
Globally, more people die from cardiovascular disease every year than from any other cause. Read more.

Globally, more people die from cardiovascular disease every year than from any other cause. Read more.
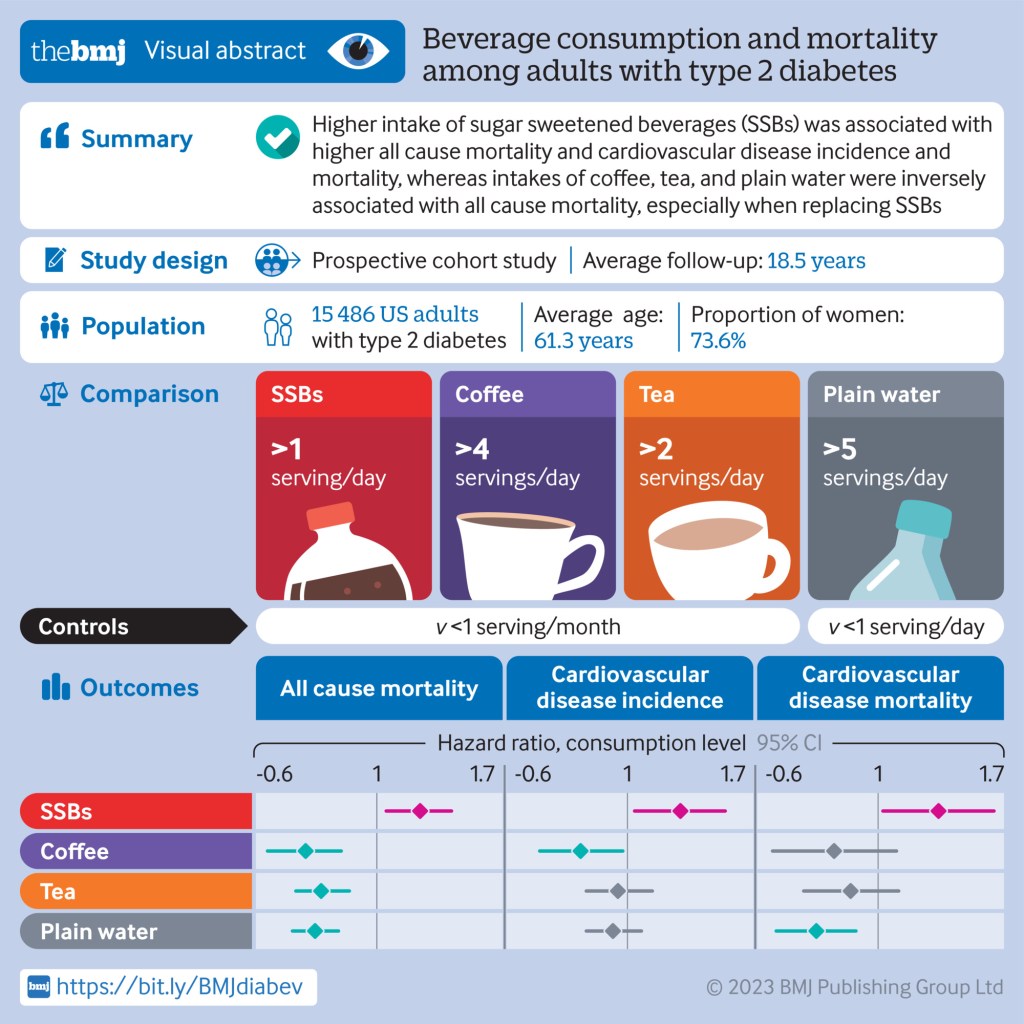
The BMJ (Published April 19, 2023) –
Conclusions: Individual beverages showed divergent associations with all cause mortality and CVD outcomes among adults with type 2 diabetes. Higher intake of SSBs was associated with higher all cause mortality and CVD incidence and mortality, whereas intakes of coffee, tea, plain water, and low fat milk were inversely associated with all cause mortality. These findings emphasize the potential role of healthy choices of beverages in managing the risk of CVD and premature death overall in adults with type 2 diabetes.

Frequent exercise is robustly associated with a decrease in cardiovascular mortality as well as the risk of developing cardiovascular disease. Physically active individuals have lower blood pressure, higher insulin sensitivity, and a more favorable plasma lipoprotein profile. Animal models of exercise show that repeated physical activity suppresses atherogenesis and increases the availability of vasodilatory mediators such as nitric oxide.
Exercise has also been found to have beneficial effects on the heart. Acutely, exercise increases cardiac output and blood pressure, but individuals adapted to exercise show lower resting heart rate and cardiac hypertrophy.
March 2023: In this episode of the Heart podcast, Digital Media Editor, Professor James Rudd, is joined by Dr Chris Wilkinson from Hull York Medical School and the James Cook hospital, UK. They discuss the concept of frailty and why it’s an important concept in cardiology.

Our new position paper with @worldheartfed summarises the relationship between obesity and cardiovascular disease (#CVD) mortality.

