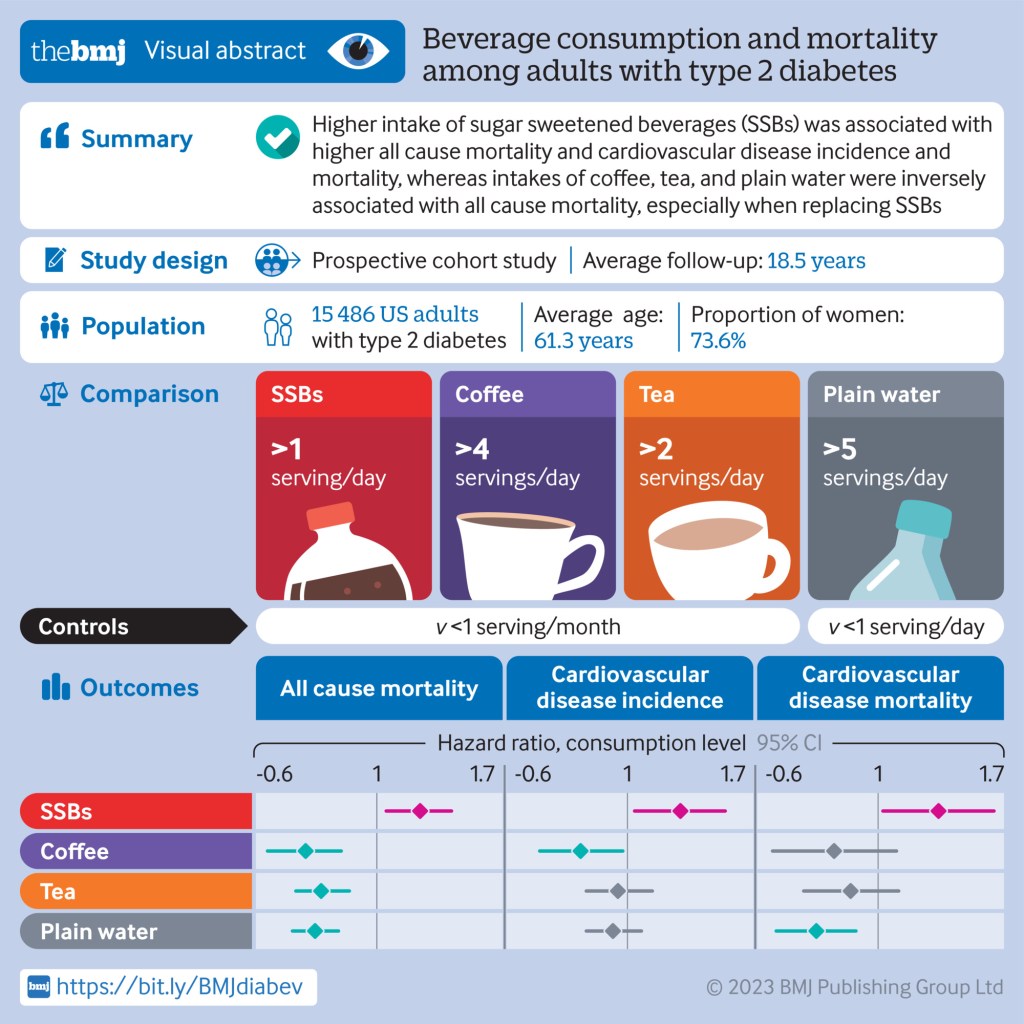
Systemic arterial hypertension is the most important modifiable risk factor for all-cause morbidity and mortality worldwide and is associated with an increased risk of cardiovascular disease (CVD).
Fewer than half of those with hypertension are aware of their condition, and many others are aware but not treated or inadequately treated, although successful treatment of hypertension reduces the global burden of disease and mortality. The aetiology of hypertension involves the complex interplay of environmental and pathophysiological factors that affect multiple systems, as well as genetic predisposition.
The evaluation of patients with hypertension includes accurate standardized blood pressure (BP) measurement, assessment of the patients’ predicted risk of atherosclerotic CVD and evidence of target-organ damage, and detection of secondary causes of hypertension and presence of comorbidities (such as CVD and kidney disease). Lifestyle changes, including dietary modifications and increased physical activity, are effective in lowering BP and preventing hypertension and its CVD sequelae.
Pharmacological therapy is very effective in lowering BP and in preventing CVD outcomes in most patients; first-line antihypertensive medications include angiotensin-converting enzyme inhibitors, angiotensin II receptor blockers, dihydropyridine calcium-channel blockers and thiazide diuretics.