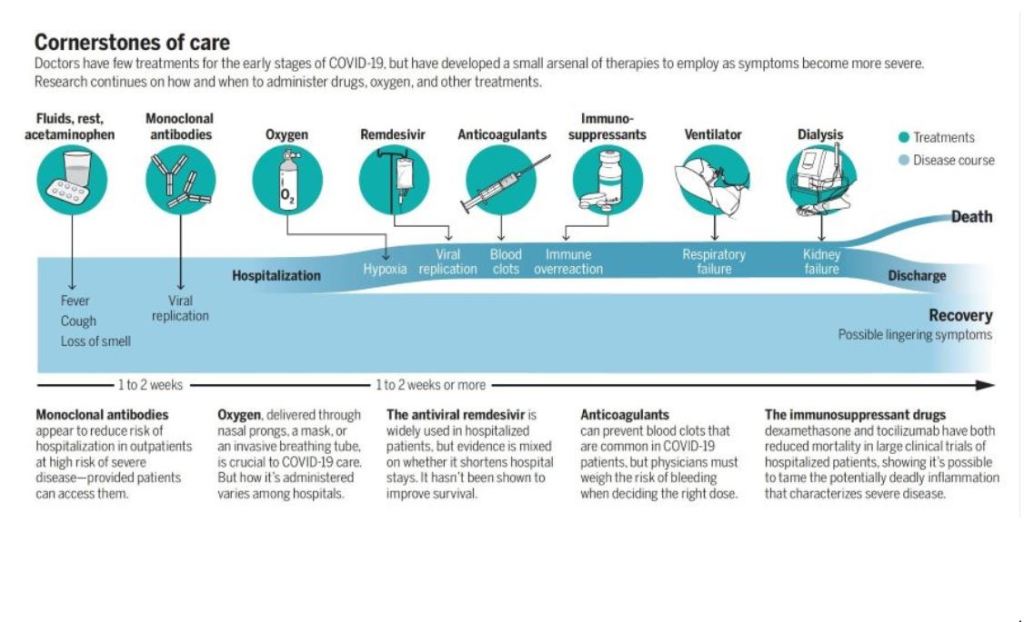
The idea is to deliver into the body bits of proteins, or antigens, from cancer cells to stimulate the immune system to attack any incipient tumors. The concept isn’t new, and it has faced skepticism. A decade ago, a Nature editorial dismissed a prominent breast cancer advocacy group’s goal of developing a preventive vaccine by 2020 as “misguided,” in part because of the genetic complexity of tumors. The editorial called the goal an “objective that science cannot yet deliver.” But now, a few teams—including one funded by the same advocacy group, the National Breast Cancer Coalition (NBCC)—are poised to test preventive vaccines, in some cases in healthy people at high genetic risk for breast and other cancers.
Tag Archives: Science Magazine
Brain Research: The Many Benefits Of Healthy Sleep
Covid-19 Review: Airborne Transmission Of Viruses
In a very good article, the Journal ‘Science’ has collated a lot of basic science regarding aerosol transmissions in viral infection generally, and Covid-19 in particular.

Early in the epidemic, I thought that large droplet transmission, which fell to the floor, and was transmitted by fomites and hand autoinoculation into the respiratory membranes, was more important. The main thesis of the article is that it is not large droplets, but aerosol particles that mainly transmit.
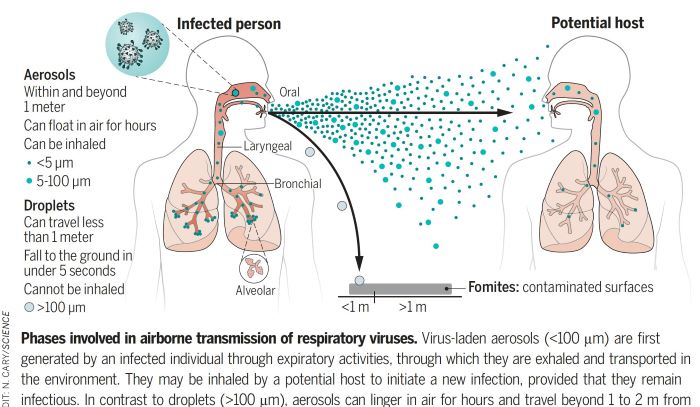
The secondary assertion is that aerosols can be up to 100 µm microns in diameter and still be transmitted by inhalation. they also stated that particle size of equal or less than 5 µm contain more virus particles than all the larger particles put together in spite of the greater mass of the larger particles . Normal speaking creates about 1000 aerosol particles per minute, And normal breathing about 7200 aerosol particles per liter of exhaled air. Coughing is more sporadic and tends to produce the larger droplets which don’t stay airborne as long, but I wouldn’t count on it.
