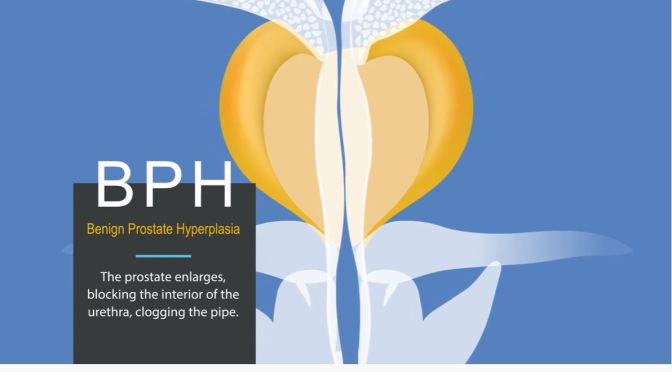
Trouble Urinating? There are many common causes for urinary issues in men. Learn about symptoms and treatment options offered by The Johns Hopkins Brady Urological Institute. https://www.hopkinsmedicine.org/brady…
Monthly Archives: May 2021
DOCTORS PODCAST: MEDICAL & TELEHEALTH NEWS (MAY 30)
A weekly podcast on the latest medical, science and telehealth news.
Technology: Robotically Assisted Heart Surgery
Robotically assisted heart surgery is a minimally invasive option most often used for mitral valve repair. Cleveland Clinic cardiothoracic surgeons explain how it works and what to expect.
Telehealth: Government & Regulatory Issues (Video)
In response to the COVID-19 pandemic, governments across the United States relaxed restrictions on telemedicine, allowing more patients to receive healthcare remotely than ever before. This development brought a number of questions about how telehealth should be regulated to the fore. Is remote care as effective as in-person care? Would long-turn expansion of telemedicine reduce costs for patients and healthcare providers? Might a greater reliance on telehealth actually reduce access to care for some patients?
HEALTH: HOW DEPRESSION AFFECTS THE BRAIN (YALE)
For many people, depression turns out to be one of the most disabling illnesses that we have in society. Despite the treatments that we have available, many people are not responding that well. It’s a disorder that can be very disabling in society. It’s also a disorder that has medical consequences.
By understanding the neurobiology of depression we hope to be able more to find the right treatment for the patient suffering from this disease. The current standard of care for the treatment of depression is based on what we call the monoamine deficiency hypothesis. Essentially, presuming that one of three neurotransmitters in the brain is deficient or underactive. But the reality is, there are more than 100 neurotransmitters in the brain. And billions of connections between neurons. So we know that that’s a limited hypothesis. Neurotransmitters can be thought of as the chemical messengers within the brain, it’s what helps one cell in the brain communicate with another, to pass that message along from one brain region to another. For decades, we thought that the primary pathology, the primary cause of depression was some abnormality in these neurotransmitters, specifically serotonin or norepinephrine. However, norepinephrine and serotonin did not seem to be able to account for this cause, or to cause the symptoms of depression in people who had major depression. Instead, the chemical messengers between the nerve cells in the higher centers of the brain, which include glutamate and GABA, were possibilities as alternative causes for the symptoms of depression. When you’re exposed to severe and chronic stress like people experience when they have depression, you lose some of the connections between the nerve cells. The communication in these circuits becomes inefficient and noisy, we think that the loss of these synaptic connections contributes to the biology of depression. There are clear differences between a healthy brain and a depressed brain. And the exciting thing is, when you treat that depression effectively, the brain goes back to looking like a healthy brain, both at the cellular level and at a global scale. It’s critical to understand the neurobiology of depression and how the brain plays a role in that for two main reasons. One, it helps us understand how the disease develops and progresses, and we can start to target treatments based on that. We are in a new era of psychiatry. This is a paradigm shift, away from a model of monoaminergic deficiency to a fuller understanding of the brain as a complex neurochemical organ. All of the research is driven by the imperative to alleviate human suffering. Depression is one of the most substantial contributors to human suffering. The opportunity to make even a tiny dent in that is an incredible opportunity.
Cancers: What Is Multiple Myeloma? (Mayo Clinic)
Multiple myeloma is a relatively uncommon form of blood cancer that affects less than 1% of the U.S. population, according the American Cancer Society. People younger than 45 rarely get the disease, and it occurs more in older men than women. And your risk is doubled if you’re African American.
Osteoporosis: Study Finds Up To 40% Greater Risk Of Hearing Loss In Women

As part of the Conservation of Hearing Study (CHEARS), researchers from Brigham and Women’s Hospital analyzed data from nearly 144,000 women who were followed for up to 34 years. They found that risk of subsequent moderate or worse hearing loss was up to 40 percent higher in study participants with osteoporosis or LBD. The study, published in the Journal of the American Geriatric Society, also found that bisphosphonates did not alter risk of hearing loss.
The researchers found that a history of vertebral fracture was associated with up to a 40 percent higher risk of hearing loss, but the same did not hold true for hip fractures, the two most common osteoporosis-related fractures. “The differing findings between these skeletal sites may reflect differences in the composition and metabolism of the bones in the spine and in the hip,” Curhan said. “These findings could provide new insight into the changes in the bone that surrounds the middle and inner ear that may contribute to hearing loss.”
DR. C’S JOURNAL: BENEFITS OF PARATHYROID HORMONE
Hormones, Vitamins, and minerals all have extensive interactions in the give-and-take of the bodies’ ballet of homeostasis. No where is this more clear-cut than the interplay of parathyroid hormone, vitamin D, and calcium.

Although it has many other actions in the body, calcium is best known as the prime component of our bones. It is essential for making them healthy and strong. The bones act as a storehouse or vault for the bodies calcium. The parathyroid hormone is the key that unlocks the vault to release the calcium so it can perform its many other roles in the body. An elevation of the calcium in the blood stream shuts down the parathyroid Glands.
Parathyroid hormone also acts to instruct the body to absorb more vitamin D, just as the vitamin D causes the intestinal tract to absorb more calcium. The parathyroid glands are in the upper poles of the thyroid which as we mentioned before sits astride the windpipe.
Sometimes the parathyroid gland develops an adenoma which causes too much secretion of parathyroid hormone.
This results in an excess of calcium in the body and a variety of symptoms, such as joint pain muscle weakness, fatigue, nausea and vomiting. One of the technicians in my medical practice developed hyperparathyroidism. It was detected by a metabolic panel, which showed an elevation of serum calcium.
This discovery, early in my practice, made me a big fan of metabolic panels when patients have general symptoms. Her condition, a parathyroid adenoma, was cured by surgery. Conversely, surgery for an overactive thyroid can sometimes accidentally remove the parathyroid glands if the surgeon isn’t careful. The parathyroid glands are tiny, but they perform a huge function.
—Dr. C.
THE DOCTORS 101 CHRONIC SYMPTOMS & CONDITIONS #40: HYPOTHYROIDISM
Hypothyroidism is a very common hormonal deficiency where there is an insufficient amount of thyroid hormone, T4. The thyroid gland regulates your metabolic activity. If you have insufficient thyroid hormone, everything seems to slow down; Your energy level, your muscle strength, your heart rate, your brain activity, and even your intestinal activity are all slower.
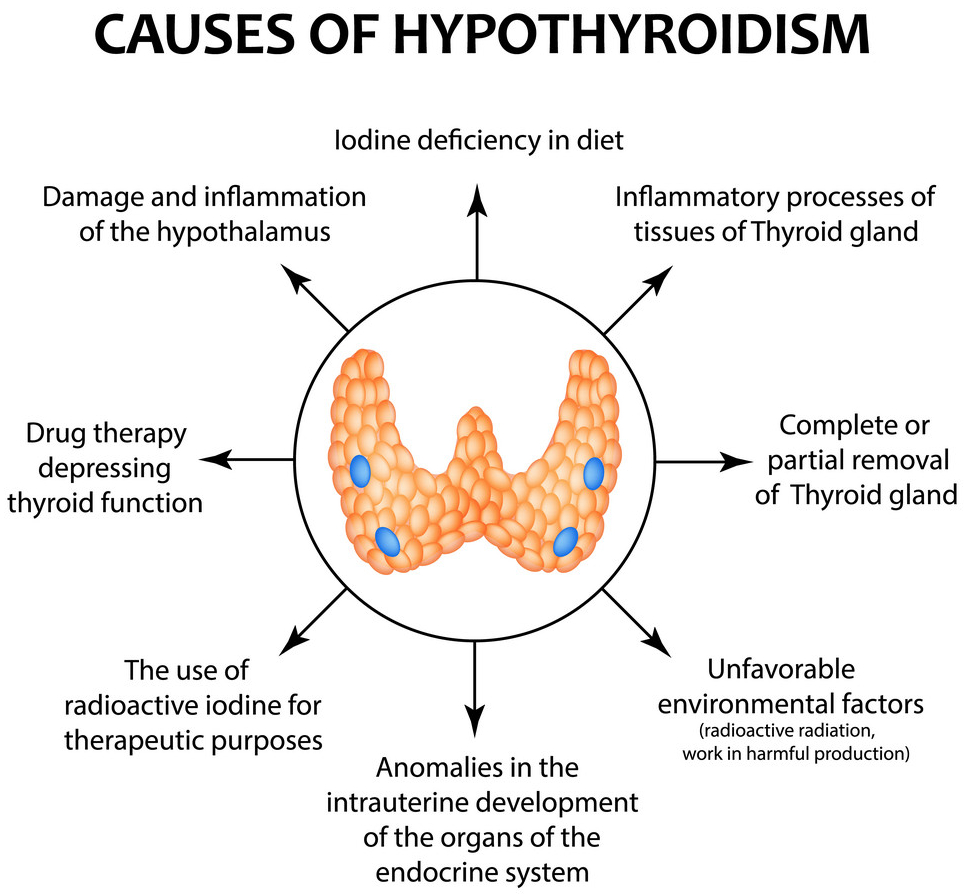
One of my habits in practice was to check the size of the thyroid, which is an H shaped gland astride the windpipe beneath the voice box. It becomes enlarged in a condition known as Hashimoto’s thyroiditis, the most common cause of adult hypothyroidism.
