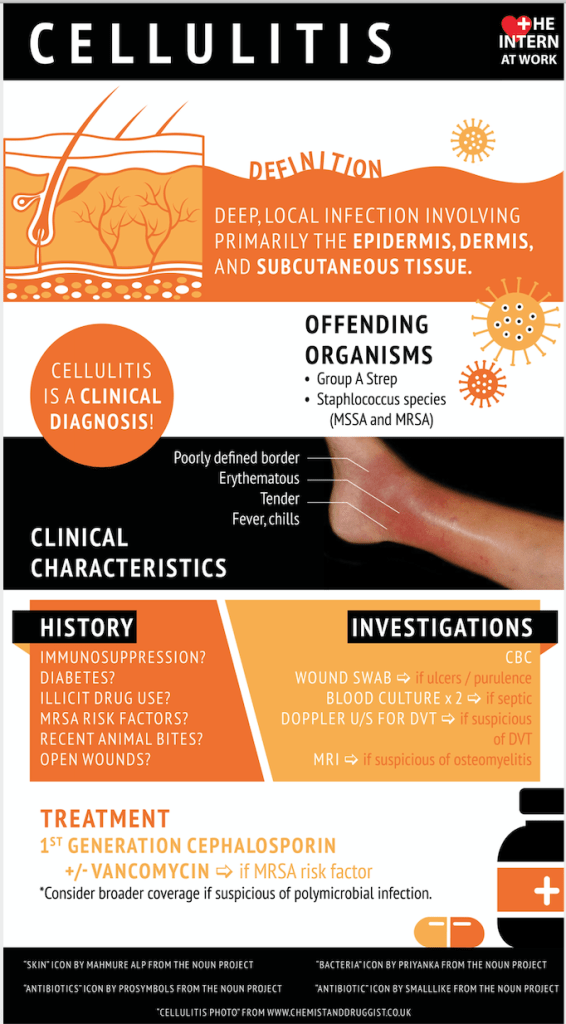
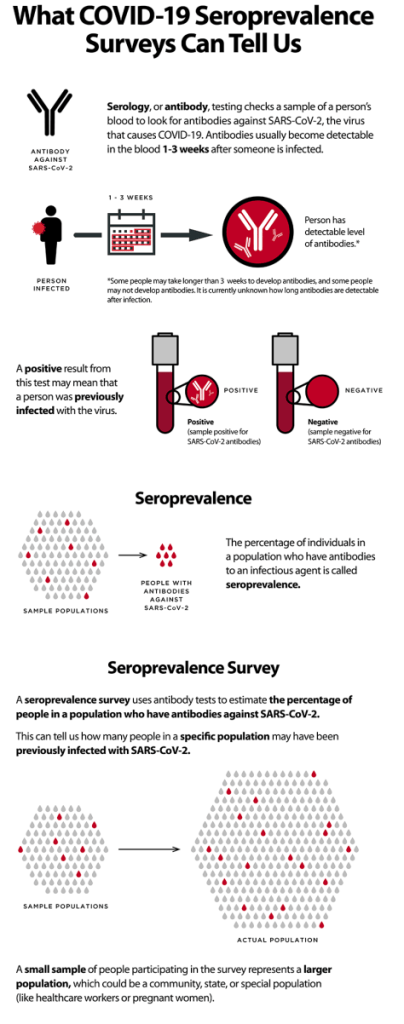
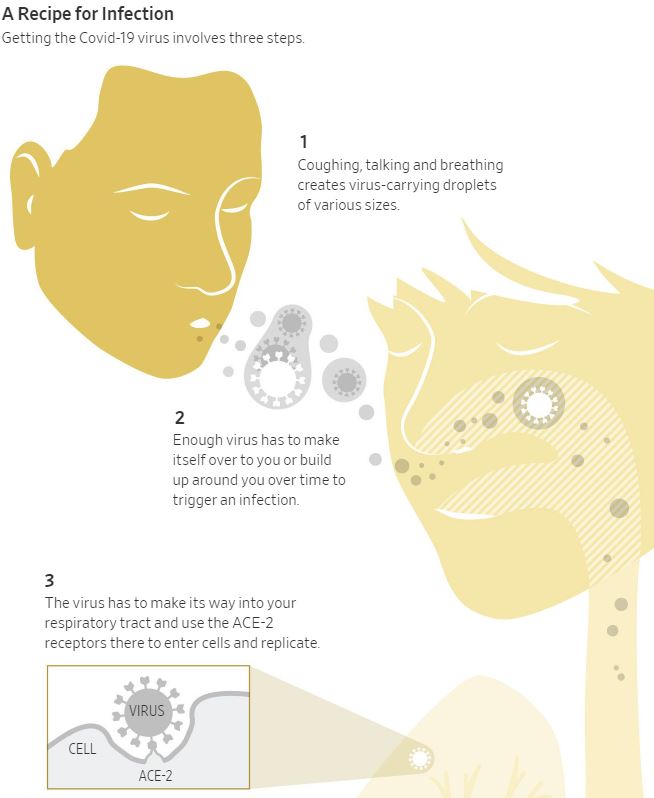
The appendix is a finger like projections at the origin of the colon in the right lower part of your abdomen. It may become inflamed, especially if there is a blockage. Appendicitis is best considered a medical emergency, since it may rupture and infect the entire abdominal cavity.