There is a tremendous difference between individuals as to the number of particles they generate. It’s estimated that 10 to 20% of individuals account for 80 to 90% of the virus.
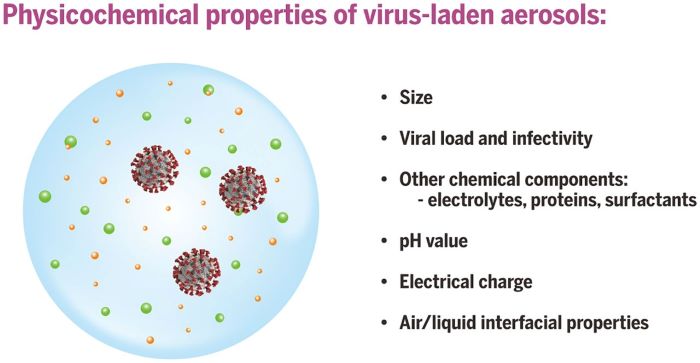
Slide number two deals with viral load and infectivity which is a function of the pH value, electrical charge, and other characteristics of the virus. An important point is that even though there is lots of viral RNA, that doesn’t mean that the virus is infective. Once again there’s a tremendous difference between the infective viable virus content of the aerosols from infected patient to patient. He stated that in one room with two Covid patients, they were 6 to 74 TCID/50 per liter, which means you’re almost certain to be infected if you don’t have a mask that filters out the virus, or some kind of purification in the room.
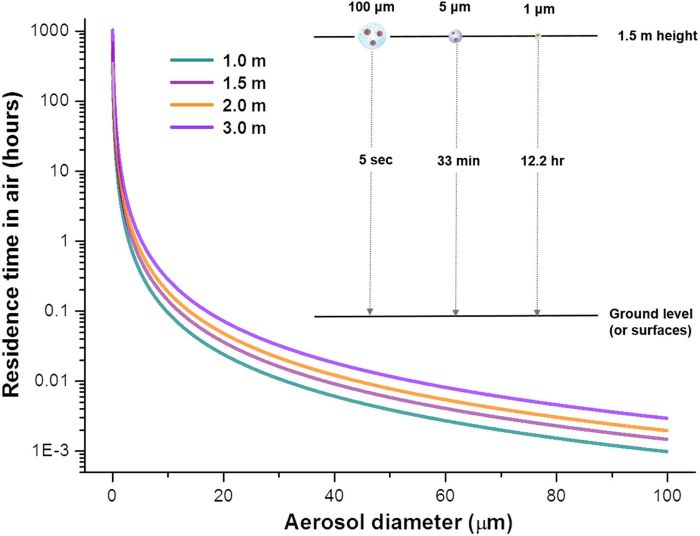
Slide Three was very interesting to me. The persistence in hours graphed against the aerosol particles size. 100 µm particles stay in the air only about five seconds, 5 µm particles stay in the air for 30 minutes, and one micrometer particles will stay in the air for 12 hours or more.
The fourth slide talks about factors affecting the distribution of indoor aerosols. There may be certain parts of the room where the particles congregate , depending on the ventilation type, whether natural, mechanical or filtered, flow patterns within the room, and indoor filtration and killing devices such as ultraviolet light.
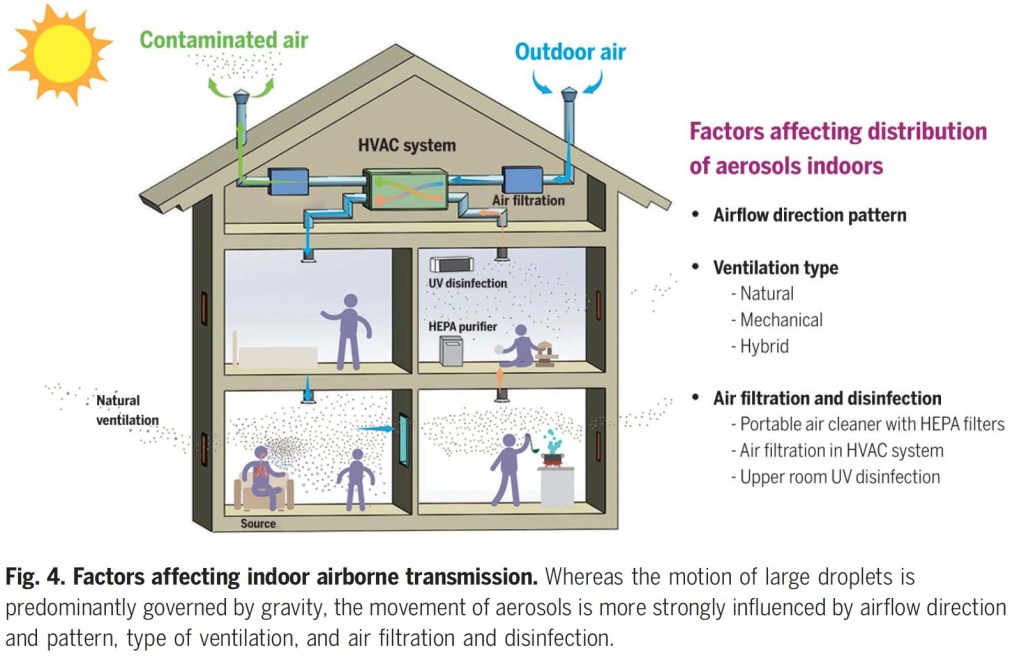
Mention is made of the CO2 level in the room as a measure of air circulation. There is a higher CO2 in the air with lots of people and poor ventilation. The recommendation is that 7-8 ppm is about the highest acceptable level, and the possibility of using a portable HEPA filter would not be a bad idea for people frequenting indoor restaurants. Of course, outdoor air with its breezes, dispersion, less humidity, higher ultraviolet and usually Greater dispersion of people is preferable to indoor contact.
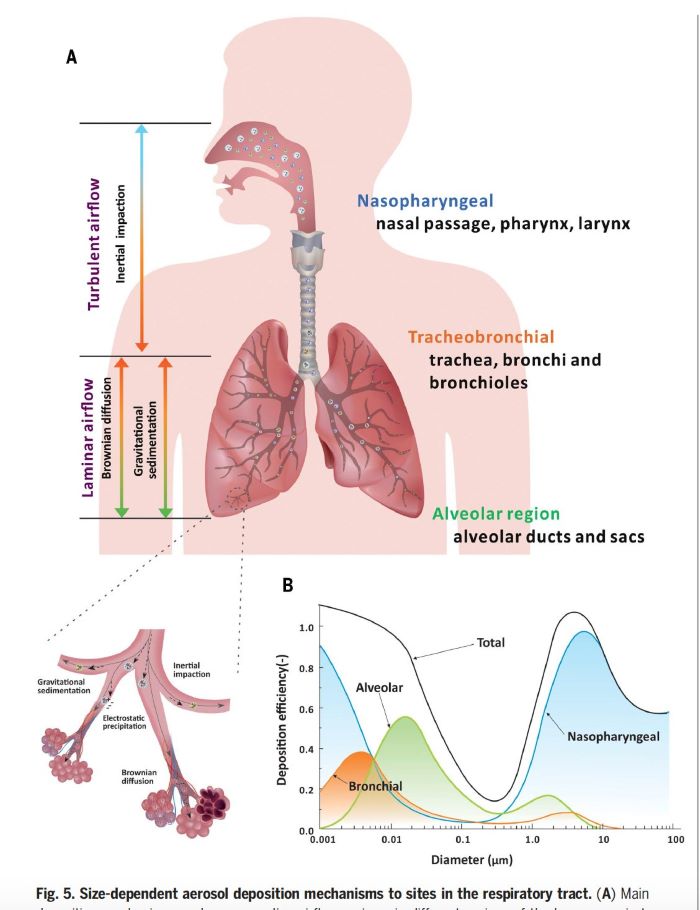
Some other interesting points are that children produce less aerosol particles because they have a smaller number of bronchi. I thought the bacteria were less likely to be aerosol transmitted than viruses, but they state that the R0 of tuberculosis can be as high as 4.3, vs. 7-8 for covid. The typical tuberculosis bacillus is relatively large, and yet is only 2 µm in length, well within the size of an aerosol particle.
–Dr. C
SCIENCE: CLEANING INDOOR AIR WILL IMPROVE HUMAN HEALTH AND COGNITION


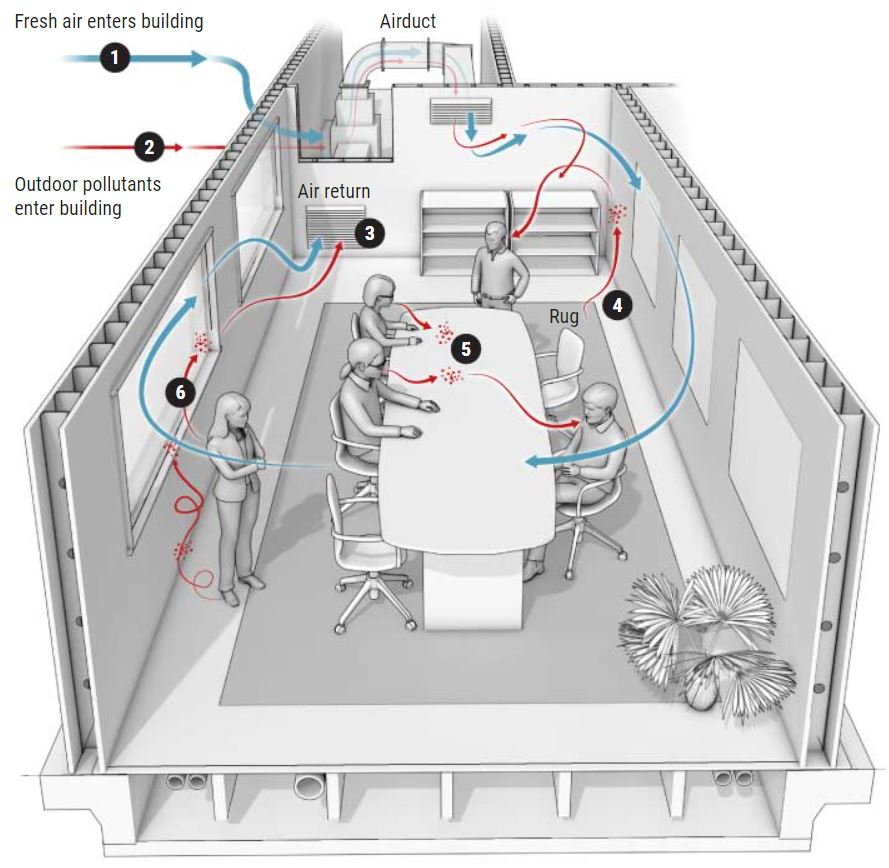
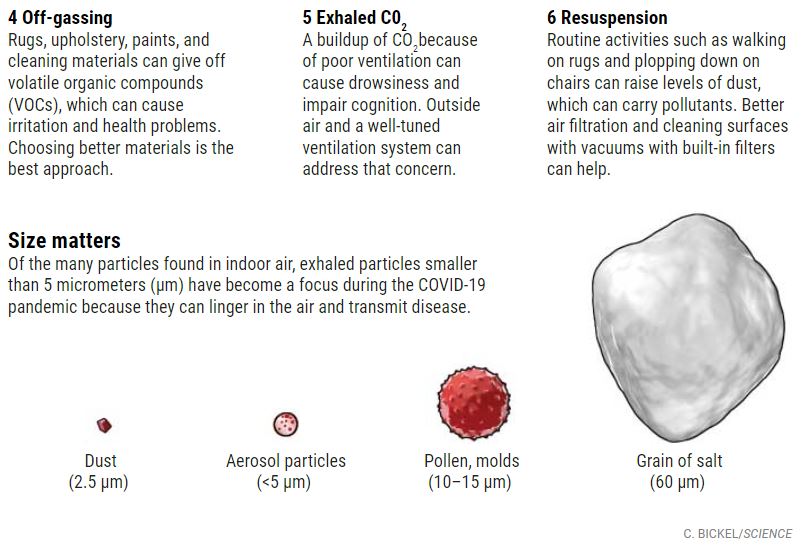

COMMENTARY:
Joseph Allen, the “air investigator”, was apparently on board early in the COVID-19 epidemic, stressing the importance of suspended air particulates, less than 2 microns in size, causing transmission of the disease.
