Gastroesophageal reflux disease (GERD) is one of the most common digestive disorders in the world. It happens when acid comes up from the stomach, which is acid-resistant, into the esophagus, which is less acid-resistant. Dr. James East, a gastroenterologist at Mayo Clinic Healthcare in London, says GERD may be common, but there can be potentially severe complications if it’s ongoing and left untreated.
Tag Archives: GERD
THE DOCTORS 101 CHRONIC SYMPTOMS & CONDITIONS #17: BAD BREATH (HALITOSIS)
Bad breath is a big social deal, and is unpleasant to be around. You are always conflicted when near a person with Halitosis; you are tempted to tell him for his own good, but are embarrassed to do so.
“Mask Breath” is the most recent reincarnation of bad breath. Supposedly the mask itself does not have an odor, but merely makes the person aware of the bad breath he has had all along. Bad breath is not only a direct problem for the person who has it, but often betrays important medical conditions which need attention.
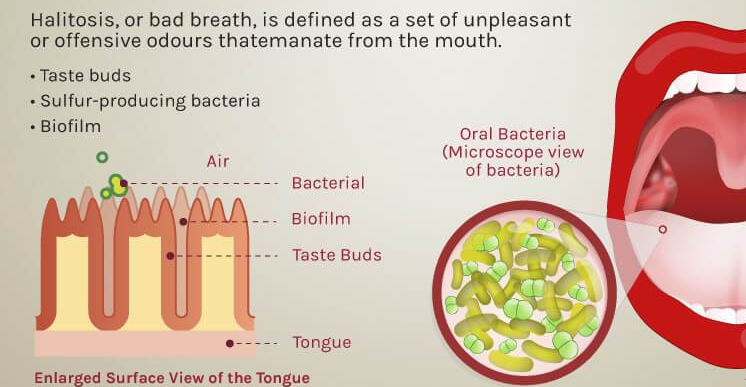
Several oral conditions can cause halitosis. The most common is poor oral hygiene. Lack of regular brushing and flossing leads to accumulation of food particles between the teeth, in the gum lines, and even under crowns. This food provides lunch for the oral bacteria, releasing malodorous compounds. This can be expensive. Have you priced restorations and implants recently?
The sneakier result of poor oral hygiene is gingivitis, or gum disease. This leads to inflammation, and is a major contributor to the inflammatory load resulting in Metabolic syndrome with its widespread effects on the brain, kidneys, and heart. And in addition, you may eventually lose your teeth. Tonsils can become inflamed and malodorous, and the associated adenoids may enlarge, leading to mouth breathing, dry mouth, and you guessed it, Bad Breath.
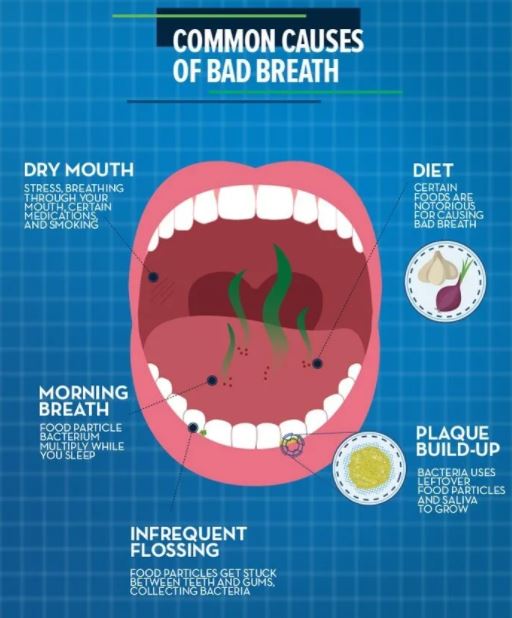
GERD is often associated with Bad Breath. The reflux of stomach contents will often leave behind a bad taste as well as bad breath. Certain metabolic conditions can give bad breath. Ketosis from diabetes, mousy breath from liver failure, and the “Fish odor syndrome”, Trimethylaminuria, can be causes.
So drink lots of water, and don’t forget to brush your teeth and floss regularly. You might benefit from a medical or dental evaluation if your bad breath doesn’t go away.
–Dr. C.
THE DOCTORS 101 CHRONIC SYMPTOMS & CONDITIONS #11: “SWALLOWING TROUBLE”
I am defining SWALLOWING TROUBLE as the difficulty in transport of food to the stomach, once clear of the throat. Problems with the initiation of the swallowing process are discussed separately.

