Dr. Sachin Nagrani, Medical Director at HEAL, talks about the benefits and growth in Telemedicine appointments.
Tag Archives: Virtual
TELEHEALTH IN AUSTRALIA: “RPA VIRTUAL HOSPITAL” IS A 24/7 PATIENT CARE SYSTEM
From The Guardian (May 12, 2020):
“Now, everybody is on board,” says Dr Teresa Anderson, chief executive of the Sydney Local Health District. “There is not one clinical department across the district that is not providing care virtually.”

What a difference a pandemic makes. Although RPA Virtual Hospital was well into development when news broke from Wuhan in January, pandemic preparations meant it was scaled up far quicker than had been envisaged.
Anderson says RPA Virtual Hospital opened on 3 February with just six nurses. It now has more than 30 nurses, as well as medical and allied health teams, and 600 registered patients. Operating out of Royal Prince Alfred Hospital campus, it functions in many ways like a regular hospital, with a clinical handover, ward rounds, multidisciplinary team meetings and its own governance structures.
The virtual hospital is part of a wider suite of innovations developed at breakneck speed during the pandemic response, which include providing care in rented hotel and apartment accommodation to Covid-19 patients and others in quarantine, thus freeing up hospital beds.
COMMENTARY
The Covid epidemic spurred development of an addition to an already good medical care system.
A group of chronically ill patients were invited into the virtual care system. Nurses are used on initial encounter. They direct the enhanced home care, referrals or hospital care as needed. Electronic devices record the care given.
Hotels are used to quarantine suspected Covid patients, with telemonitoring.
As in America, the Covid epidemic has exposed the excesses of unneeded “elective” surgery, most notoriously surgery for back pain.
We can learn a lot by studying the health care of other countries.
—Dr. C.
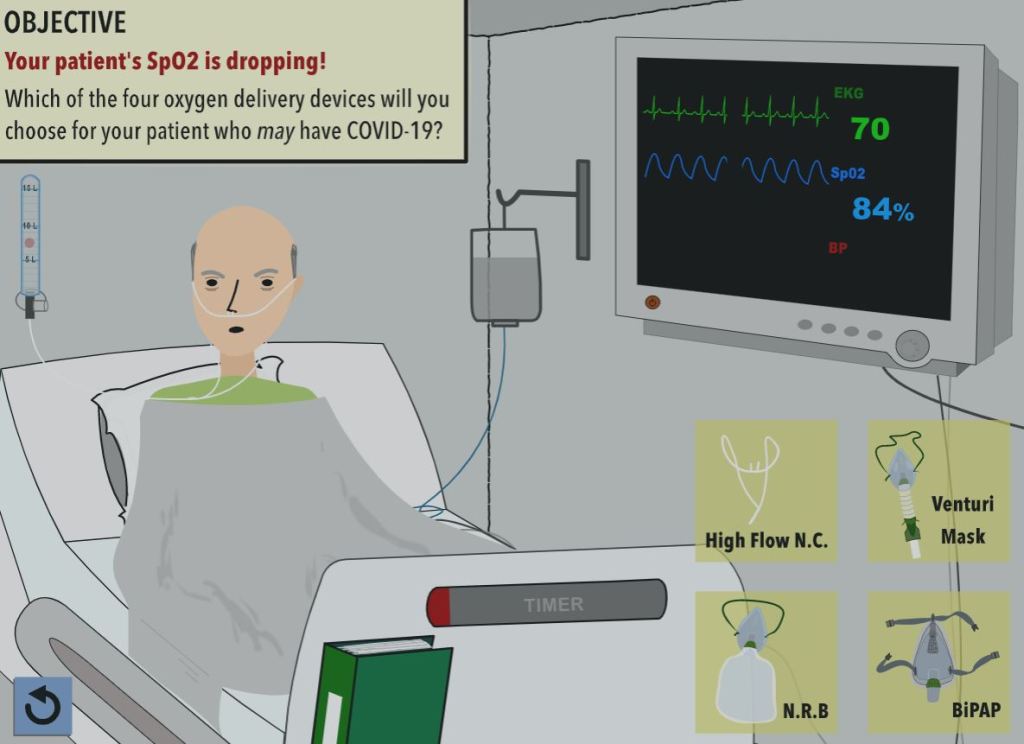
PHYSICIAN’S CORNER: NEJM “COVID-19 PRIMER – VIRTUAL PATIENT SIMULATION” (2020)

