

Go to online ‘interactive’ puzzle
Solution to last week’s puzzle:
From tele-consults in the ED to on-site fundus imaging at Primary Care offices, New York Eye and Ear Infirmary of Mount Sinai (NYEE) is adapting to the rapidly changing healthcare environment with innovative new applications and technologies and making them a permanent part of our patient service. These approaches are not only valuable social distancing tools, to reduce coronavirus exposure of physicians, staff, and patients, but they also allow greater access to care and quicker and more effective triage of patients.
For more information about NYEE, visit www.nyee.edu
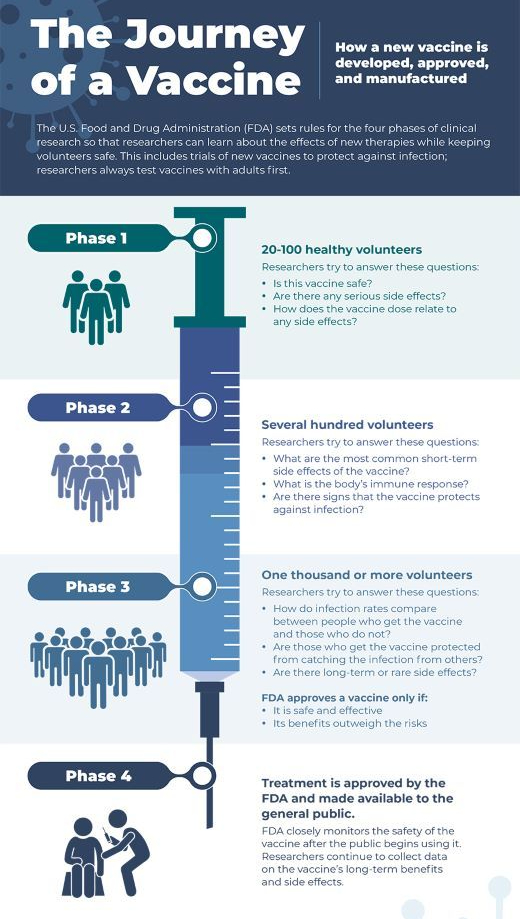
Anthony S. Fauci, MD returns to JAMA’s Q&A series to discuss the latest developments in the COVID-19 pandemic, including the continued importance of nonpharmaceutical interventions (masking, handwashing, physical distancing) for managing rising case numbers in the US and globally.
Recorded October 28, 2020.
Topics discussed in this interview: 0:00 Introduction 0:20 NAM Presidential Citation for Exemplary Leadership 1:19 COVID-19 numbers and excess deaths 4:05 National masking mandate 5:55 How to get people to accept masking 7:07 Herd Immunity and the Great Barrington Declaration 9:51 The holidays and airplane travel 13:44 Therapies update 17:54 Vaccines update 20:08 Vaccine distribution 22:00 Vaccine safety 24:42 How Australia has dealt with COVID-19 spikes 27:00 Acknowledgements and baseball
Peripheral Neuropathy is a common problem, and almost a quarter of the population will eventually suffer from it. It is very common in diabetes and metabolic syndrome, alcoholism, and in cancer therapy.
Even getting older is a risk; almost 10% of individuals 65 years old have some symptoms. There are more than 100 different types of peripheral neuropathy, and often it is just one feature of a primary illness.
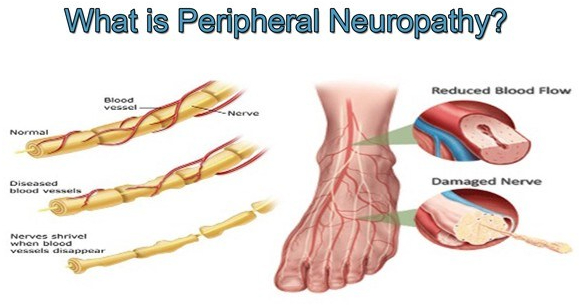
Sometimes there is no known cause, such as in 2 of my older friends. I have a diminished vibratory sense in my feet, which causes me no noticeable problem. The longer nerves are more likely to be involved, except for the rare sensory ganglionopathy which is symptomatic of some cancers ( a “paraneoplastic disorder”) , some infections and autoimmune diseases.
