Bad breath is a big social deal, and is unpleasant to be around. You are always conflicted when near a person with Halitosis; you are tempted to tell him for his own good, but are embarrassed to do so.
“Mask Breath” is the most recent reincarnation of bad breath. Supposedly the mask itself does not have an odor, but merely makes the person aware of the bad breath he has had all along. Bad breath is not only a direct problem for the person who has it, but often betrays important medical conditions which need attention.
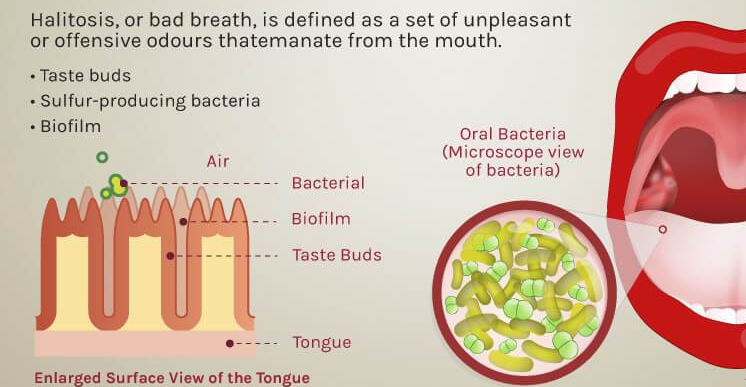
Several oral conditions can cause halitosis. The most common is poor oral hygiene. Lack of regular brushing and flossing leads to accumulation of food particles between the teeth, in the gum lines, and even under crowns. This food provides lunch for the oral bacteria, releasing malodorous compounds. This can be expensive. Have you priced restorations and implants recently?
The sneakier result of poor oral hygiene is gingivitis, or gum disease. This leads to inflammation, and is a major contributor to the inflammatory load resulting in Metabolic syndrome with its widespread effects on the brain, kidneys, and heart. And in addition, you may eventually lose your teeth. Tonsils can become inflamed and malodorous, and the associated adenoids may enlarge, leading to mouth breathing, dry mouth, and you guessed it, Bad Breath.
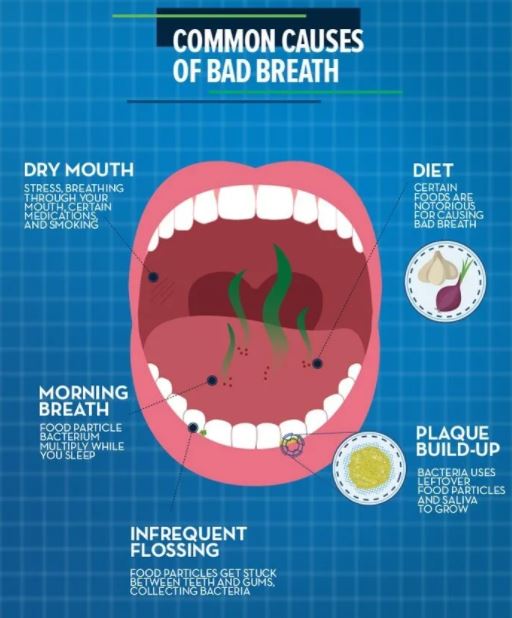
GERD is often associated with Bad Breath. The reflux of stomach contents will often leave behind a bad taste as well as bad breath. Certain metabolic conditions can give bad breath. Ketosis from diabetes, mousy breath from liver failure, and the “Fish odor syndrome”, Trimethylaminuria, can be causes.
So drink lots of water, and don’t forget to brush your teeth and floss regularly. You might benefit from a medical or dental evaluation if your bad breath doesn’t go away.