Periprocedural risks associated with #colonoscopy aren't limited to perforation and bleeding. For patients over age 75, postcolonoscopy stroke and myocardial infarction were more common than perforation. https://t.co/nnswZQXIeH pic.twitter.com/Bel0NAJjhw
— NEJM Journal Watch (@JWatch) January 30, 2022
Tag Archives: New England Journal of Medicine
Studies: Salt Substitutes Lower Stroke, Death Risks
Telemedicine: Disruptive & Sustaining Innovation
“…telemedicine can improve through both sustaining innovation (incremental improvement upon what we are already doing for patients) and through disruptive innovation (simpler solutions for patients with simpler needs and/or patients we are not currently serving).”

Telemedicine as a Sustaining Innovation
Most telemedicine in its current form is a sustaining innovation. There has been incremental improvement in telecommunication technologies from the traditional phone to current videoconferencing software integrated with electronic medical records, development of secure platforms for short messaging service (SMS) between patients and providers, and introduction of connected devices that can monitor and transmit patients’ health data to their providers.
Disruptive Telemedicine
Beyond improving the way care is already delivered, telemedicine may also serve as a vehicle for disruption in overlooked health care markets, particularly low-end or new-market segments. Many customers are currently overserved by traditional care delivery in the form of regular visits (in-person or virtual) with a physician, which are structured to provide more than what they need and less of what they want.
2021 HEART RESEARCH: TOP FINDINGS OF CARDIOLOGISTS
Coronary artery bypass graft (CABG) was supported as superior to fractional flow reserve (FFR)–guided percutaneous coronary intervention (PCI) for three-vessel coronary artery disease (CAD). PCI failed to meet noninferiority criteria at 1-year follow-up in a study comparing outcomes between FFR-guided PCI using contemporary stents and CABG. This adds to existing evidence showing superior outcomes with CABG in patients with the most-complex CAD.
The sodium–glucose transporter-2 (SGLT-2) inhibitor empagliflozin was found to be beneficial in heart failure with preserved ejection fraction. Empagliflozin is the first medication shown to improve outcomes in this population. It’s unknown if this is a class effect of all SGLT-2 inhibitors, but this could be a game changer.
Poor-quality carbohydrates were linked to cardiovascular mortality, around the world. Consumption of higher-glycemic-index carbohydrates was associated with higher rates of cardiovascular disease and mortality in countries all around the world. These data are particularly important because lower-income countries often have diets high in refined carbohydrates, which may worsen cardiovascular disparities.
New guidelines for managing valvular heart disease were released. These new guidelines add or elevate several recommendations for transcatheter therapy, and they lower thresholds for intervention in some conditions.
The editors of Circulation: Cardiovascular Quality and Outcomes addressed racial-ethnic disparities. The editors affirmed that structural racism is a public health crisis and that the scientific publishing community can play a role in addressing it.
Tricuspid annuloplasty for moderate regurgitation during mitral-valve surgery was of unclear benefit. Annuloplasty was associated with less progression of moderate tricuspid regurgitation but more pacemakers at 2 years. Unfortunately, this mixed outcome does not clearly inform the decision on performing annuloplasty at the time of surgery, and longer-term follow-up is needed.
Immediate angiography was not beneficial in out-of-hospital cardiac arrest without ST elevation. Patients with out-of-hospital cardiac arrest who did not have ST elevation on their initial ECG did not benefit from immediate angiography. Although a potential coronary culprit was identified in about 40% of patients, neurologic injury was by far the most frequent cause of death, negating any benefit from coronary revascularization.
Many statin side effects are related to the “nocebo” effect. A creative study enrolled 60 people with statin intolerance and gave them 12 randomly ordered 1-month treatment periods: 4 periods of no medication, 4 of placebo, and 4 of statin. Symptom intensity did not differ between placebo and statin periods and, interestingly, some even had more symptoms on placebo. This demonstrates that some cases of “statin intolerance” may be related to the “nocebo” effect.
