New Scientist – The biggest immune organ is our gut and what we eat can support a healthy immune response. From eating the rainbow, consuming more fermented foods or fasting longer overnight, King’s College epidemiologist Tim Spector has top tips to boost your immunity through what you eat.
Category Archives: Prevention
Regenerative Medicine: How It Slows Down Aging
“Diverse aging populations, vulnerable to chronic disease, are at the cusp of a promising future. Indeed, growing regenerative options offer opportunities to boost innate healing, and address aging-associated decline. The outlook for an extended well-being strives to achieve health for all,”
Andre Terzic, M.D., Ph.D., a Mayo Clinic cardiologist
Regenerative medicine could slow the clock on degenerative diseases that often ravage the golden years, a Mayo Clinic study finds. Life span has nearly doubled since the 1950s, but health span — the number of disease-free years — has not kept pace. According to a paper published in NPJ Regenerative Medicine., people are generally living longer, but the last decade of life is often racked with chronic, age-related diseases that diminish quality of life. These final years come with a great cost burden to society.
Researchers contend that new solutions for increasing health span lie at the intersection of regenerative medicine research, anti-senescent investigation, clinical care and societal supports. A regenerative approach offers hope of extending the longevity of good health, so a person’s final years can be lived to the fullest.
Health: American Heart Association Checklist
The American Heart Association (AHA) recently revised its checklist for achieving optimal heart health, introducing its new Life’s Essential 8. The list replaces the AHA’s decade-old Life’s Simple 7.
Sleep health is the new addition to the cardiovascular health scoring tool, which now advises that adults get seven to nine hours per night. The organization updated four of the categories:
- Diet: More emphasis was given to following heart-healthy diets like the DASH and Mediterranean.
- Nicotine exposure: Secondhand smoke and vaping were added as risk factors.
- Blood lipids: People now can get a non-fasting blood sample that measures total, HDL, and non-HDL cholesterol. Non-HDL cholesterol can provide similar risk information as LDL cholesterol.
- Blood sugar: Measurements now include hemoglobin A1c, a key component to assessing type 2 diabetes risk.
- Three categories were unchanged:
- Physical activity: The optimal weekly level is at least 150 minutes of moderate activity or 75 minutes of vigorous activity.
- Body mass index (BMI): A BMI of 18.5 to 24.9 is ideal for heart health.
- Blood pressure: Levels less than 120/80 millimeters of mercury (mm Hg) remain optimal. Stage 1 hypertension is 130 to 139 mm Hg for systolic pressure (the first number) or 80 to 89 mm Hg for diastolic pressure (the second number).
- You can calculate your heart health score at mlc.heart.org. The guidelines were published online June 29, 2022, by Circulation.
Prevention: The Benefits Of Well-Woman Exams

For women and people assigned female at birth (AFAB), taking care of your health requires more than an annual physical. You should also visit a women’s health specialist — like an Ob/Gyn, midwife or nurse practitioner — each year to keep healthy. More than just a checkup for your breasts/chest and reproductive organs; well-woman exams can also help you develop rapport with a women’s health specialist.
“Well-women exams are important for a number of reasons. No. 1 is that they help you to establish care with a specialist so that if there is a problem down the road, you have a provider that you know and feel comfortable talking to,” says Ob/Gyn Amanda Elbin, MD.
That comfort level is important, too, especially because many of us may not feel comfortable talking with just anyone about issues “down there.”

