Continuing the AMA’s “Look Forward/Look Back” series, AMA CXO Todd Unger talks with Meg Barron, the AMA’s vice president of digital health strategy, about the role of telehealth post-pandemic and a new program that can help practices optimize and expand their telehealth efforts.
Tag Archives: American Medical Association
TELEMEDICINE: THE RISE OF TELEDERMATOLOGY (AMA)
From AMA.org (June 12, 2020):

“There’s an aging population, and there’s a lot of skin out there,” said Dr. Isaacs. “One in five people in the country develop skin cancer, but there is a plethora of benign skin conditions that also require the expertise of the dermatologist. So, you have increasing demand and a limited supply of dermatologists.”
A basic example of how the TPMG teledermatology program works involves a patient who is concerned about a suspicious lesion or mole on their body. The patient can take a picture of the location in question and send it to their primary care physician for review. The physician can request the patient come in for a more thorough evaluation, or if the physician determines that a dermatologist should be involved, they can send the photo to an on-call dermatologist to review.
If the patient does an in-person evaluation, the physician can also take a higher-quality image and forward that to a dermatologist. The dermatologist can then decide whether there is a problem, if a prescription is needed, or if there should be an in-person evaluation and potential biopsy.
A study in the Journal of the American Academy of Dermatology in 2019 found that when TPMG dermatologists had the chance to look at well-photographed skin lesions, they were able to identify nearly 10% more cancers with almost 40% fewer referrals to the dermatology department.
COMMENTARY
A high quality I-phone picture of a skin lesion can provide the dermatologist with 90% of the information needed for a diagnosis.
Melanoma diagnosis depends even more on the visual. In fact, Artificial Intelligence evaluation of Melanoma may be overtaking dermatologist expertise.
Size can be indicated by including a dime in the photo.
It is true that the roughness, softness or hardness may be important in diagnosis, but perhaps these characteristics could be described by the Patient.
This week, I started worrying about an itchy, rapidly growing lesion on my back. I sent a picture of this to my dermatologist, hoping he would call it a wart and reassure me. It was very regular, soft, and had a rough surface like warts I have had in the past.
However, he saw some redness and had me come in for removal. We will see what the pathology shows.
Dermatologists are in short supply, and making more efficient use of their expertise attractive.
Calling the Doctor’s office, arranging for e-mail Photo transmission, and a talk with the Doctor on the phone could save a visit. The Primary Doctor could send you directly to the dermatologist, or might be comfortable with watching and waiting.
Dermatology is indeed a field ripe for Telemedicine.
—Dr. C.
TELEMEDICINE 2020: guidance to move forward in a POST-PANDEMIC world
From a John Locke Foundation article (May 13, 2020):
A combination of stay-at-home orders, recommendations from health professionals, and the rollback of restrictive telehealth regulations boosted the use of telehealth.

….with an eye toward the future, the authors offer recommendations for all interested parties to consider moving forward. These recommendations were informed by our research and a stakeholder meeting of industry groups who work with telehealth. These groups included Doctor on Demand, the American Medical Association, and the Center for Connected Health Policy. The paper’s recommendations are as follows:
- Data on COVID-19 telehealth administration and programs must be collected and analyzed.
- Regulatory flexibility should be built into telehealth to accommodate the range of use cases.
- Telehealth services should be utilized for primary care to reduce service redundancies.
- States should be empowered to move away from parity models to reduce the cost of telehealth services.
- Telehealth services should be available to the medically underserved.
- Innovation, privacy, and data security in telehealth services should be the norm.
COMMENTARY
Telemedicine is an “almost perfect” extension of Medical Care for the Covid epidemic (1). As we ease away from Panic, we will not be abandoning distancing, cleanliness, and other personal measures that keep us well. SARS-CoV-2, or the next Pandemic Virus will be lurking in the background.
Likewise, Medicine will always embrace Telemedicine for its’ convenience, safety, and efficiency, if we can overcome the roadblocks discussed in the above article.
One efficiency in particular, discussed in the previous RPA( from Australia) article stood out; the use of Nurse-triage to direct telephone (or someday audio-visual) Patients to the most appropriate destination; ER, Urgent Care, after-hours clinic, or home care.
The Schmidtt-Thompson protocol ( which guides triage) has been used since 1980, having stood the test of time and lawyers. It is available in electronic form, and when fully automated, it should be made available without cost.
Just imagine all of the unnecessary ER visits And Physician Visits potentially saved!
Telemedicine has indeed added convenience and safety in the Era ( it seems like forever) of Covid.
There are many Telemedicine ideas that will still be used when Covid hopefully takes its’ place in the Influenza immunization vial.
—Dr. C.
TELEMEDICINE: “THE MOST COMMON USES AND HIGHEST VALUE FOR PATIENTS”
Telehealth had been gaining momentum in recent years, but the COVID-19 pandemic is propelling physician practices to quickly figure out how they can best use the technology to provide patients with care while practicing physical distancing.
(From an AMA article -April 29, 2020)
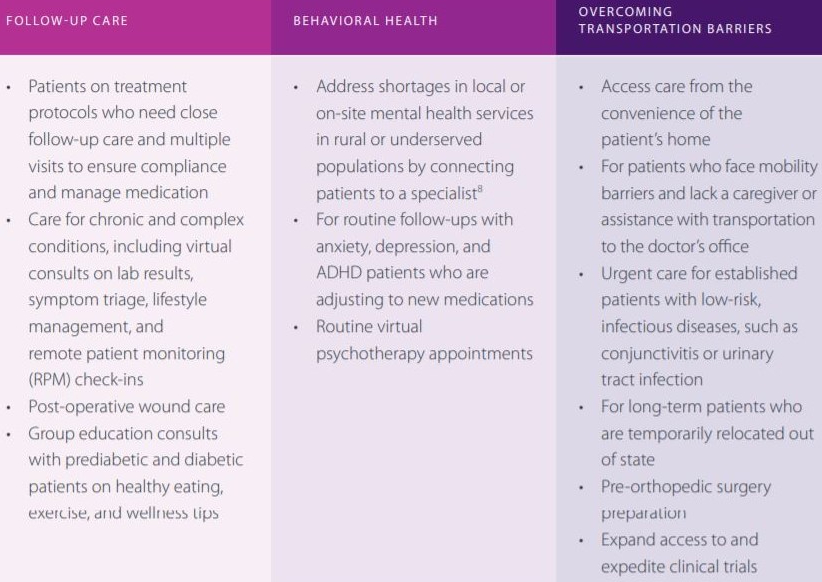
COMMON USES FOR TELEHEALTH INCLUDE: