From a John Locke Foundation article (May 13, 2020):
A combination of stay-at-home orders, recommendations from health professionals, and the rollback of restrictive telehealth regulations boosted the use of telehealth.
….with an eye toward the future, the authors offer recommendations for all interested parties to consider moving forward. These recommendations were informed by our research and a stakeholder meeting of industry groups who work with telehealth. These groups included Doctor on Demand, the American Medical Association, and the Center for Connected Health Policy. The paper’s recommendations are as follows:
- Data on COVID-19 telehealth administration and programs must be collected and analyzed.
- Regulatory flexibility should be built into telehealth to accommodate the range of use cases.
- Telehealth services should be utilized for primary care to reduce service redundancies.
- States should be empowered to move away from parity models to reduce the cost of telehealth services.
- Telehealth services should be available to the medically underserved.
- Innovation, privacy, and data security in telehealth services should be the norm.
Read more
COMMENTARY
Telemedicine is an “almost perfect” extension of Medical Care for the Covid epidemic (1). As we ease away from Panic, we will not be abandoning distancing, cleanliness, and other personal measures that keep us well. SARS-CoV-2, or the next Pandemic Virus will be lurking in the background.
Likewise, Medicine will always embrace Telemedicine for its’ convenience, safety, and efficiency, if we can overcome the roadblocks discussed in the above article.
One efficiency in particular, discussed in the previous RPA( from Australia) article stood out; the use of Nurse-triage to direct telephone (or someday audio-visual) Patients to the most appropriate destination; ER, Urgent Care, after-hours clinic, or home care.
The Schmidtt-Thompson protocol ( which guides triage) has been used since 1980, having stood the test of time and lawyers. It is available in electronic form, and when fully automated, it should be made available without cost.
Just imagine all of the unnecessary ER visits And Physician Visits potentially saved!
Telemedicine has indeed added convenience and safety in the Era ( it seems like forever) of Covid.
There are many Telemedicine ideas that will still be used when Covid hopefully takes its’ place in the Influenza immunization vial.
—Dr. C.
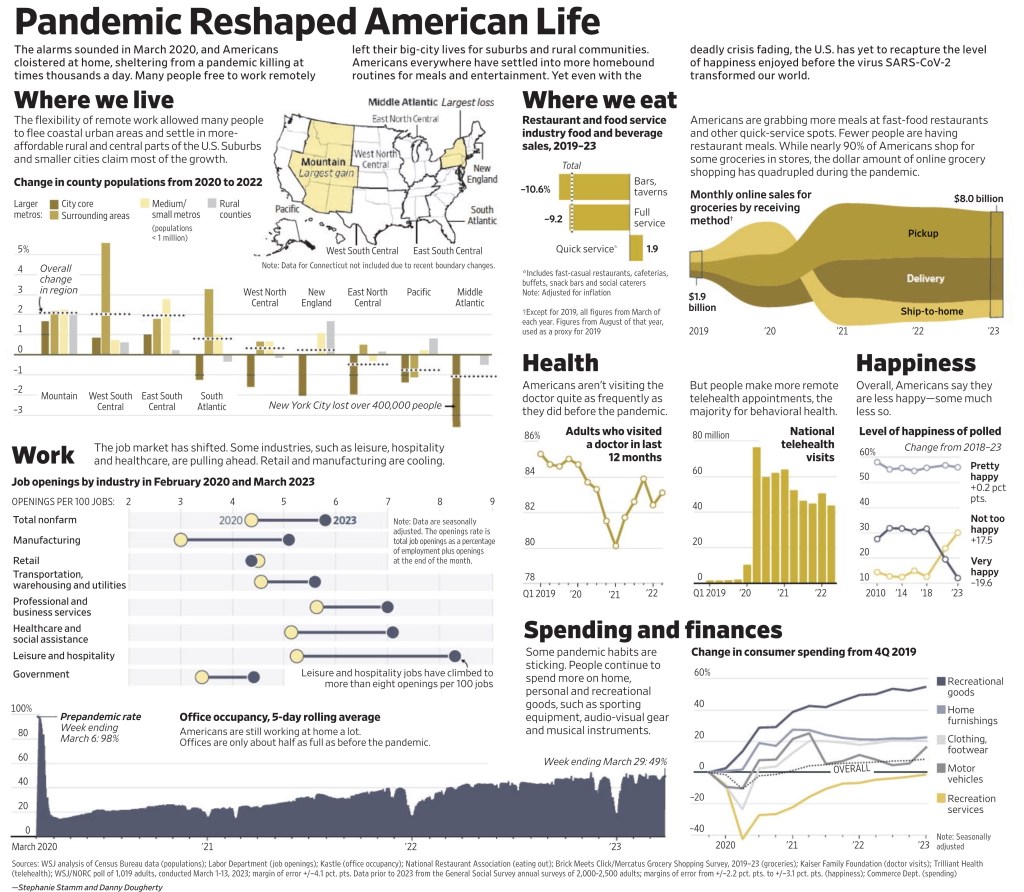
Wall Street Journal (May 5, 2023) – The alarms sounded in March 2020, and Americans cloistered at home, sheltering from a pandemic killing at times thousands a day. Many people free to work remotely left their big-city lives for suburbs and rural communities. Americans everywhere have settled into more homebound routines for meals and entertainment. Yet even with the deadly crisis fading, the U.S. has yet to recapture the level of happiness enjoyed before the virus SARS-CoV-2 transformed our world.