
Monthly Archives: September 2022
Technology: How AI Can Improve Diagnostics (GAO)
Each year, medical diagnosis errors affect the health of millions of Americans and cost billions of dollars. Machine learning technologies can help identify hidden or complex patterns in diagnostic data to detect diseases earlier and improve treatments.
Several machine learning (ML) technologies are available in the U.S. to assist with the diagnostic process. The resulting benefits include earlier detection of diseases; more consistent analysis of medical data; and increased access to care, particularly for underserved populations. GAO identified a variety of ML-based technologies for five selected diseases
- Certain cancers,
- Diabetic retinopathy,
- Alzheimer’s disease,
- Heart disease,
- COVID-19
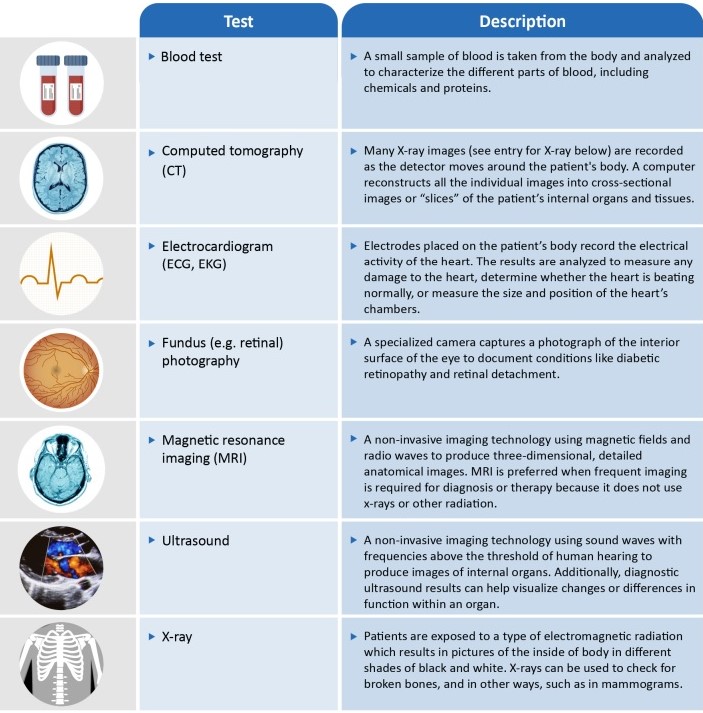
Most technologies relying on data from imaging such as x-rays or magnetic resonance imaging (MRI). However, these ML technologies have generally not been widely adopted.
Cervical Cancer: Its Risks, Symptoms & Treatment
Learning about cervical cancer can be intimidating. Kristina Butler, M.D., a gynecologic oncologist at Mayo Clinic, walks you through the facts, the questions, and the answers to help you better understand this condition.
Video timeline: 0:00 Introduction 0:38 What is cervical cancer? 1:16 Who gets cervical cancer? / Risk factors 2:23 Symptoms of cervical cancer 3:03 How is cervical cancer diagnosed? 4:26 Treatment options 5:20 Coping methods/ What now? 6:10 Ending
Glaucoma: The Risks Of Ocular Hypertension
Often described as the silent thief of sight, glaucoma is the most common cause of irreversible blindness in the world. High pressure in the eye damages the optic nerve, first stealing peripheral vision (what you see at the corners of your eyes) and later harming central vision (what you see when looking straight ahead). Usually, people notice no symptoms until vision loss occurs.
Lowering high eye pressure is the only known treatment to prevent or interrupt glaucoma. But does everyone with higher-than-normal eye pressure need to be treated? A major long-term study provides some clues, though not yet a complete answer.
Does everyone with high eye pressure develop glaucoma?
In the US, glaucoma affects an estimated three million people, half of whom do not know that they have it. An ophthalmologist can perform a comprehensive eye exam to determine if someone has glaucoma, or is at risk for developing it in the future due to high eye pressure (ocular hypertension). Research from the long-running Ocular Hypertension Treatment Study (OHTS) shows that some people with high eye pressure may never develop glaucoma, while others will.
Prostate Cancer: Seven Top Questions Answered
Mitchell Humphreys, M.D., a urologist at Mayo Clinic, answers the important questions you may have about prostate cancer.
Video timeline: 0:00 Introduction 0:16 How do you know how fast my cancer is growing? 0:49 Is prostate cancer sexually transmitted? 1:04 Is prostate cancer hereditary? 1:36 What can I do to prevent or slow prostate cancer? 2:03 Is there a risk of cancer spreading if I have a biopsy of my prostate? 2:20: When should I stop screening for prostate cancer? 2:46 How can I be the best partner to my medical team? 3:12 Ending
Get informed: https://mayocl.in/3Sk7lJE.
DOCTORS PODCAST: MEDICAL & TELEHEALTH NEWS (SEP 25)
A weekly podcast on the latest medical, science and telehealth news.
Medicine: Adult-Onset Autoimmune Diabetes
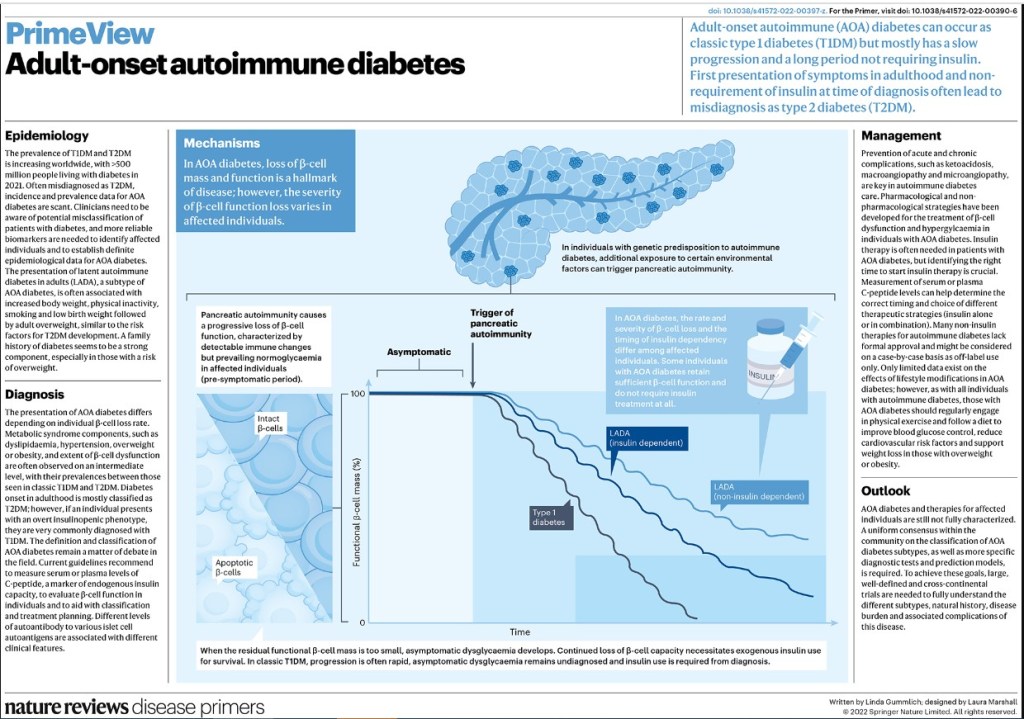
- Adult-onset autoimmune diabetes encompasses a wide spectrum of heterogeneous genotypes and phenotypes, ranging from classic adult-onset type 1 diabetes mellitus to latent autoimmune diabetes in adults (LADA)
- The heterogeneity of LADA arises from its definition as being present in any adult with diabetes who does not require insulin and who is positive for any islet autoantibody, regardless of titre, number or epitope specificity
- The heterogeneity of LADA manifests in different clinical phenotypes, ranging from prevalent insulin resistance to prevalent insulin deficiency, each of which might be associated with different autoimmune and metabolic markers
- Although patients with LADA are leaner and have healthier lipid and blood pressure profiles, evidence shows that there is no difference in cardiovascular outcomes between these patients and those with type 2 diabetes mellitus
Medicine: Using Stem Cells To Treat Osteonecrosis
Daniel Wiznia, MD, an orthopaedic surgeon with Yale School of Medicine, is practicing a surgical technique designed to render 10% of hip replacements unnecessary. Regenerative properties from a patient’s own stem cells are responsible for regrowing bone, restoring blood flow, and being able to avoid further interventional surgery.
Osteonecrosis, also known as avascular necrosis, occurs in more than 20,000 Americans each year. As the condition progresses, bone cells known as osteoblasts become unable to repair themselves and sustain the integrity of the bone, and ultimately die. The bone deterioration leads to a decrease in blood flow to the area, further weakening the entire skeletal structure of the upper leg.
If unaddressed, the ball portion of the hip’s ball and socket joint will cave in on itself and collapse, requiring a total hip replacement. The fact that patients often receive this diagnosis during their 30s and 40s presents a particular challenge.
While the lifespan of hip prosthetics has dramatically increased in recent years, a patient who undergoes a total hip arthroplasty, or total hip replacement, at that age will almost certainly require a revision later in life. This redo of the same surgery at an older age comes with an entirely new set of risks and potential complications, making it that much harder to manage down the road.
Blood Pressure: What Is Hypertension? (Video)
Learning about hypertension can be intimidating. Leslie Thomas M.D., a nephrologist at Mayo Clinic, walks you through the facts, the questions, and the answers to help you better understand this condition.
Video timeline: 0:00 Introduction 0:39 What is hypertension? 1:13 Who gets hypertension? / Risk factors 2:18 Symptoms of hypertension 2:36 How is hypertension diagnosed? 3:14 Treatment options 3:51 Coping methods/ What now? 4:05 Ending
COMMENTARY:
Hypertension is an elevation of the blood pressure in the arteries. It is measured conventionally by blood pressure cuffs, although a catheter in the artery is more accurate. I’ve had my blood pressure taken countless numbers of times by nurses and doctors who sometimes put the cuff on my arm through a piece of clothing, making it less accurate. Sometimes it is taken by an automatic blood pressure cuff even in the doctors office. The automated cuff can be purchased for $20 or less for you to use it at home, but it’s accuracy is questionable when you have an irregular heartbeat with atrial fibrillation such as I do.
The blood pressure reading which is considered to be normal Is dropping. In the present video, following 2017 guidelines , they state that a systolic reading of more than 120 mmHg is elevated, and anything more than 130 is hypertension. It may be true that studies have been done to show that these slight elevations cause problems, but so can the drugs that are used to lower blood pressure; a cough can be caused by ACE inhibitors. Fatigue and fainting can be caused by an excessive dosage of any blood pressure medication.
Healthy diet, especially avoiding extra salt, Regular exercise and good sleep will go a long way towards keeping your blood pressure at 120 or below on the high reading (systolic), and 80 on the low reading (diastolic).
My systolic blood pressure varies between 120 and 140 systolic, and is usually around 60 diastolic. For a long time I thought the relatively low (diastolic) blood pressure was more important, since diastole is of greater duration than systole, but it has now been determined that the systolic blood pressure reading is the one to worry about. Calcification and lack of elasticities in the arteries as you get older can lead to higher systolic blood pressure.
It used to be thought that the normal systolic blood pressure was 100+ your age in years. Those days are gone, however, and greater life expectancy and health Is one result of carefully monitoring your blood pressure, and working hard to keep it down.
Please refer to the Mayo Clinic article to give you (much) more information.
—Dr. C.
Dr. C’s Journal: What Is Achilles Tendinitis?
The Achilles tendon, or “heel cord”, connects your calf muscle to the heel. Overuse can inflame the tendon, or even tear or rupture it, causing a lot of pain.
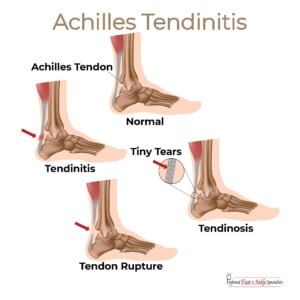
Sudden increases in intensity of exercise can be a cause. It is more common in men, and as you get older. Running a lot in the soft sand of the beach has caused problems in many of my friends. Achilles tendinitis can be caused by certain antibiotics, such as fluoroquinolones.
Varying your type of exercise, or cross training, distributes the strain you put on your body and decreases the likelihood of Achilles tendinitis. Swimming comes to mind with any disturbance of your lower extremities. The pool in which I swim three days a week is disparagingly called the “injured reserve pool” in my community Stretching before exercising is always a good idea. Pick a routine and stick with it, particularly as you get older. If you have flat feet, getting a slight lift for the heel may help to take tension off the Heel cord, and orthotics may help. Getting expert advice is always advisable.
Prevention is always far better than treatment.
If a short period of rest doesn’t get rid of the pain, check with your Doctor, who might examine the tendon, take x-rays, or order ultrasounds to check the extent of the difficulty.
—Dr. C.