PAIN in the mid-chest ON SWALLOWING is a worrisome symptom which can be due to inflammation of the lining of the esophagus from a variety of causes. An esophageal yeast infection, which can also involve the throat (called ‘“thrush”), often warns of immune deficiency and can be a sign of AIDS, or be caused by immune suppressing medication. If persistent, pain on swallowing can be a warning sign of CANCER.
If in the presence of GERD, it can be a sign of chronic inflammation or ulceration. In-coordination of the normally smooth muscular propulsive wave can cause a cramping, muscular pain.
Normal “peristalsis” is so efficient, that food can be swallowed without the help of gravity, when UPSIDE DOWN. I wouldn’t recommend trying this, even to cure hiccoughs. There is a muscular “gate” at the bottom of the esophagus, just as it enters the stomach. This gate is often too relaxed, and allows for the reflux of acid and food from the stomach, or GERD. It can also Fail to open, called achalasia, and hold up the food in its journey to the stomach.
The area can be scarred by repeated acid reflux, and become NARROWED; this is called a STRICTURE, and can cause a blockage in swallowing. One of my Doctor friends had to go to the Emergency room when some Steak got stuck in the esophagus.
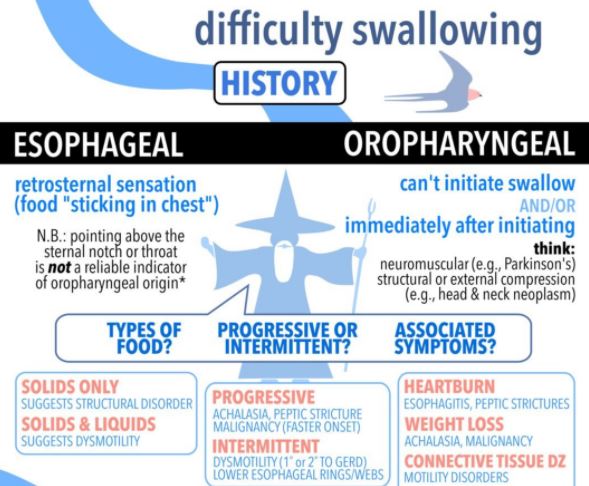
The ER Doctor removed the steak with a fiberoptic Scope, and then proceeded to DILATE the stricture with a “bougie”, an instrument of a precisely calibrated size designed to STRETCH the constricted area. This uncomfortable procedure had to be done repeatedly, a caution to those who would wait too long before getting such a problem evaluated and corrected.
EOSINOPHILIC ESOPHAGITIS has been diagnosed with increasing frequency, and can cause Pain in the middle of the chest, trouble swallowing, and even regurgitation of food. This special type of inflammation is more common in allergic patients, and can be caused by certain foods.
So as you can see, swallowing trouble, if persistent, is nothing to fool around with, and should be checked out by a competent doctor. Don’t wait too long.
–Dr. C..
Dr. C’s Journal: A Little Bit About “Energy & Fatigue”
Sometimes I wake up in the morning with a feeling of RELAXED ENERGY. My mind is clear, I have no fatigue, and believe once more that the world is wonderful, and it’s great to be alive.
I St-re-tch, exercise my hands (I have Osteoarthritis, and they are stiff), take out my Nite guard ( I grind my teeth at night and would otherwise wear them away), take my beta blocker eye drops ( to lower my intraocular pressure) and wash down my Eliquis ( an anticoagulant to prevent stroke from my Atrial Fibrillation) with 16 oz. of water, while thinking about all of the delights awaiting me.
Yes, my body was in better shape 60 years ago; but I had much more responsibility then, and much less discretionary time. All things considered, I like to believe that I am happier now.

The KEY is to stay in GOOD HEALTH. GOOD SLEEP is critical, but it cannot be had by willpower alone. As I have discussed previously, you need a bedtime routine, good SLEEP HYGIENE.
You also need a…….. GOOD DIET. with lots of fruits, vegetables and whole grains. Fatty, spicy foods will stay in your stomach and bother you at night, particularly if you eat Late. I like to finish eating by 5 PM. Late dinner is also likely to produce GERD, and maybe Sleep Apnea.
GOOD EXERCISE is also critical. If you are not tired at the end of the day, it is hard to get good sleep. I always seem to sleep better on the day when I walk the hills for an hour, which is 3 days a week. Try not to exercise within 2 hours of bedtime. Assuming that you have a good base of SLEEP, DIET and EXERCISE, there are other mechanisms that can foul things up. INFLAMMATORY conditions often cause fatigue.