CLICK ON PATIENT BELOW TO LAUNCH “VIRTUAL PATIENT SIMULATION”

COMMENTARY
This interactive simulated case of Covid 19 (SARS CoV-2) is remarkable: a unique opportunity to stand in the shoes of a ER Doctor without any risk, except to our egos.
This is meant for doctors, but the intellectually curious Guests of this site might enjoy the experience, especially Doctor Lisa Sanders fans.
The vocabulary is full Medical, and will give a foretaste of the words I will slowly be exploring. I believe that patients should not be intimidated by their lab reports.
I’ll start the vocabulary journey with FERRITIN which is a marker for IRON STORES in the body. You can have too much iron, which is dangerous (iron overload), in which case the ferritin is high.
There was a time when I had too little iron ( was anemic, with a hemoglobin of 8.6, and felt terrible) and my ferritin was low. I now check my ferritin every 6 months to make sure I am taking enough iron to offset my blood loss, which is another story I will tell when I start go through my medicine cabinet and discuss the Meds one at a time.
The reason for testing ferritin in our interactive Covid 19 case was because ferritin is markedly elevated in cases of inflammation/ infection. It is an “acute phase reactant”, and may reflect the “cytokines storm” that may be a contributor to the lethality of Covid 19.
There is another way to benefit from this simulation: the train-wreck of a patient serves as a cautionary tale of what you wish NOT to become. Our present medical profession is so DISEASE oriented. How much better if our society and our medical profession were HEALTH oriented instead.
—Dr. C.
HHS Website: “Telehealth – Health Care From The Safety Of Our Homes”

For patients
Wondering how to get started with telehealth? Check out the information below to better understand your options.

If screening tools and self-checkers do not lead you to the care or information you are seeking, you can reach out directly to your doctor or health insurance company for options that can help connect you to a provider online. Understanding telehealth
Find out what it is, what to expect during a visit, and what kinds of care may be available. Telehealth during the COVID-19 emergency
Whether you’re looking for health care related to COVID-19 or something else, find out more about how to prepare for the visit. Preparing for a video visit
TELEMEDICINE: TRANSITION TO WIDESPREAD ADOPTION

Until recently, there were several barriers preventing widespread adoption of telemedicine. The two broad themes were:
- Providers, health systems, and payers were slow to embrace change
- A failure to appreciate that telemedicine is not a new type of medicine, but rather simply a care delivery mechanism that can be utilized with some patients, some of the time, to provide high-quality care

Addressing the Telemedicine Myths
Myth 1: Telemedicine is “too hard.”
This was not true before Covid-19 and we have further demonstrated that it is not true now. Almost every provider and the great majority of patients in the U.S. already possess the technology needed to conduct a telemedicine visit — a smartphone, tablet, or computer.
It turns out that when fear of catching a potentially fatal disease strikes, telemedicine is no longer too hard.
Myth 2: Patients prioritize existing relationships with their provider over transactional episodic care.
Data argues otherwise: The majority of times, patients just want care. Falling primary care visits rates, coupled with growing emergency department and urgent care visit rates, suggests convenience as more important than an established relationship.
Myth 3. You cannot do a physical examination.
It turns out you can. A new 21st-century physical exam utilizing telemedicine emphasizes the importance of general appearance (sick or not sick, weight, distress), respiratory effort, and environmental factors including a visual assessment of the home that is not something that can be accomplished at an office visit.
The majority of times, patients just want care.
Myth 4: Virtual visits are less effective than in-person visits.
Focusing on the comparison in diagnostic accuracy between virtual and in-person visits sets up a false dichotomy. Focusing on actionable information is more important than diagnostic accuracy.2 Actionable information recognizes providers might not always make a diagnosis within a single visit, whether in-person or telemedicine.
Like every other new challenge, you have to try telemedicine to get comfortable with it.
Myth 5. There is not a payment model supporting telemedicine.
While it is true that the Centers for Medicare & Medicaid Services (pre-Covid-19) had limited reimbursement based upon site of service and geography, since the Covid-19 outbreak, to the credit of the federal government and commercial payers, telemedicine is now covered.