His article in Science: “clean indoor air will improve human health and cognition” is well worth reading, or at least inspecting the info graphic. As a practicing allergist, I was aware that inside dust mite particles and mold spores made allergies worse. We had a service where we would go into homes and sample the air. An excess of certain Indoor mold spores, compared with those outside, would indicate a “problem home”. We would then try to find the water leakage source that produced the molds.
I also had a patient who could not tolerate a new house, with its carpets and other artificial materials. The only place where she felt better was in an old seaside house 100 miles south of San Francisco. I thought there were some psychological factors, but who knows? Volatile organic compounds, VOCs, probably affect some people more severely.
Beginning shortly after the energy crisis in the 80s, the “sick building syndrome”, characterized by headache and fatigue in certain buildings, was on the news. The eventual solution was to create better ventilation, with a reduction of CO2 and VOCs in those buildings. In addition, federal agencies began banning certain artificial fabrics that out-gassed VOCs.
There was eventually less talk about sick building syndrome, except for the occasional air system which was contaminated with Legionella bacteria.
The present article stresses accumulation of CO2 and VOCs In the stale air in the individual home or office as a cause of diminished attention and productivity.
CO2 monitors still cost about $200, and so I think I am going to just try to increase the ventilation in my office, where I get sleepy in the afternoon, by opening the windows and sliding doors. I wonder about the indoor CO2 in Scandinavian winters, where depression is increased.
—Dr. C.
MEDICINE: UNDERSTANDING ‘LONG COVID’ SYNDROME
The risk of COVID-19 has been largely communicated only in terms of deaths and hospital capacity, with recovery and survival conflated with each other. Around one in three people with symptomatic COVID-19 still experience symptoms 12 weeks after onset (1). Long Covid can be experienced by all age groups and not only those with acute severe disease. The debilitating symptoms are wide-ranging, multisystemic, and predominantly fluctuating or relapsing. There is still much to understand about Long Covid, but what is not well understood should not be ignored.
Long Covid is likely the first illness in history that has been defined by patients through social media platforms such as Twitter and Facebook. People with Long Covid formed a movement that demanded recognition of what was happening to them. During the first wave of the pandemic in 2020, online testimonials of prolonged symptoms following severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) infection were the only source of reassurance to others with a similar experience, including this author (2). In the absence of any guidance or recognition about the possibility of a persistent illness, peer support is all that people with Long Covid had. Many previously healthy and active people described persistent symptoms of the acute illness that fluctuated, with new symptoms appearing weeks later. In many countries, most nonhospitalized people did not have lab confirmation of SARS-CoV-2 infection owing to lack of access to community testing, so their symptoms remained without a diagnosis.
By summer 2020, thousands were joining social media support groups. A common theme started to emerge: lack of recognition by the medical profession. Patients, including doctors, with Long Covid were consulting their health care providers, and their symptoms were commonly minimized, dismissed, or labeled as anxiety (3). A narrative emerged of people struggling to make sense of their symptoms and forming their own groups to understand and research what was happening to them in an international citizen science movement (4). The testimonials of people living with Long Covid demonstrated themes of stigma and discrimination.
COVID-19: INSIDE MEDICINE’S LONGEST YEAR (2020 – 2021)
PROTEIN VACCINE: NOVAVAX PRIMES IMMUNE SYSTEM TO MAKE ANTIBODIES (VIDEO)
PODCAST: FEAR OF VACCINES, CONFUSION OVER ORIGINS OF CORONAVIRUS (sCIENCE)

Science Editor-in-Chief Holden Thorp joins host Sarah Crespi to discuss his editorial on preventing vaccine hesitancy during the coronavirus pandemic. Even before the current crisis, fear of vaccines had become a global problem, with the World Health Organization naming it as one of the top 10 worldwide health threats in 2019. Now, it seems increasingly possible that many people will refuse to get vaccinated. What can public health officials and researchers do to get ahead of this issue?
Also this week, Sarah talks with Science Senior Correspondent Jon Cohen about his story on Chinese scientist Shi Zhengli, the bat researcher at the center of the COVID-19 origins controversy—and why she thinks President Donald Trump owes her an apology.
Finally, Geert Van der Snickt, a professor in the conservation-restoration department at the University of Antwerp, talks with Sarah about his Science Advances paper on a new process for peering into the past of paintings. His team used a combination of techniques to look beneath an overpainting on the Ghent Altarpiece by Hubert and Jan Van Eyck—a pivotal piece that showed the potential of oil paints and even included an early example of painting from an aerial view.