The most common inflammatory diseases are OBESITY, METABOLIC SYNDROME and DIABETES. OBESITY is the defining disease of our EXCESSIVE SOCIETY, where there is too much of everything, and excessive consumption is relentlessly advertised everywhere.
External correction is probably a pipe dream, since there is no will even to Tax Sugar-containing Beverages, the “low hanging fruit” of dietary excess. Internal correction is all that is left, and that takes WILL POWER, also in short supply.
INFECTIOUS DISEASES are a subset of inflammatory conditions. COVID 19 is the poster child of infection, and FATIGUE is one of the hallmarks of the disease. Interleukins, like TNF-alpha, IL-1, andIL-6 are some of the defense factors which cause the fatigue. AUTOIMMUNE Diseases like Rheumatoid Arthritis and Lupus are also associated with fatigue-producing interleukins.

Fatigue even has its own flagship disease, CHRONIC FATIGUE SYNDROME. Chronic viral disease has been suspected as the cause of this condition, and inflammatory cytokines may be elevated. This condition, and the similar GULF WAR SYNDROME are still poorly understood. Several CFS patients were sent to me when I was in practice, and I had some success in getting them to exercise regularly, which seemed to help. CANCER is another category of diseases where Fatigue is prominent.
Inflammation plays a role in these diseases, which also drain energy substrates from the Patients body; Cancer cells have a high metabolic requirement. MEDICATIONS, Cancer meds especially, but a variety of other Drugs are associated with FATIGUE. I went through MY MEDICATION LIST. Lo and behold, 3 of them are associated with fatigue.
Finasteride is a relic of my prostate operation, recommended to keep it from growing back. It causes fatigue, probably because of its ANTITESTOSTERONE effect. At least I can still pee, and am not bald. I take METFORMIN because of its fame in prolonging life. Its mechanism is that of interacting with the Sirtuin system, and increasing the inefficiency of mitochondria. Isn’t this surprising?
Like many other things in physiology, you place a stress on the body, and the body responds by improving its performance. If you are fatigued, you exercise. Respecting the body works with drugs as well. If you are drinking a ton of coffee and stop it, after a few weeks you will feel less fatigued.
And when you ARE FATIGUED, you drink a LITTLE coffee, and it wakes you right up. Caffeine works by displacing ADENOSINE, which causes Fatigue as it increases through the morning, peaking at SIESTA (or tea) time,at about 2 PM. OMEPRAZOLE, which I take to prevent HEARTBURN, also is related to fatigue especially if it blocks MAGNESIUM for long enough. DEPRESSION overlaps with fatigue, as does SLEEPINESS, to increase the complexity of the situation.
Many chronic LUNG, KIDNEY and LIVER diseases are associated with fatigue as a secondary concern. STAY HEALTHY!
–Dr. C
THE DOCTORS 101 CHRONIC SYMPTOMS & CONDITIONS #4: HEARTBURN (ACID REFLUX)
I have been having Heartburn for more than 40 years. The cause of Heartburn is leakage of acid from the stomach, where tissues have evolved to tolerate the highly acidic conditions, into the esophagus, where they haven’t.
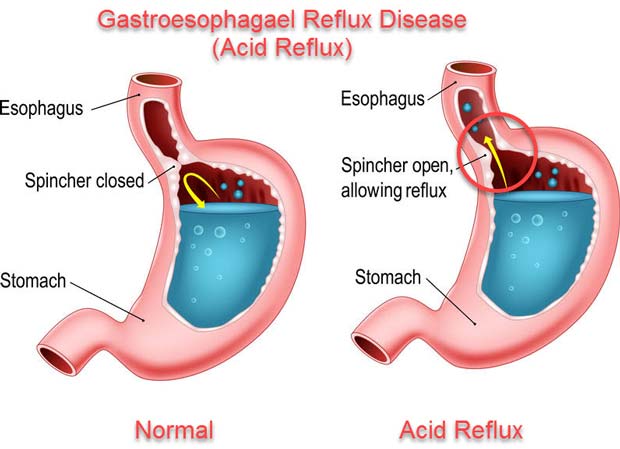
The young body has an efficient, functional gate, or sphincter, keeping the food, once swallowed into the stomach, from coming back up. As you eat, you chew your food well to aid digestion. Your taste buds, sensing chemicals in the delicious food, activate saliva.
The salivary enzymes start the digestion of the carbohydrates in the food. If you eat slowly enough, you may be able to appreciate the digestion of tasteless starch, like in bread, into sweet sugar, right in your mouth.