As you recall from the last posting, when the thyroid function is low, the brain causes a release of TSH, which stimulates the thyroid gland. In order to produce more thyroid hormone, the gland enlarges and the examining physician can feel it.
Babies can be born without a thyroid. I had one such patient when I was in training. The baby was inexplicably limp, and did not cry vigorously like other babies. When given thyroid hormone, she developed normally. Such babies often go undetected, don’t grow and become mentally deficient.
The thyroid gland produces thyroxine, which is T4. In the tissues, the T4 is converted into the much more active T3. This is often the medication of choice in hypothyroidism. In giving thyroid Hormonal, the physician must adjust the dose, depending on the patients response. Only after a number of visits is the proper dose found.
Please refer to the Mayo clinic article on hypothyroidism. The use of the TSH as a blood test is also discussed.
—Dr. C.
DR. C’S JOURNAL: THYROID STIMULATING HORMONE
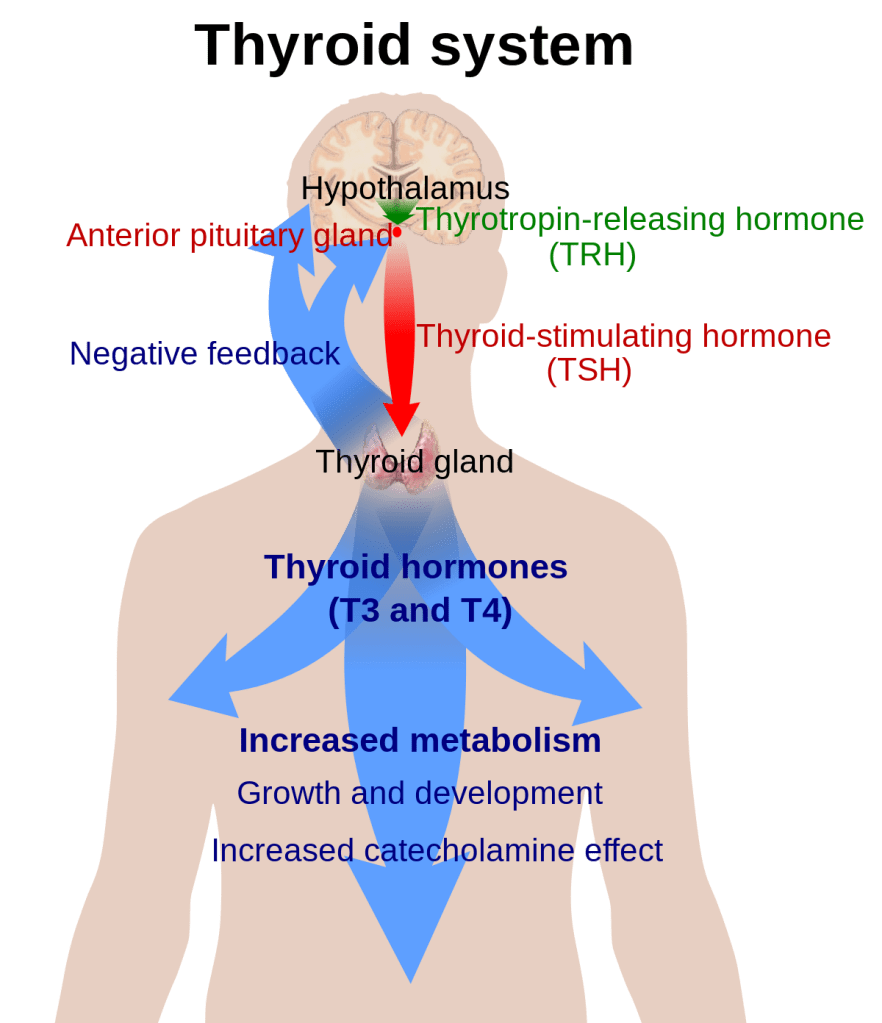
Thyroid stimulating hormone (TSH) is one of a series of regulatory hormones to come from the pituitary gland, often called the “master gland“ of the body. Most of the pituitary hormones are released upon signals from the hypothalamus, part of the real master coordinator of the body, the brain.
TSH Instructs the Thyroid gland to produce more Thyroid hormone. When more Thyroid hormone is produced, The increase of Thyroxin in the bloodstream causes the TSH level to drop.
Our metabolism is full of these servomechanisms which control the level of critical substances. When the thyroid does not function properly, and the thyroid level drops, the TSH is increased. An elevated TSH it is presently the best test we have for hypothyroidism.
Conversely, when there is excessive thyroid activity (hyperthyroidism), the TSH level drops to vanishingly low amounts. Tomorrow the subject will be thyroxin.