When I was a practicing pediatrician, appendicitis was one of the two conditions I refused to allow myself to overlook; the other one was meningitis, which is now mostly prevented by immunization.
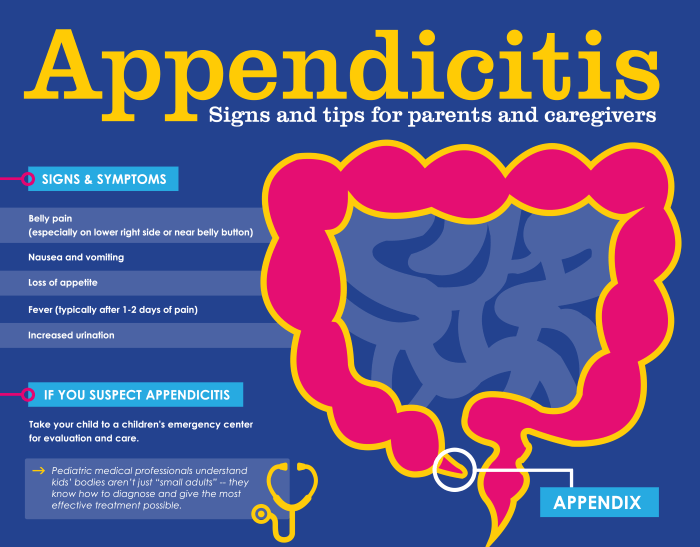
Pain in the abdomen is almost invariably present as the main symptom of appendicitis. This pain often begins around the belly button and then migrates to the right lower part of the abdomen. The patient should try to notice whether jarring the abdomen by walking makes the pain worse; if so, this finding would favor an inflammatory condition like appendicitis.
A similar condition, diverticulitis, may cause similar symptoms in the left lower part of the abdomen, and other conditions may cause confusion. The doctor checks to see if it is more painful in the right lower belly area, and she may pull her hand away suddenly. If the pain intensifies, there may be inflammation around the appendix. Sometimes a vaginal examination or rectal examination will be needed to help with the diagnosis; the appendix is close to these areas.
Other symptoms and signs may be a low-grade fever, vomiting, add an elevated white blood cell count. In the modern medical era, ultrasound, CT scans, and MRIs are sometimes used to visualize the appendix to evaluate its size and possible inflammation.
Treatment used to consist only of surgery, but with imaging techniques available to prevent disaster, the condition can be treated with antibiotics. 30 to 50% of those so treated will still eventually require surgery. Removal of the appendix is now sometimes performed through a fiberoptic scope, leading to more rapid recovery.
A dilemma is present for individuals who go to the south pole to live for several months, and where weather may prevent them from getting proper medical help. Such people may have their appendix removed as a preventative. Of course they also can take antibiotics if appendicitis develops, but it’s really scary to use medical treatment only, without the aid of modern imaging techniques.
Please consult the following Mayo clinic article for more information.