunate, since PCPs are the only doctors who attend the whole field of Medicine (have you ever asked an orthopedist about your cough?).
However, some of the slack is being taken up by Nurse Practitioners [2] and Physicians Assistants [3].
If you know a retired Internist or Family Practice Physician, be sure to cultivate a friendly relationship (and give them a hug when the Covid 19 epidemic cools off). They might be inclined to be that greatest of all Medical Resources- the Patient Advocate [4].
—Dr. C.