When the sensory ganglia are involved, the numbness, tingling or pain can be more central, such as in the face or upper arm. There are 3 types of nerves that can be involved in peripheral neuropathy; Sensory, Motor and autonomic.
The sensory nerves deal with sensations, such as hot, cold, touch, pain, tingling, and numbness. Motor nerve involvement results in weakness or paralysis of an arm, leg or other area under Voluntary control. The autonomic nervous system coordinates activities beyond voluntary control, such as sweating, salivation, food propulsion and heart rate, which can be activated or inhibited.
The symptoms of neuropathy depend upon the type of nerve involved. Balance is a complex ability that can be disturbed by a lack of proper sensory nerve function (Position sense or proprioception) motor weakness, vision or coordination which involve higher centers.
The medical evaluation of peripheral neuropathy begins with a family practitioner or internist who does a detailed history, asking about such things as diet, medications, alcohol consumption, and injuries. Vitamin intake is important, but can be overdone.
Peripheral nerve symptoms can actually be caused by excessive B6, pyridoxine. The upper limit is 100 Mg.. A physical exam checks for weakness, sensory problems, reflexes and balance. Blood tests may reveal diabetic, kidney, liver, thyroid or immune problems problems.
A major disorder associated with neuropathy may be revealed and pursued. If nothing turns up, and the neuropathy is significant, referral may be needed to a neurologist, or other appropriate specialist. Many specialized tests and treatments may be needed.
Even with the best of care, a specific “cure” may not be found. Peripheral neuropathy can often be avoided by a healthy lifestyle.
A new recipe for patterning cells on a surface holds promise for spinal cord injuries. Video by the Office of Communications
DR. C REVIEWS MAJOR HEALTH AND TELEMEDICAL NEWS FOR THE WEEK ENDING OCTOBER 25, 2020.



There are over 35,000,000 reported cases of COVID-19 disease and 1 000 000 deaths across more than 200 countries worldwide.1 With cases continuing to rise and a robust vaccine not yet available for safe and widespread delivery, lifestyle adaptations will be needed for the foreseeable future. As we try to contain the spread of the virus, adults are spending more time at home. Recent evidence2 suggests that physical activity levels have decreased by ~30% and sitting time has increased by ~30%. This is a major concern as physical inactivity and sedentary behaviour are risk factors3 for cardiovascular disease, obesity, cancer, diabetes, hypertension, bone and joint disease, depression and premature death.
To date, more than 130 authors from across the world have provided COVID-19-related commentary on these concerns. Many experts4 have emphasised the importance of increasing healthy living behaviours and others5 have indicated that we are now simultaneously fighting not one but two pandemics (ie, COVID-19, physical inactivity). Physical inactivity alone results in over 3 million deaths per year5 and a global burden of US$50 billion.6 Immediate action is required to facilitate physical activity during the COVID-19 pandemic because it is an effective form of medicine3 to promote good health, prevent disease and bolster immune function. Accordingly, widespread messaging to keep adults physically active is of paramount importance.
Several organisations including the WHO, American Heart Association and American College of Sports Medicine have offered initial suggestions and resources for engaging in physical activity during the COVID-19 pandemic. Expanding on these resources, our infographic aims to present a comprehensive illustration for promoting daily physical activity to the lay audience during the COVID-19 pandemic (figure 1). As illustrated, adults are spending more time at home, moving less and sitting more. Physical activity provides numerous health benefits, some of which may even help directly combat the effects of COVID-19. For substantial health benefits, adults should engage in 150–300 min of moderate-to-vigorous intensity physical activity each week and limit the time spent sitting. The recommended levels of physical activity are safely attainable even at home. Using a combination of both formal and informal activities, 150 min can be reached during the week with frequent sessions of physical activity spread throughout the day. Sedentary behaviour can be further reduced by breaking up prolonged sitting with short active breaks. In summary, this infographic offers as an evidence-based tool for public health officials, clinicians, educators and policymakers to communicate the importance of engaging in physical activity during the COVID-19 pandemic.
Learn more about the Yale School of Medicine and #YaleMedicine‘s response to COVID-19, visit: https://covid.yale.edu.