You then swallow the food, which slips past another gate, called the epiglottis, diverting the bolus of food past your windpipe. This gate sometimes does not shut tight, and you choke on the food or drink. The food is then conducted into the highly acidic environment of the stomach.
The stomach evolved to be an acidic, “fiery pit”, inhospitable to any bacteria that came in with the food, thus protecting the stomach from infection. In the old days, there were a lot of bacteria, and the acidity of the stomach was useful, and evolutionarily conserved.
These days, the “fiery pit” tends to be a problem. As you get older, the gate that keeps food in the stomach gets more floppy and relaxed, and allows food to come back up into the esophagus, and sometimes, most often at night when you would rather be sleeping, all the way up to your throat, and is inhaled into your windpipe and lungs in what is called “gastroesophageal reflux”, or GERD.
Even if the food, and acid, doesn’t make it all the way up, and stops at the esophagus, which has not evolved to tolerate acid, you will have “heart burn”. Of course it is not the heart that is burning, but the esophagus, which runs right past the back of the heart as it goes all the way from the throat to the stomach.
When I first developed Heartburn, all that was available was the flavored chalk, Calcium Carbonate, sold as Tums. It works right away, and is a source of Calcium, but can cause trouble, like kidney stones, if you take too much. The relief didn’t last long enough for me, and I had to take more in the middle of the night.
My next medicine was Xantac, a medication that blocks histamine from stimulating acid production in the stomach. The H2 blockers have recently been recalled because of NDMA contamination. I sometimes used H2 blockers like Xantac when my patients would get a bad allergic reaction. In such cases BOTH an H1 blocker like Benadryl, and an H2 blocker are called for.
Zantac was not strong enough for me, and I soon graduated to Prilosec,which directly blocks the secretion of acid in the stomach.

Prilosec was then very expensive, but now is available as the inexpensive GENERIC Medication, Omeprazole. It seems that no medication is without side effects.
Omeprazole, by reducing stomach acid, makes stomach and GI infections more likely, and interferes with the absorption of B12, and Calcium.
If you have had a lot of heartburn over a long period of time, you should check with a Gastroenterologist, who may scope you to rule out Barritt’s esophagus, which can lead to Cancer.
It is interesting that the antacid Tums in excess can cause too MUCH Calcium in the body, and can cause kidney stones and other kidney problems like MAS, and Omeprazole, by interfering with absorption can cause too LITTLE absorption of Calcium, leading to OSTEOPOROSIS.
The best rule is to take as low a dose of ANY medication as possible, preferably none, to understand the possible side effects, and compensate for them if you can.
–Dr. C
STUDY: “FRAGMENTED SLEEP” INCREASES INFLAMMATION & HARDENING OF THE ARTERIES
From UC Berkeley (June 4, 2020):

“We’ve discovered that fragmented sleep is associated with a unique pathway — chronic circulating inflammation throughout the blood stream — which, in turn, is linked to higher amounts of plaques in coronary arteries,” said study senior author Matthew Walker, a UC Berkeley professor of psychology and neuroscience.
Disrupted nightly sleep and clogged arteries tend to sneak up on us as we age. And while both disorders may seem unrelated, a new UC Berkeley study helps explain why they are, in fact, pathologically intertwined.
Some tips to improve sleep quality
- Maintain a regular sleep routine, going to bed and waking up at the same time each day.
- As part of a nightly wind-down routine, avoid viewing computer, smartphone and TV screens in the last hour before bedtime, and keep phones and other digital devices out of the bedroom.
- Engage in some form of physical exercise during the day.
- Get exposure to natural daylight, especially in the first half of the day.
- Avoid stimulants, like caffeine, and sedatives, like alcohol, later in the day.
UC Berkeley sleep scientists have begun to reveal what it is about fragmented nightly sleep that leads to the fatty arterial plaque buildup known as atherosclerosis that can result in fatal heart disease.
COMMENTARY
“How much sleep do we need”, and “Sleep Hygine” were past topics on this site, and my own sleep fragmentation was mentioned. This study correlates sleep fragmentation in the elderly with increased blood vessel disease compared to elderly people who have no interruptions in their sleep.
The elderly have several obstacles to a good, full night’s sleep, although a fair number of my friends claim the blessings of sleeping soundly. As we get older, we lose the deepest sleep we enjoyed as children, and there is some loss of REM sleep as well. The elderly sleep more lightly.