Shorter duration of dual antiplatelet therapy following PCI/stent placement was found to be acceptable in patients with high bleeding risk. A large, randomized trial found that 1 month of dual antiplatelet therapy provided similar clinical outcomes and a lower bleeding risk than 3-to-6-month regimens for this challenging patient subset.
“De-escalation” of dual antiplatelet therapy for patients undergoing PCI for acute myocardial infarction (MI). This industry-funded study evaluated patients who had received 1 month of aspirin plus ticagrelor after acute MI and stent placement and “de-escalated” half to aspirin plus clopidogrel. At 1 year, there was significantly less bleeding in the de-escalation group and a nonsignificant trend toward fewer ischemic events as well.
Covid-19: Is There Prior Infection Immunity?
Eric Rubin is the Editor-in-Chief of the Journal. Lindsey Baden is a Deputy Editor of the Journal. Stephen Morrissey, the interviewer, is the Executive Managing Editor of the Journal. E.J. Rubin, L.R. Baden, and S. Morrissey. Audio Interview: How Much Protection Does Prior SARS-CoV-2 Infection Provide?
COVID-19 VACCINES: ‘FREQUENTLY ASKED QUESTIONS ANSWERED’

How does each of the available Covid-19 vaccines work?
Once the vaccine is injected, the mRNA is taken up by the macrophages near the injection site and instructs those cells to make the spike protein. The spike protein then appears on the surface of the macrophages, inducing an immune response that mimics the way we fight off infections and protects us from natural infection with SARS-CoV-2. Enzymes in the body then degrade and dispose of the mRNA. No live virus is involved, and no genetic material enters the nucleus of the cells.
Although these are the first mRNA vaccines to be broadly tested and used in clinical practice, scientists have been working on mRNA vaccines for years. And despite this wonderful parody piece. opens in new tab saying that the technology is “obvious,” in fact the breakthrough insight that put the mRNA inside a lipid coating to prevent it from degrading is quite brilliant — and yes, this may be the first time the New England Journal of Medicine has referenced a piece in The Onion. (Last reviewed/updated on 11 Jan 2021)
How should early side effects be managed?
Analgesics and antipyretics such as acetaminophen or ibuprofen are effective in managing post-vaccine side effects including injection-site pain, myalgias, and fever. However, the CDC does not recommend prevaccine administration of these drugs, as they could theoretically blunt vaccine-induced antibody responses.
Because of the small risk of anaphylaxis, sites that administer the vaccines must have on hand strategies to evaluate and treat these potentially life-threatening reactions. The CDC has issued recommendations on how sites should prepare. opens in new tab. (Last reviewed/updated on 11 Jan 2021)
How long will the vaccines work? Are booster doses required?
Since the vaccines have been tested only since the summer of 2020, we do not have information about the durability of protection. Data from the phase 1 trial of the Moderna vaccine suggested that neutralizing antibodies persisted for nearly 4 months. opens in new tab, with titers declining slightly over time. Given the absence of information on how long the vaccines will be protective, there is currently no specific recommendation for booster doses. (Last reviewed/updated on 11 Jan 2021)
Do the vaccines prevent transmission of the virus to others?
Many commentaries on the results of the vaccine clinical trials cite a lack of information on asymptomatic infection as a limitation in our knowledge about the vaccines’ effectiveness. Indeed, this is a theoretical concern, since up to 40% of people who get infected with SARS-CoV-2 have no symptoms but may still transmit the virus to others.
Nonetheless, there are several good reasons to be optimistic about the vaccines’ effect on disease transmission. First, in the Moderna trial. opens in new tab, participants underwent nasopharyngeal swab PCR testing at baseline and testing at week 4, when they returned for their second dose. Among those who were negative at baseline and without symptoms, 39 (0.3%) in the placebo group and 15 (0.1%) in the mRNA-1273 group had nasopharyngeal swabs that were positive for SARS-CoV-2 by RT-PCR. These data suggest that even after one dose, the vaccine has a protective effect in preventing asymptomatic infection.
