Continuing the AMA’s “Look Forward/Look Back” series, AMA CXO Todd Unger talks with Meg Barron, the AMA’s vice president of digital health strategy, about the role of telehealth post-pandemic and a new program that can help practices optimize and expand their telehealth efforts.
Tag Archives: Digital Health
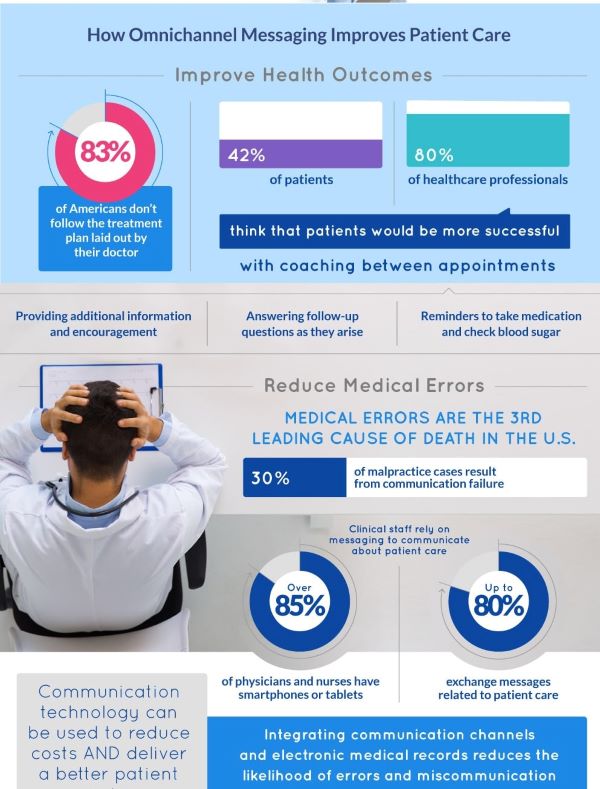
INFOGRAPHIC: FUTURE OF HEALTHCARE IS DIGITAL
DIGITAL HEALTH: THE FUTURE OF WEARABLE DEVICES
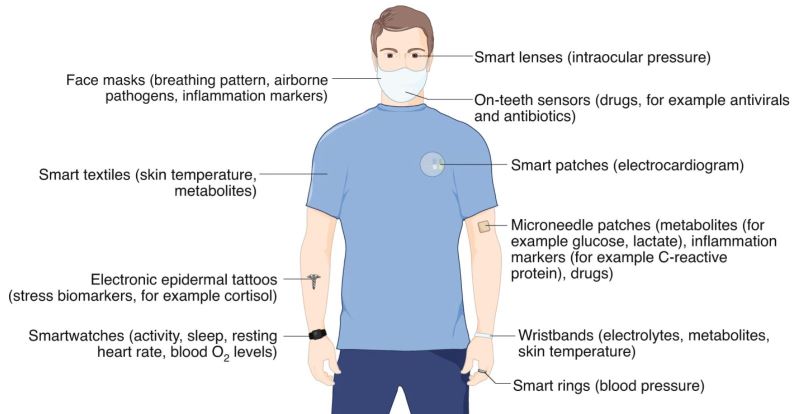

Currently, smartwatches provide information such as heart rate, sleep time and activity patterns. In the future, this could be augmented with new classes of wearable devices that monitor, for example, concentrations of cortisol for tracking stress (using electronic epidermal tattoos), biomarkers of inflammation and levels of blood O2 (microneedle patches), skin temperature (electronic textiles), blood pressure (smart rings), concentration of ions (wristbands), intraocular pressure (smart contact lenses), the presence of airborne pathogens and breathing anomalies (face masks), and the concentration of therapeutic drugs (on-teeth sensors)2,10,12,13,14,15,16. Such emerging low-cost wearable sensing technologies, monitoring both physical parameters and biochemical markers, could be used to identify symptomatic and pre-symptomatic cases in future pandemics. The devices could also be used to remotely monitor the recovery of individuals undergoing treatment or self-isolating at home.
HEALTHCARE: TOP DIGITAL TECHNOLOGY TRENDS (2020)
From MD+DI (June 17, 2020):

Remote-care solutions like telehealth and wearable devices are included in the new approach that healthcare professionals will be embracing as they position their businesses to best serve patients in a COVID-19 world. Digital healthcare product solutions address critical issues for the remote delivery of care or the “hospital at home” that have been resonating long before we began looking at all our interactions through a social-distancing lens.
Wearables and On-Body Devices – Real-time data collection and communication are critical to digital health initiatives. More than half of survey respondents—52%—said they are currently developing or planning to develop wearable or on-body devices as part of their strategy. Another 33% said the same for patient-monitoring solutions.

