Two years into the COVID pandemic, U.S. physicians have a growing arsenal of therapies to keep mild disease from worsening. Here is a rundown of what is on hand for hospitalized patients, as well as for people who are primarily recovering at home. https://t.co/4BV53Etz8s
— Scientific American (@sciam) January 21, 2022
Tag Archives: Drugs
Medicine: Is Metformin A Wonder Drug? (Harvard)
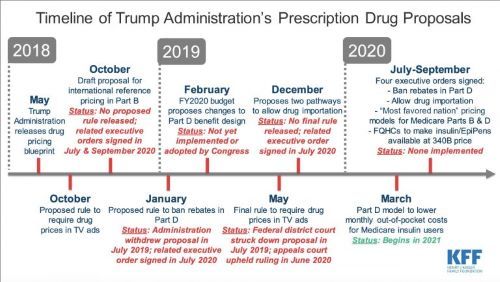
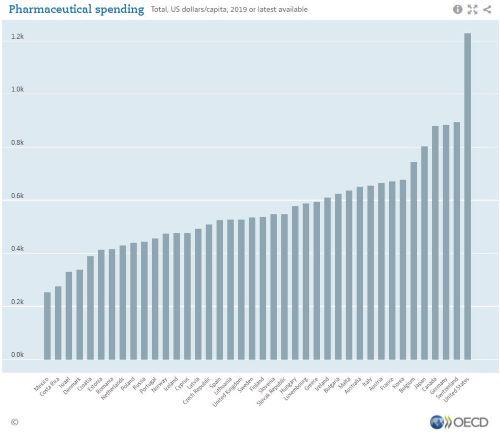
PRESCRIPTION DRUGS: ‘WHY THEY REMAIN HIGH-PRICED’
There may be few issues that unite Americans ahead of the 2020 election as do their concerns about the cost of prescription drugs.

A clear majority — 75% — of respondents to a July survey said the cost of prescription medicines would be among the factors likely to influence their votes this year, according to a report from Gallup and the nonprofit West Health. Gallup reported on results from 1,007 interviews conducted with adults between July 1 and July 24.
1. What are the 2020 presidential candidates saying they will do to lower drug prices?
Both President Donald Trump, a Republican, and former Vice President Joe Biden, a Democrat, have highlighted insulin costs in their discussions of the need to lower drug prices.
In a January interview with the New York Times editorial board, Biden noted the widespread discontent among Americans about sticker shock often experienced at pharmacies. He spoke of a need for the federal government to act to make medicines more affordable.
“This is a place where I find, whether you’re Republican or Democrat, you think you’re getting screwed on drug prices. And you are, in terms of everything from insulin to inhalers and a whole range of other things,” Biden said. “So, again, can I guarantee that it gets done? No, but I can tell you what, if anybody can get it done, I can, and I think there’s a consensus for it.”
2. Why doesn’t Medicare, the biggest U.S. purchaser of drugs, directly negotiate on drug prices?
Congress has taken different approaches in designing the terms under which the two largest federal health programs, Medicaid and Medicare, buy drugs.
Medicaid is a program run by states with federal contributions and oversight. It covers people with low incomes and disabilities. Almost 67 million people were enrolled in Medicaid as of May 2020, including about 29 million children. In 1990 Congress decided that drugmakers who want to have their products covered by Medicaid must give rebates to the government. The initial rebate is equal to 23.1% of the average manufacturer price (AMP) for most drugs, or the AMP minus the best price provided to most other private-sector payers, whichever is greater. An additional rebate kicks in when prices rise faster than general inflation.
3. What’s the deal with rebates and discounts?
There’s widespread frustration among lawmakers and policy analysts about the lack of clarity about the role of middlemen in the supply chain for medicines. Known as pharmacy benefit managers (PBMs), these businesses describe the aim of their business as making drugs more affordable for consumers. Insurers like Cigna and UnitedHealth operate some of the nation’s largest PBMs, as does pharmacy giant CVS Health, which also owns insurer Aetna.
“They will tell you their mission is to lower drug costs,” said Rep. Earl L. “Buddy” Carter, a Georgia Republican, a pharmacist and a critic of PBMs, in a speech on the House floor last year. “My question to you would be: How is that working out?”
4. What is the “distinctly American” phenomenon of specialty drugs?
Kesselheim also has written on what he terms “Specialty Drugs — A Distinctly American Phenomenon.” That’s the title of a 2020 paper in the New England Journal of Medicine Kesselheim authored with Huseyin Naci, an associate professor of health policy at the London School of Economics.
In this Perspective article, Kesselheim and Naci look at how the “specialty” designation morphed from its origin in the 1970s. It then referred to a need for extra steps for preparation and delivery of new injectable and infusion products.
5. How much does it cost to bring a new drug to market anyway?
The median cost for a medicine developed in recent years was $985 million, according to a study published in JAMA in March 2020, “Estimated Research and Development Investment Needed to Bring a New Medicine to Market, 2009-2018.”
“Rising drug prices have attracted public debate in the United States and abroad on fairness of drug pricing and revenues,” write the study’s authors: Olivier J. Wouters of the London School of Economics; Martin McKee of the London School of Hygiene and Tropical Medicine; and Jeroen Luyten of Leuven Institute for Healthcare Policy, KU Leuven, Belgium. “Central to this debate is the scale of research and development investment by companies that is required to bring new medicines to market.”
INFOGRAPHIC: “MEDICAID PHARMACY BENEFITS IN U.S.”

