Breast cancer is best looked at from the historical perspective, as did Lindsay Fitzharris in the December 3, 2022 issue of the Wall Street Journal.
Can you imagine having breast cancer in the mid 1800s before the germ theory was developed? 50% of all surgeries died of severe infection at that time. Before the development of anesthesia, of course, cancer removal was extremely painful as well. Even if the patient escaped dying from infection, the one size fits all often meant removal of some chest wall muscles, leading a gaping wound.
Today, prophylactic breast imaging (mammography) often discovers the cancer at a very early and treatable stage.
Searching the cancer cells for rogue genes and surface markers often shows the way to better treatment; no longer does one size fit all.
Sometimes the breast lump is removed with minimal surgery and radiation is used, often yielding better results than the old time radical mastectomy.
Surgery itself is often aided by tissue biopsy, and now, with “intelligent” knives, gases from the surgical cut, using mass spectrophotometry, can tell the surgeon whether the tissue being cut is cancerous or normal.
Immunization methods are in development which will help your immune system to conquer any residual cancer, and “smart” T cells can be used to attack cancer cells directly.
Breast cancer Is still the most common cause of cancer deaths in women, even with all of the modern developments. Early detection is very beneficial, as with Breast self-examination and regular mammograms as prescribed by your doctor.
Extra care should be taken in families with certain genetic markers like like the BRCA gene.
—Dr. C.
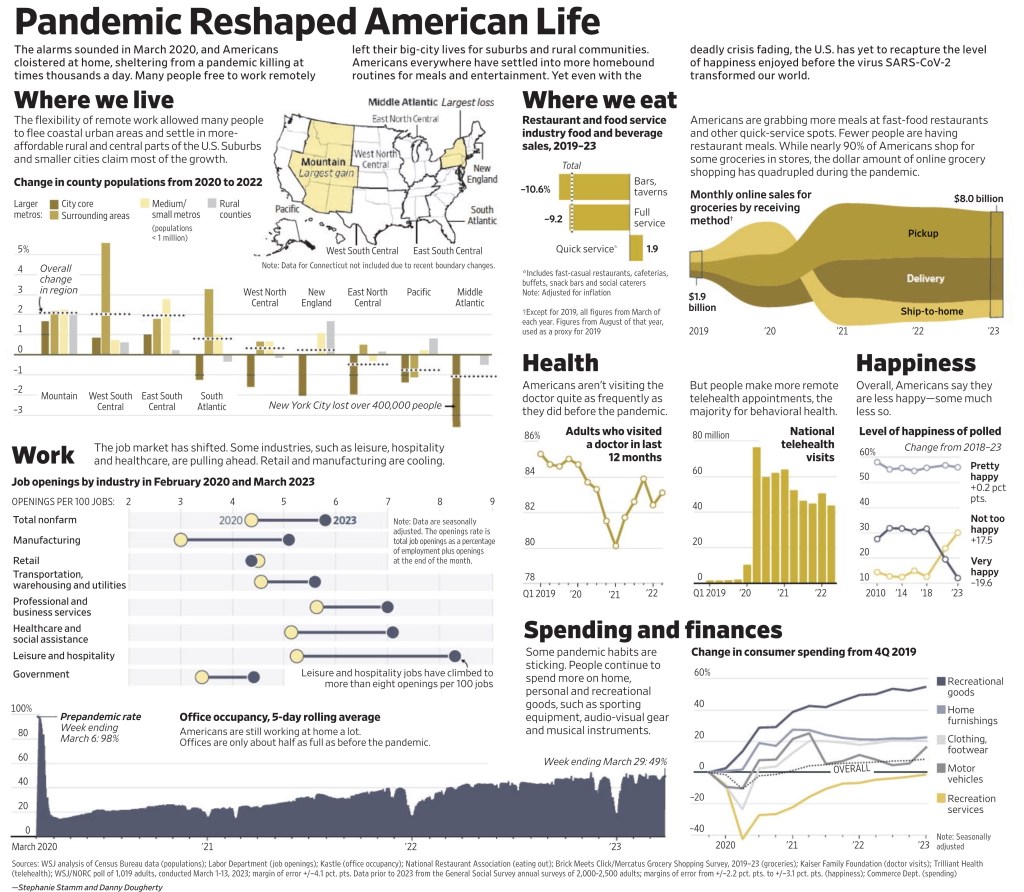
Wall Street Journal (May 5, 2023) – The alarms sounded in March 2020, and Americans cloistered at home, sheltering from a pandemic killing at times thousands a day. Many people free to work remotely left their big-city lives for suburbs and rural communities. Americans everywhere have settled into more homebound routines for meals and entertainment. Yet even with the deadly crisis fading, the U.S. has yet to recapture the level of happiness enjoyed before the virus SARS-CoV-2 transformed our world.