- Expanded Patient Base
Late appointments and no-shows are frustrating elements of in-person care. They result in lost time for the healthcare practitioner (HCP) as well as lost opportunities to reach out to a new patient.
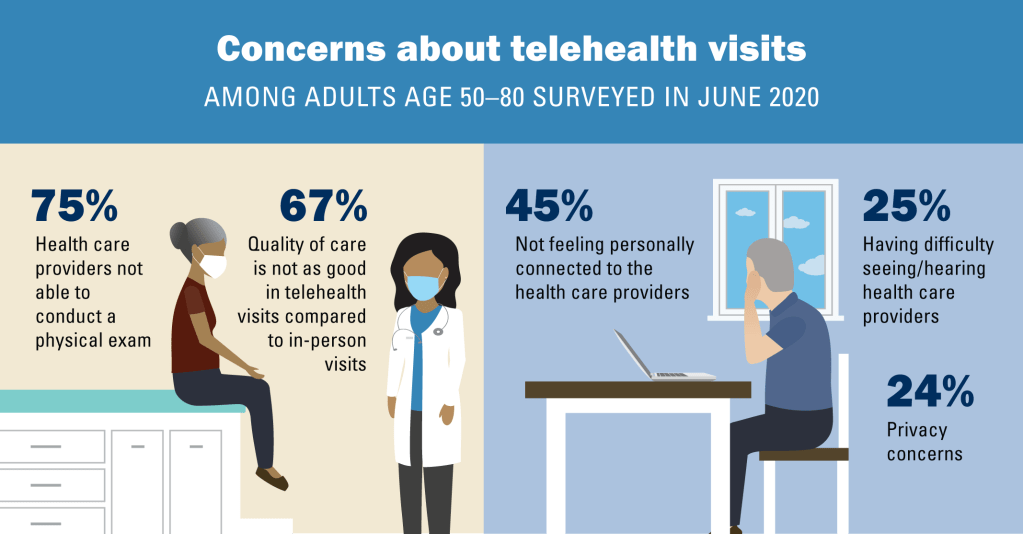
Virtual medical visits can reduce no-shows and increase treatment persistence. In a recent survey, U.S. patients who experienced telehealth visits rated this type of healthcare highly (above 80% positive), saying that using the method was beneficial to their mental health as well.
Additionally, HCPs can use telehealth to dramatically expand their patient base, as the technology provides easy access and scheduling. In a cross-sectional survey, 52.5% of clinicians said virtual visits allow for higher efficiency—and that its quality was equal to that of in-person visits.
- Increased Patient Flexibility
Patients must consider a variety of personal barriers when booking a doctor’s appointment: travel time, time off work, childcare. Telehealth visits dramatically reduce these considerations, reducing stress and increasing flexibility. Even established patients highly appreciate and prefer its convenience because of such advantages as family closeness, preferred modality, and improved self-management.
Patients benefit as well from reduced transportation and waiting times. Collectively, on-demand virtual visits can help your patients balance work, life, and healthcare.
- Increased Collaboration Opportunities Among Medical Disciplines
Optimized communication between patient-directed disciplines and diagnostic facilities is important for achieving fast and straightforward healthcare measures. The faster pace of treatment times and therapies that may result could benefit patients’ well-being.
Combining expertise increases diagnostic value. Doctors can easily invite consulting physicians to attend virtual visits on demand and quickly offer a second opinion or additional experience.
Digital platforms also offer easy access to congresses, seminars, and trainings, which reduces cost, time, and effort, strongly supporting the medical education of your healthcare personnel.
- Increased Patient Adherence
Easy access to generalists and specialists is key for patient adherence, treatment success, and hospital promotion. Proven factors include close monitoring, satisfaction, and short waiting periods.
Additionally, in regard to mental health, telehealth services have been proven to effectively support service delivery and reduction of depressive symptoms.
Virtual care is a promising approach to increase and keep patient adherence and persistence. Even for novel disease onsets, patients may stay with their preferred healthcare institution. Plainly stated: the happy patient comes back again.
- Easier Patient Follow-Up
Advances in treatment adherence and persistence mainly rely on regular and systematic touchpoints by HCPs. Telehealth opportunities and remote care options can create a variety of these touchpoints in personalized and case-specific ways, ranging from an overview of patient consultations to implantable cardiac monitors. Remote monitoring especially holds tremendous potential to profit from telehealth applications.
Depending on the disease and patient type, digital engagement and follow-up can greatly benefit treatment outcomes and quality of life. Digital symptom calendars and diagnostic tools support treatment decisions and speed.
- Improved Patient Outcomes
By using telehealth options, health-compromised patients have a lower risk of infection from classic healthcare-associated pathogens such as multiresistant Staphylococcus aureus (MRSA). Telehealth can reduce complications and potential disease progression for patients.
Physicians using telehealth have more possibilities to educate patients about their treatment plan, whether about medication or hands-on therapy. By using digital tools, zooming in scans for a close-up or providing self-injection videos, doctors can offer flexible and direct communication, which can improve patient satisfaction.
Telehealth also presents an opportunity for a physician or care team to see the environment of the patient and identify any issues the patient might not have mentioned and allow for an improved treatment plan.
- Physicians and Care Teams’ Health
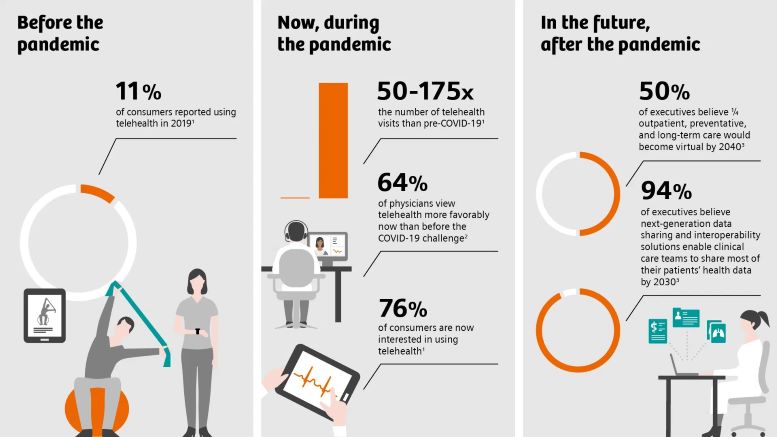
Especially during the pandemic, doctors using telehealth could maintain the necessary distance from potentially infectious patients while staying in touch digitally. Virtual consultations became applicable and led to the rising numbers of features and platforms.
Besides the pivotal role of protecting doctors’ physical health, telehealth options also allow for optimized workload planning, improving physicians’ work-life balance. In a representative survey among 1,594 physicians across the U.S., 55% agreed or strongly agreed that “telehealth has improved the satisfaction of my work.”
- Cost Reduction
Telehealth solutions can reduce costs in various medical disciplines, such as dermatology, pediatric medicine, and cardiology. General expenses, like front-desk support, space for medical examination rooms, and material can also be reduced. Telehealth opportunities may reflect a favorable add-on for your hospital, considering their easy implementation, financial benefits, and cost reduction.
The benefits of telehealth opportunities are striking—for patients, doctors, and hospitals. Constantly increasing the number of services, tools, devices, and apps that enter the market has significantly improved healthcare procedures across all medical disciplines. Covid-19 opened the door for telehealth and digital medicine, and now it’s here to stay.