Miniaturization, flexible circuitry, and biometric capturing sensors are leading to exciting new devices that will help patients in recovery or with chronic issues. The data communicated from these solutions will equip healthcare providers and patients with the data that can transform healthcare.
Seamless technology integration – A range of emerging technologies, including artificial intelligence (AI), 5G, cloud-based applications, and a growing roster of IoMT devices.
More than nine in 10 healthcare solution providers agree that the collection and purposing of data should be standardized to enable interoperability between devices and within product platforms, according to the survey.
TELEHEALTH CARE: PATIENTS CAN EXPECT EXPANDED “CONTACTLESS EXPERIENCES”
From Healthcare IT News (June 12, 2020):
Technology-enabled workflows now enable patients to complete most of the registration formalities prior to the visit, be it a virtual consult or a clinic visit. Registration kiosks in hospital lobbies may soon be enabled with facial recognition software to eliminate the need for touching any surface.

Routine examinations are also going virtual, with many diagnostic procedures now possible through remotely controlled devices. Caregivers are beginning to do their patient rounds through virtual visits. This trend will only grow in the coming years.
A vast and growing array of automated communication tools allows caregivers to use rule-based messaging to push everything from health coaching, post-discharge care instructions, and appointment reminders through IVR, text, SMS, and mobile alerts.
PODCASTS: TELEMEDICINE TECHNOLOGY CAN LEAVE MANY PATIENTS BEHIND
Amid the Covid-19 pandemic, more doctors are turning to telemedicine. That’s a problem for tens of millions on the wrong side of the digital divide.
SPEAKING ON A landline, the patient complained of an itchy eye. On the call’s other end, physician Carla Harwell considered the possibilities, from seasonal allergies to vision-damaging herpes. Luckily, the elderly patient’s daughter was visiting during the phone consultation, so Harwell asked her to text a picture of her mom’s eye. The photo shocked Harwell. It was the worst case of bacterial conjunctivitis the doctor had ever seen.

Without the picture, Harwell would have told the octogenarian patient to call back in a few days or come to her office, risking an in-patient visit during the Covid-19 pandemic. She certainly wouldn’t have prescribed the antibacterial eye drops needed to treat the infection. “I probably would not have prescribed anything,” Harwell says. “That’s a scary thought.”
COMMENTARY
Telehealth is here, will remain after the pandemic, and is useful in many situations.
Being older, poorer, minority, Linguistically challenged, rural, less informed and less Tech-savvy reinforce each other in comprising Barriers to proper Medical care of ANY kind, especially Telemedicine. These handicaps will hopefully improve with time, and should be A societal priority.
Special internet-connected roving Aid-mobiles in afflicted areas is one feasible idea that would help. Responding to a lesser “911” number, the health-van could go to the calling persons location, help the person to the van, take pictures and other data for a Telehealth Doctor to evaluate, and facilitate treatment.
A neighborhood Telehealth site is also workable, and was a precondition to Rural Telehealth access, pre-pandemic.
If you are reading this message, congratulations! You are increasing your information, technical facility and your access to better Healthcare.
—Dr. C.
INFOGRAPHICS: “DIGITAL HEALTH TECHNOLOGIES IMPROVING PATIENT CARE”

COMMENTARY
The technology of telemedicine will predictably and steadily get better.
Medical assistants, mostly human at present, are commonplace, notably in specialty offices, and machines using improving voice-to-text transcription are getting better.
Wearable devices are proliferating and hopefully coming down in cost, and platform technology is improving though still glitchy.
Patients generally accept Telemedicine. They like the saving of travel time and infection exposure.
Doctors may drag their feet because the increased effort and legal exposure is not compensated by increase in payment. On the contrary, pre-Covid compensation was LESS for a televisit. Continuing Parity would help.
The politicians at the state level should eventually make licenses valid across state borders.
The big wild card is the Legal Profession. Unless they develop restraint( and litigious patients reform), there could be a feeding Frenzy, which would delay implementation of a very good idea.
Eventually telemedicine deserves to be 50% or more of medical practice.
—Dr. C.
Podcasts: “The Usefulness of Telehealth and Digital Health During COVID-19 “
In the current times that we live in health care professionals are looking for ways to provide safe, quality care from a distance. Telehealth and Digital health are proving to be the perfect tools during this COVID-19 pandemic.
PART I
In today’s episode Part I, we are joined with Dr. Amit Sachdev and Dr. Curtis Lowery. Dr. Sachdev is a physician most recently at the Brigham and Women’s Hospital, Harvard Medical School and he is currently working on the COVID response.

Dr. Curtis Lowery is the director of the UAMS Institute for Digital Health and Innovation. He also serves as a professor for the UAMS Department of Obstetrics and Gynecology. This episode is in two parts and it serves as an introduction to telehealth and digital health amidst the COVID-19 pandemic.
PART II
In part 2 of our conversation with Dr. Amit Sachdev and Dr. Curtis Lowery over the usefulness of telehealth and digital health during the COVID-19 pandemic. Dr. Sachdev is a physician most recently at the Brigham and Women’s Hospital, Harvard Medical School and he is currently working on the COVID response. Dr. Curtis Lowery is the director of the UAMS Institute for Digital Health and Innovation. He also serves as a professor for the UAMS Department of Obstetrics and Gynecology. Let’s continue the conversation.