Second, findings from population-based studies now suggest that people without symptoms are less likely to transmit the virus to others. Third, it would be highly unlikely in biological terms for a vaccine to prevent disease and not also prevent infection. If there is an example of a vaccine in widespread clinical use that has this selective effect — prevents disease but not infection — I can’t think of one!
Until we know more, however, we should continue to emphasize to our patients that vaccination does not allow us to stop other important measures to prevent the spread of Covid-19. We need to continue social distancing, masking, avoiding crowded indoor settings, and regular hand washing. (Last reviewed/updated on 11 Jan 2021)
MEDICAL REVIEWS: COVID-19 & ‘CYTOKINE STORM’ (NEJM)
Podcast: ‘Health Policy After The 2020 Election’

Dr. Sherry Glied is dean of the New York University Wagner Graduate School of Public Service. Dr. Mark Pauly is a professor of health care management at the Wharton School of the University of Pennsylvania.
Stephen Morrissey, the interviewer, is the Executive Managing Editor of the Journal. S. Glied. Health Policy in a Biden Administration. N Engl J Med 2020;383:1501-1503. M.V. Pauly. Health Policy after a Trump Election Victory. N Engl J Med 2020;383:1503-1505.
HEALTH: “COMPRESSION THERAPY” REDUCES CHRONIC CELLULITIS & LEG EDEMA
New England Journal of Medicine (Aug 13, 2020) – In this small, single-center, nonblinded trial involving patients with chronic edema of the leg and cellulitis, compression therapy resulted in a lower incidence of recurrence of cellulitis than conservative treatment.
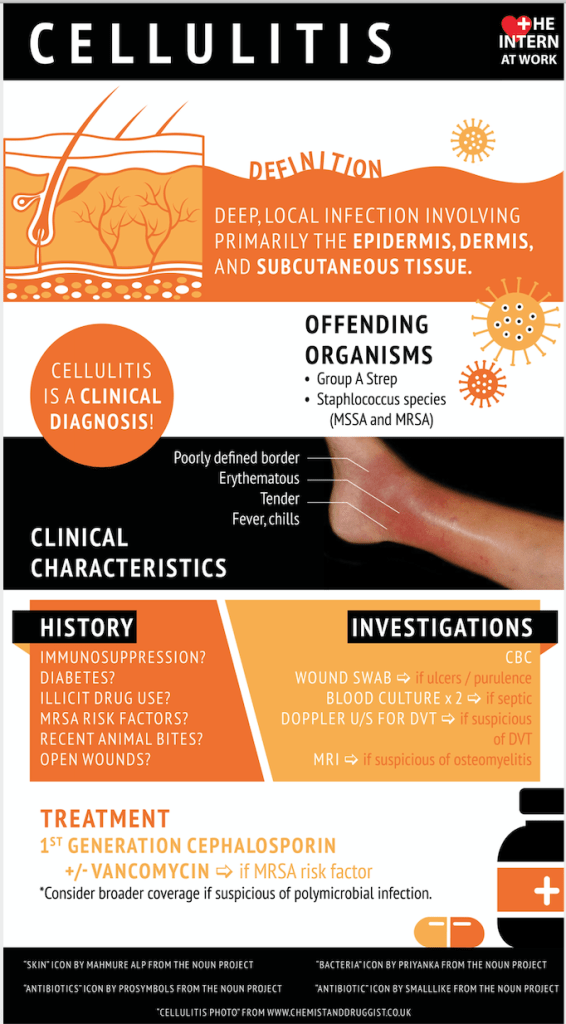
The researchers have conducted a single-center, randomized, nonblinded trial that aimed to find out an association between the compression therapy and controlled incidents of chronic edema of the leg and people with cellulitis that can be defined as an infection of the skin that involves subcutaneous tissues or the innermost layer of the skin. Cellulitis can be caused by trauma or scratching of other lesions due to animal or human bites that result in fever, extreme pain, and redness of the skin.