World Obesity Federation (January 2023) – The ongoing obesity epidemic represents a global public health crisis that contributes to poor health outcomes, reduced quality of life, and >2.8 million deaths each year. Obesity is relapsing, progressive, and heterogeneous. It is considered a chronic disease by the World Obesity Federation (WOF) and a chronic condition by the World Heart Federation (WHF).
People living with overweight/obesity are at greater risk for cardiovascular (CV) morbidity and mortality. Increased adiposity (body fat), particularly visceral/abdominal fat, is linked to CV risk and CV disease (CVD) via multiple direct and indirect pathophysiological mechanisms. The development of CVD is driven, in part, by obesity-related metabolic, endocrinologic, immunologic, structural, humoral, haemodynamic, and functional alterations.
Learn more: http://bit.ly/3THvOZa


In December 2020, a week before cardiologist Stuart Katz was scheduled to receive his first COVID-19 vaccine, he came down with a fever. He spent the next two weeks wracked with a cough, body aches and chills. After months of helping others to weather the pandemic, Katz, who works at New York University, was having his own first-hand experience of COVID-19.
On Christmas Day, Katz’s acute illness finally subsided. But many symptoms lingered, including some related to the organ he’s built his career around: the heart. Walking up two flights of stairs would leave him breathless, with his heart racing at 120 beats per minute. Over the next several months, he began to feel better, and he’s now back to his normal routine of walking and cycling. But reports about COVID-19’s effects on the cardiovascular system have made him concerned about his long-term health. “I say to myself, ‘Well, is it really over?’” Katz says.
In one study1 this year, researchers used records from the US Department of Veterans Affairs (VA) to estimate how often COVID-19 leads to cardiovascular problems. They found that people who had had the disease faced substantially increased risks for 20 cardiovascular conditions — including potentially catastrophic problems such as heart attacks and strokes — in the year after infection with the coronavirus SARS-CoV-2. Researchers say that these complications can happen even in people who seem to have completely recovered from a mild infection.
Some smaller studies have mirrored these findings, but others find lower rates of complications. With millions or perhaps even billions of people having been infected with SARS-CoV-2, clinicians are wondering whether the pandemic will be followed by a cardiovascular aftershock. Meanwhile, researchers are trying to understand who is most at risk of these heart-related problems, how long the risk persists and what causes these symptoms.
COMMENTARY:
The heart and Covid are connected from a variety of angles.
Obese people with high blood fats, diabetes, the metabolic syndrome tend to have atherosclerosis and heart problems, making them more susceptible to severe Covid and long Covid. Covid loves to involve the lining of blood vessels and the heart, the endothelium, where the number of ACE receptors are high.
The respiratory tract and lung are a particular target for Covid, and reduced oxygen from lung involvement can compromise the hard-working heart.
Heart cells, cardio myocytes, can be directly infected with the virus. Even Covid vaccines can rarely produce myocarditis, raising the possibility that there is some antigenic similarity between the virus and heart cells, similar to the beta hemolytic streptococcus and the heart which sets up rheumatic fever.
If this similarity is real, the tendency of Covid to compromise the immune system and produce a cytokine storm in severe cases could therefore specifically involve the heart.
The nature article indicates several different varieties of heart problems and is a recommended read. From my personal standpoint, arrhythmias were mentioned, and I already have trouble with a couple of different types, AF and NSVT.
To make definite statements about the likelihood of heart involvement in Covid is problematic. The patients reported on were infected with an earlier strain of Covid, and the present one, BA.5, seems to be milder, and may not be as hard on the heart as previous strains. Many more people are now immunized, and the most susceptible patients may have passed away. There are medications to take, such as remdesivir, and even select immune globulins, such as an immuno-suppressed friend of mine was given when he contracted Covid recently.
The bottom line for me is that I am 90 years old and have no desire to let Covid have a crack at me, so I avoid big gatherings, and wear a mask whenever I am exposed.
—Dr. C.
The most common heart attack symptom in women is the same as in men — some type of chest pain, pressure or discomfort that lasts more than a few minutes or comes and goes.
But chest pain is not always severe or even the most noticeable symptom, particularly in women. Women often describe heart attack pain as pressure or tightness. And it’s possible to have a heart attack without chest pain.
Women are more likely than men to have heart attack symptoms unrelated to chest pain, such as:
These symptoms may be vague and not as noticeable as the crushing chest pain often associated with heart attacks. This might be because women tend to have blockages not only in their main arteries but also in the smaller ones that supply blood to the heart — a condition called small vessel heart disease or coronary microvascular disease.
ess than 7% of the U.S. adult population has good cardiometabolic health, a devastating health crisis requiring urgent action, according to research led by a team from the Friedman School of Nutrition Science and Policy at Tufts University in a pioneering perspective on cardiometabolic health trends and disparities published in the July 12 issue of the Journal of the American College of Cardiology. Their team also included researchers from Tufts Medical Center.
Researchers evaluated Americans across five components of health: levels of blood pressure, blood sugar, blood cholesterol, adiposity (overweight and obesity), and presence or absence of cardiovascular disease (heart attack, stroke, etc.). They found that only 6.8 percent of U.S. adults had optimal levels of all five components as of 2017-2018.
The routine mammograms women receive to check for breast cancer may also offer clues to their risk for heart disease, new research suggests.
White spots or lines visible on mammograms indicate a buildup of calcium in breast arteries. This breast arterial calcification is different from coronary artery calcification, which is known to be a marker for higher cardiovascular risk. For the study, researchers followed 5,059 postmenopausal women (ages 60 to 79) for six and a half years. They found that those with breast arterial calcification were 51% more likely to develop heart disease or have a stroke than those without calcification. The study was published March 15, 2022, in Circulation: Cardiovascular Imaging.