Reports: Tufts Health & Nutrition – October 2022
Technology: How AI Can Improve Diagnostics (GAO)
Each year, medical diagnosis errors affect the health of millions of Americans and cost billions of dollars. Machine learning technologies can help identify hidden or complex patterns in diagnostic data to detect diseases earlier and improve treatments.
Several machine learning (ML) technologies are available in the U.S. to assist with the diagnostic process. The resulting benefits include earlier detection of diseases; more consistent analysis of medical data; and increased access to care, particularly for underserved populations. GAO identified a variety of ML-based technologies for five selected diseases
- Certain cancers,
- Diabetic retinopathy,
- Alzheimer’s disease,
- Heart disease,
- COVID-19
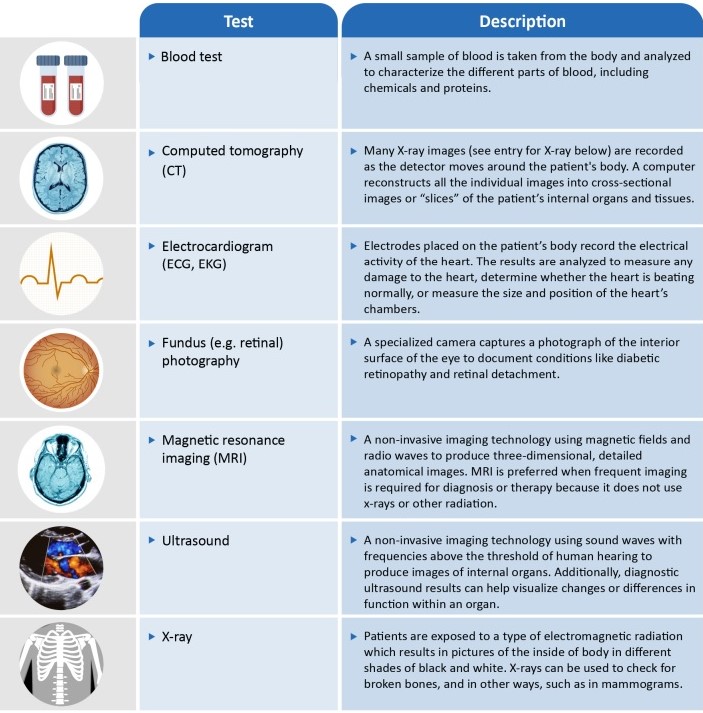
Most technologies relying on data from imaging such as x-rays or magnetic resonance imaging (MRI). However, these ML technologies have generally not been widely adopted.
Osteoarthritis: Increased Walking Lowers Knee Pain
People with knee osteoarthritis may reduce their risk of knee pain by walking more, according to a study published online June 8, 2022, by Arthritis & Rheumatology.

Researchers looked at the walking habits of more than 1,200 people with knee osteoarthritis (average age 63, 45% men). They were asked how often they walked for exercise since age 50 and whether they had frequent knee pain. X-rays were done to assess structural knee damage.
The investigators first looked at participants who did not report regular knee pain. They found that among this group, those who walked for exercise were less likely to later develop knee pain (26%) at the follow-up eight years later compared with those who did not walk for exercise (37%).
Prevention: Flu Shots Lower Heart Attack Risks
Influenza-related stress on your body can launch a negative chain of events that builds toward a heart attack. This video shares how getting a seasonal flu shot can significantly lower your risk of having a heart attack or cardiac arrest, especially if you’re in a high-risk group.
Chapters: 0:00 Can flu shots lower risk of heart attacks? 0:37 How does the flu shot lower risk of heart attacks? 1:08 Who is most at risk of having a flu related heart attack? 1:30 Why else should you get a flu shot?

