Degenerative neurological diseases are particularly horrible. They affect the brain, the very essence of our humanity. Moreover, almost all of these conditions have no satisfactory treatment. Alzheimer’s, Parkinson’s, and Huntington’s disease come to mind.
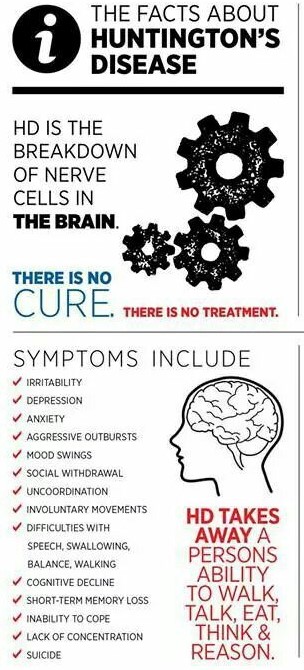
Much more is known about the genetics of Huntington’s than any other aspect of the disease. The problem is due to CAG repeats, which either crowd out or distort the function of the Htt protein.
If a child of a Huntington family anticipates having children, intervention to prevent transmission, such as artificial insemination and eliminating any zygotes containing the Huntington Gene will prevent the children from inheriting the disease.
Huntington’s is considered to be inherited by a somatic dominant Gene. This gene codes for a number of CAG repeats in excess of the normal number, less than 35. However the number of CAG repeats tends to increase with each generation, and it is possible for parents with somewhat less than 35 repeats eventually to produce the disease in their offspring.
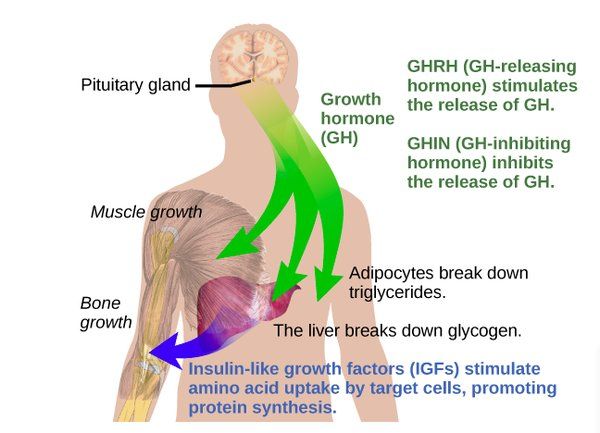
As in any degenerative brain disease, the focus of medical treatment is on neurotransmitters. This is because neurotransmitters can be studied and used as the basis of medical treatment that lessens the effects of the disease. In the case of Huntington’s, dopamine, glutamate and acetylcholine have all been implicated, although transmitter balance is probably more important, and changes with time.
Neural malfunction, however, is where the true pathology lies, and all neurons, especially those of the Corpus stratum and Cerebral Cortex contain Htt and are eventually involved, Leaving a shrunken brain that loses much of its substance and function.
The symptoms begin as a movement disorder, and initially was called Huntington Chorea, because of the abnormal “Dance-like” movements of affected individuals . Eventually, psychiatric, intellectual and other symptoms occur which span all areas of the brain.
Today, after swimming, I encountered a man whose brother has Huntington’s disease. So far he has been spared. He is part of a study of Huntington’s Disease Families. He denies knowing anything about his genetics, and indeed does not want to know, Nor would I in his situation, since nothing can be done to affect the basic progress of the disease.
Please refer to the accompanying meal clinic article for more information about Huntington‘s disease.