PRESCRIPTION DRUGS: “ON MEDICATIONS IN GENERAL”
Several ideas apply to ALL MEDICINES. Terminology should be clarified. Medicine, Pharmaceutical, and Drug, in my mind are equivalent.

The term “drug” is pejorative, and I try to use it so. The term “Pharmaceutical” is too long, leaving me with “medication”.
There are some Practical points. You should look at your prescription when you first get it, to make sure it is the right one. Yes, pharmacists rarely make some mistakes. They are human.
You should ask the Pharmacist if she knows WHERE the drug was manufactured. Foreign countries, especially China and India, are less reliable, and the USA is safer. The original Brand Name drugs are more often domestically produced, but even these are being “offshored”.
Next, check the prescription date and expiration date.You should get a ” SHELF LIFE” (the difference between the two) of about 2 years, otherwise, you might ask the pharmacist the next time to give you the “best dating” in his stock.
Store your medications in a cool, dark, dry place in order to prolong their life. Light, heat and moisture degrade most compounds. Remember the O.J. Simpson case? Part of the reason he was acquitted is that a critical DNA sample was stored in a plastic bag, which retained moisture, rather than a paper bag, which is recommended because paper is porous, and allows moisture to escape.
You should follow the suggested TIME to take the medication, because there is almost always an optimal time to take a given medication.

CHRONOPHARMACOLOGY is an emerging field, which is finding that more than 50% of medications are TIME SENSITIVE in their effect in the body. This is an unimportant, academic consideration for most Patients, given the high THERAPEUTIC WINDOW (dosage latitude) of most medications, the mild illness of most patients, and the disinclination of most Doctors to add one more detail onto their already heavy load.
In discussing the medicines in my cabinet and a few other important ones, I will be addressing TIMING.
What about OUTDATED MEDICATIONS? As discussed by the following article from Harvard, the dating is not critical except for liquids, and a few others, like Tetracycline.
This is fortunate, given the expense of medications today. What if I drop a pill on the floor, at home. I usually pick it up and take it. if i just dropped it, unless it is very inexpensive.
What if a pill sticks in your throat, like happens to me a lot? I drink water first, to moisten my throat to make it slipperier.
Next, I take a good sip of water, try to swish it back and go back with my head to accelerate the pill backward, and think confidence. Certain sizes of pills are my nemesis and i have to break them in two.
Please follow Dr. Cs Medicine Cabinet in future postings of DWWR.
–Dr.C.
CORONAVIRUS: CONFUSING HYDROXYCHLOROQUINE STUDIES (NATURE PODCAST)
President Trump’s preferred coronavirus treatment is the focus of a new study suggesting it could cause more harm than good, but not everybody agrees. We discuss the fallout as trials around the world are paused and countries diverge over policy advice.

12:12 Are we rushing science?
Coronavirus papers are being published extremely quickly, while normally healthy scientific debate is being blown up in the world’s press. Is there a balancing act between timely research and accurate messaging?
18:49 One good thing
Our hosts pick out things that have made them smile in the last week, including hedgerow brews and a trip into the past using AI.
Recipe: Elderflower ‘Champagne’
Video: Denis Shiryaev restores historic footage with AI
22:30 The latest coronavirus research papers
Noah Baker takes a look through some of the key coronavirus papers of the last few weeks.
News: Coronavirus research updates
medRxiv: Full genome viral sequences inform patterns of SARS-CoV-2 spread into and within Israel
Harvard Library: Reductions in commuting mobility predict geographic differences in SARS-CoV-2 prevalence in New York City
Science: DNA vaccine protection against SARS-CoV-2 in rhesus macaques