Tendinopathy: Diagnosis, Treatment & Prevention
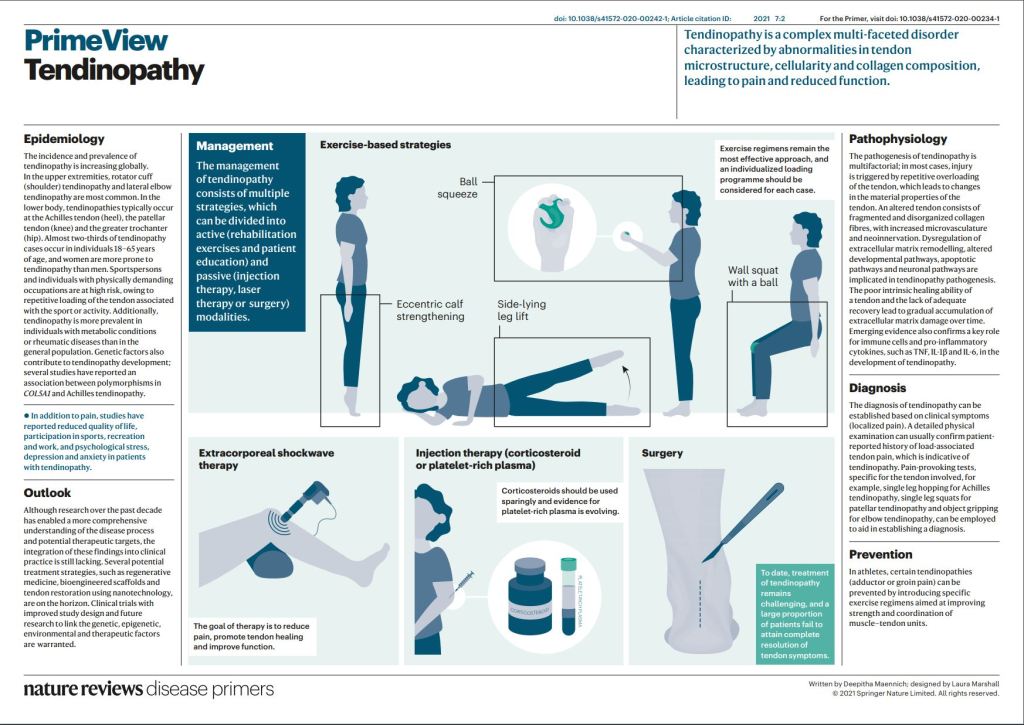
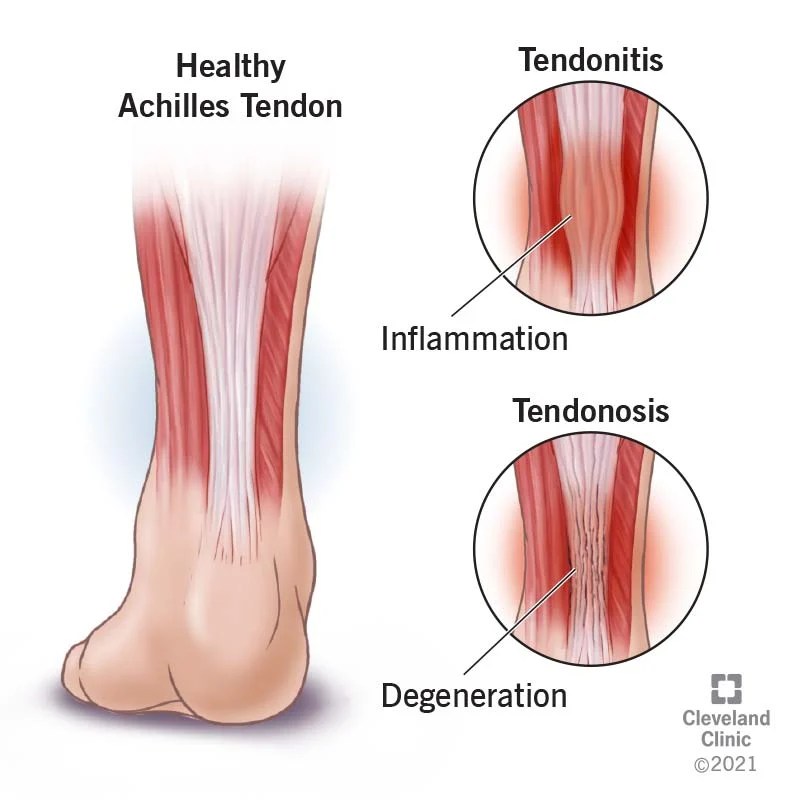
Tendinopathy is the broad term for any tendon condition that causes pain and swelling. Your tendons are rope-like tissues in your body that attach muscle to bone. When your muscles tighten and relax, your tendons and bones move. One example of a tendon is your Achilles tendon, which attaches your calf muscle to your heel bone and causes ankle movement. If you have pain and/or swelling in that area, you might have Achilles tendinopathy.
The pain from tendinopathy can interfere with your daily life. For example, it can keep you from playing sports and from doing housework. So, if you have pain or swelling, make sure to contact your healthcare provider for help.
NEWSLETTERS: TUFTS HEALTH & NUTRITION – SEPT 2022

Is That Popular Diet Plan a Healthy Choice?
Some attention and planning may be necessary to ensure popular diet plans provide enough of all the nutrients you need.
SPECIAL REPORT: Small Amounts of Physical Activity Can Have Big Benefits
Grab-n-Go Lunch
FEATURED RECIPE: Hummus and Veggie Wraps
ASK TUFTS EXPERTS: Activated charcoal; oatmeal vs. oat bran