COMMENTARY
I have been using compression stockings for decades, since the discovery of the difference in color of my feet. An evaluation by a vascular surgeon revealed incompetence in the valve of my left popliteal vein. It wasn’t long before I developed small varicose veins.
Comfortable with PREVENTATIVE MEDICINE after a career in ALLERGY, I started wearing Jobst compression stockings, with 30-40 mm of constrictive force. After a decade or so of daily wearing, my big toes started to overlap my second toes, and I began using toe-spreaders; scissor-toe and hammer-toe were my worry, and I wanted to prevent this discomfort.
After a while, I began to notice that the Jobst stockings tended to bunch my toes together. Also, with the developing arthritis in my fingers, it was increasingly hard to get the 30-40mm stockings on without straining my arthritic hands. I now wear OPEN-TOE 15-20mm compression Medi stockings, which are easier to get on, and don’t bunch up my toes.
I still use the visco-elastic toe spreaders. Now, back to the compression stockings for treatment of cellulitis complicating ankle swelling. Of course it works. Beta Hemolytic Streptococci and Staph aureus like nothing better to feed on than a warm pool of interstitial fluid, which is the juice that comprises the ankle swelling.
And BLOOD CLOTS tend to form in the stagnant pools of blood which aggregates in varicose veins, particularly when you are sitting for a long time, such as during a long airline trip. By all means, use compression stockings if you have ankle edema, or even a condition predisposing to ankle edema like varicose veins. Don’t wait for the complication to develop. Be PROACTIVE, and STAY HEALTHY.
–DR. C
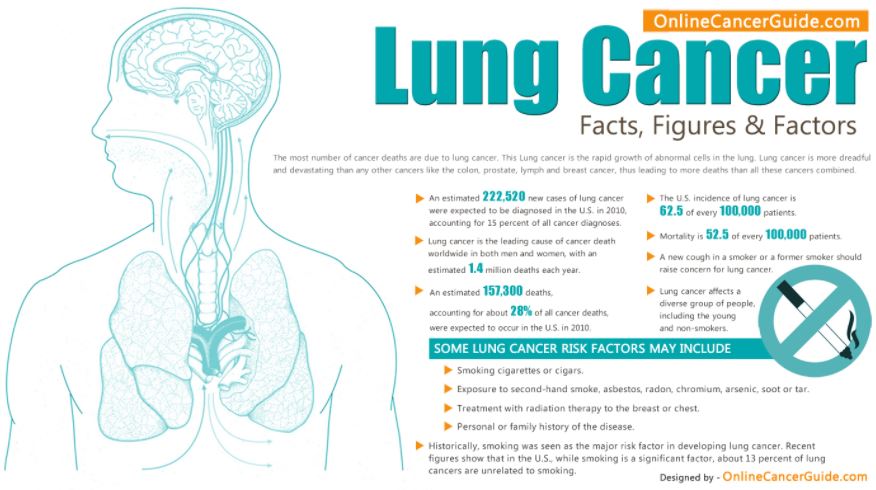
MEDICINE: LUNG CANCER DEATHS DROP AS TARGETED THERAPIES IMPROVE (NEJM)
NEJM (Aug 13, 2020) – Population-level mortality from NSCLC in the United States fell sharply from 2013 to 2016, and survival after diagnosis improved substantially. Our analysis suggests that a reduction in incidence along with treatment advances — particularly approvals for and use of targeted therapies — is likely to explain the reduction in mortality observed during this period.
“The survival benefit for patients with non-small cell lung cancer treated with targeted therapies has been demonstrated in clinical trials, but this study highlights the impact of these treatments at the population level,” said Nadia Howlader, Ph.D., of NCI’s Division of Cancer Control and Population Sciences, who led the study. “We can now see the impact of advances in lung cancer treatment on survival.”