An explosion of advances in digital technology, imaging, gene sequencing and AI will likely transform the annual physical into an even more virtual experience https://t.co/nyuH8A6tWB
— The Wall Street Journal (@WSJ) September 6, 2021
Tag Archives: Physical Examination
THE DOCTORS 101 CHRONIC SYMPTOMS AND CONDITIONS #28: CERVICAL POLYPS
Cervical polyps are fairly common, particularly in young women who have had children. They are rare before periods start, and uncommon after menopause. Polyps are often silent, without symptoms.
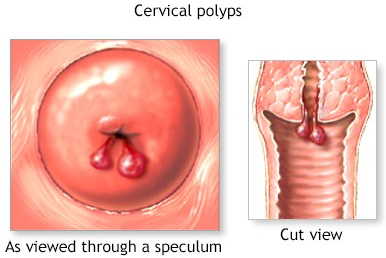
Polyps are often silent, without symptoms. Polyps are often associated with INFLAMMATION, and may be discovered because of vaginal DISCHARGE. They may bleed and betray themselves by heavy periods, or BLEEDING between periods.
My Daughter, a Student Health Physician, recently saw a patient who presented with a foul discharge and examination revealed a large polyp. A blood count showed a severe ANEMIA.
Although cancer is rare, the polyp should be biopsied or removed and examined to be sure there is no malignancy. Cervical Polyps are often discovered on a routine Physical Examination. Preventative Physical and Vaginal examinations in young women are important to check for such conditions as Polyps, do PAP smears, and, in sexually active women, screen for STDs.
–Dr. C.
TELEMEDICINE: TRANSITION TO WIDESPREAD ADOPTION

Until recently, there were several barriers preventing widespread adoption of telemedicine. The two broad themes were:
- Providers, health systems, and payers were slow to embrace change
- A failure to appreciate that telemedicine is not a new type of medicine, but rather simply a care delivery mechanism that can be utilized with some patients, some of the time, to provide high-quality care

Addressing the Telemedicine Myths
Myth 1: Telemedicine is “too hard.”
This was not true before Covid-19 and we have further demonstrated that it is not true now. Almost every provider and the great majority of patients in the U.S. already possess the technology needed to conduct a telemedicine visit — a smartphone, tablet, or computer.
It turns out that when fear of catching a potentially fatal disease strikes, telemedicine is no longer too hard.
Myth 2: Patients prioritize existing relationships with their provider over transactional episodic care.
Data argues otherwise: The majority of times, patients just want care. Falling primary care visits rates, coupled with growing emergency department and urgent care visit rates, suggests convenience as more important than an established relationship.
Myth 3. You cannot do a physical examination.
It turns out you can. A new 21st-century physical exam utilizing telemedicine emphasizes the importance of general appearance (sick or not sick, weight, distress), respiratory effort, and environmental factors including a visual assessment of the home that is not something that can be accomplished at an office visit.
The majority of times, patients just want care.
Myth 4: Virtual visits are less effective than in-person visits.
Focusing on the comparison in diagnostic accuracy between virtual and in-person visits sets up a false dichotomy. Focusing on actionable information is more important than diagnostic accuracy.2 Actionable information recognizes providers might not always make a diagnosis within a single visit, whether in-person or telemedicine.
Like every other new challenge, you have to try telemedicine to get comfortable with it.
Myth 5. There is not a payment model supporting telemedicine.
While it is true that the Centers for Medicare & Medicaid Services (pre-Covid-19) had limited reimbursement based upon site of service and geography, since the Covid-19 outbreak, to the credit of the federal government and commercial payers, telemedicine is now covered.