Diseases begin to accumulate as we get older, and These DISORDERS and their TREATMENT can disrupt sleep. I mentioned My BPH with it’s blockage of flow, leading to incomplete emptying of my bladder. This led to FREQUENT URINATION and frequent arousal at night.
With aging, the tissues in the throat become more flabby, and if you SLEEP on your BACK, your inhalation may be blocked. This may result in OBSTRUCTIVE SLEEP APNEA, where your breathing and sleep are interrupted repeatedly. The associated SNORING may interrupt the sleep of your partner, or even the sleep of those in the next room.
GERD, where you choke on regurgitated stomach contents, is more common in the elderly.
Chronic Heart, lung and Kidney disease can interfere with sleep.
SLEEP DEPRIVATION leads to a variety of problems, such as the inflammation and Arterial blockage highlighted in the above article.
Sleep is intimately connected with DIET and EXERCISE. As one of the PILLARS of HEALTH, It s well worth discussing with your Doctor and following her instructions.
—Dr. C.
THE DOCTORS 101 CHRONIC SYMPTOMS & CONDITIONS #1 – THE “CHRONIC COUGH”

In my 88 years, I have had at least a dozen medical problems. Some have gone away on their own, some have been removed surgically, and a few have become CHRONIC, lasting for years, ultimately becoming a part of my life.
I have compiled a list of these and other SYMPTOMS & CONDITIONS I have seen as a physician. Over the next year, I will discuss them one by one, appending these vetted articles for further reading.
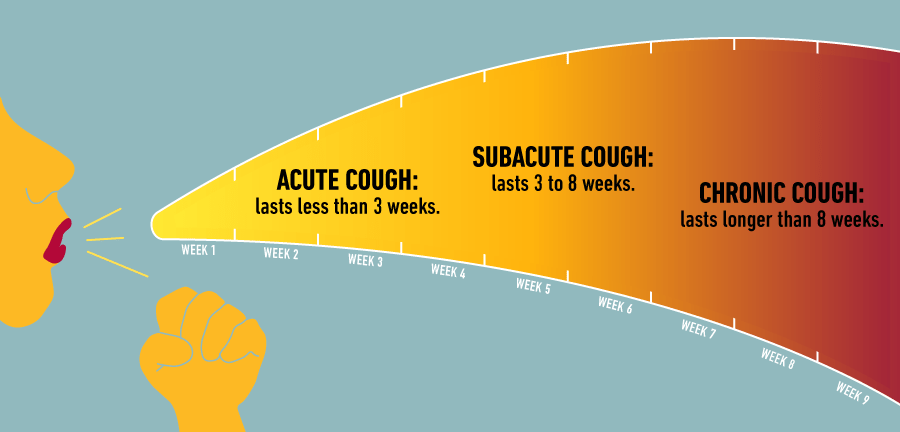
The ‘CHRONIC COUGH’ will be the first discussed.
As an Allergist, I was involved with coughing all of my adult life. If my patients did NOT have asthma, they usually coughed from mucus pouring down the back of their throat (post-nasal drip), from their allergic nasal condition (allergic rhinitis), or sometimes from the associated SINUSITIS drainage.
Asthma was a much more common cause of Chronic Cough for my Patients, sometimes theIr main problem. All asthmatic have a chronic inflammation of their breathing tubes(bronchi), and the resulting BRONCHITIS irritates the airway nerve endings, causing Cough.
Without enough narrowing of the airways to cause wheezing, this is called “cough equivalent asthma”. With the addition of airway narrowing (constriction) to the above situation, ASTHMA results.
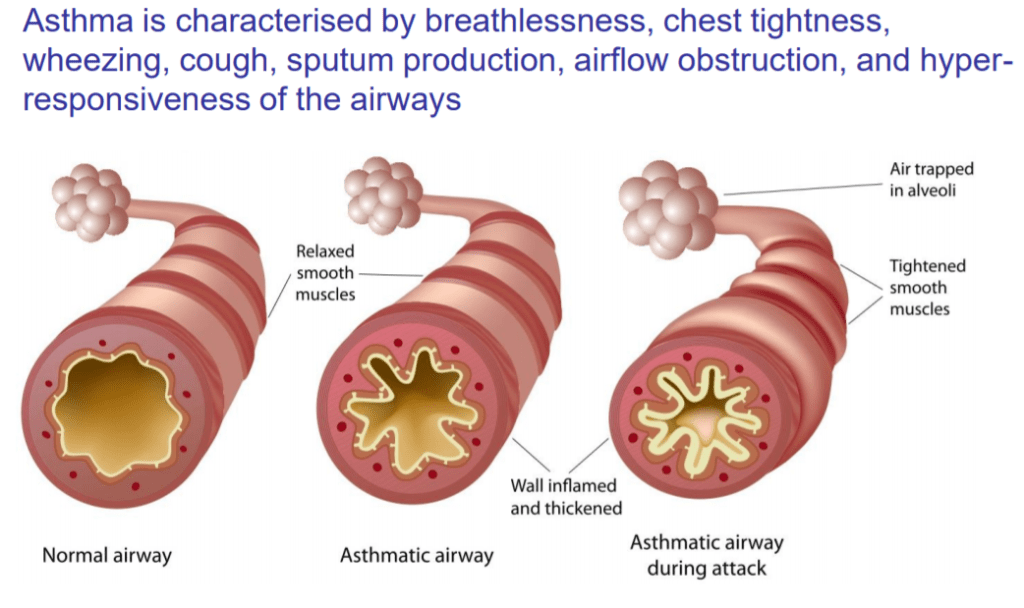
There is added shortness of breath (dyspnea), and the cough becomes the “tight” wheezy cough of full-blown Asthma.
COPD (chronic obstructive pulmonary disease) may be a residue of long-term asthma, but commonly results from cigarette smoking. Where loss of alveolae (air sacs) predominates, dyspnea (shortness of breath) is more common.
Where bronchial tube inflammation is more prominent, mucus and cough result. This cough is useful in clearing the mucus; a USEFUL COUGH (although my Patients did not always appreciate their friend, which could be bad enough to cause hernias or incontinence).
Gastro-esophageal reflux is a chronic condition where stomach contents are not retained in the stomach by the G-E Sphincter ( a type of “purse-string” Gate), but spill(reflux) up, when not restrained by gravity, at NIGHT. The ACIDIC STOMACH CONTENTS burn the esophagus on the way up(heart burn), and are often aspirated into the airways during sleep, causing inflammation and COUGH.
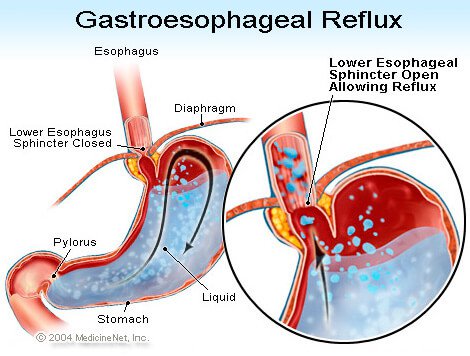
There are many other less common CHRONIC LUNG ( pulmonary) DISEASES (conditions) such as sarcoidosis, bronchiectasis, interstitial pneumonitis, TB, and cancer, that can be diagnosed by imaging (X-Ray, etc.). Heart failure can also cause cough, as can blood pressure medication (ACE inhibitors).
Smoking is an obvious cause; chronic smoking, chronic cough. Smokers know what is causing their cough, and usually don’t bother coming to the Doctor unless they cough up some blood, or develop one of the myriads of diseases caused by their habit.
If you have a chronic cough, check with your Primary Care Doctor, who may refer you to an Allergist or Pulmonologist. The following article will be useful to your understanding of cough, and will provide a LIST OF QUESTIONS the DOCTOR will likely ask you.
—Dr. C.
DOCTORS CALL: “CHRONIC COUGH – DIAGNOSIS AND TREATMENT” (MAYO CLINIC)
On the Mayo Clinic Radio program, Dr. Kaiser Lim, a Mayo Clinic pulmonary and critical care physician, explains chronic cough and how it can be treated.
COMMENTARY
If you have had a cough for more than 8 weeks, the good news is that you don’t have Covid 19. The bad news is that you need a Medical evaluation, tests and imaging to find out what is going on.
COUGH is not a disease, but is a manifestation, a SYMPTOM of a disease.
Your Primary Care Doctor will do a Medical History, an examination and a chest X-Ray which may allow her to DIAGNOSE what disease or problem Is causing the cough, and allow her to treat it.
If you continue to cough, you will be referred to a specialist, such as an Allergist or a Pulmonologist. ENT (sinusitis) and Gastroenterology (GERD) are 2 other medical fields often involved.
Usually blessed relief comes when Chronic Cough is properly diagnosed and treated, but a few Patients continue to suffer, challenging the best of medical care. 2 of my friends continue to cough after Medical School Level evaluations.
Nature continues to hide some of her secrets from Medical Science.