Chronic pain can develop from an acute pain state. The mechanisms mediating the transition from acute to chronic pain remain to be elucidated. Here, Parisien et al. focused on the immune system using samples from patients and animal models. Transcriptomic analysis in immune cells from subjects with low back pain showed that neutrophil activation–dependent inflammatory genes were up-regulated in subjects with resolved pain, whereas no changes were observed in patients with persistent pain. In rodents, anti-inflammatory treatments prolonged pain duration and the effect was abolished by neutrophil administration. Last, clinical data showed that the use of anti-inflammatory drugs was associated with increased risk of persistent pain, suggesting that anti-inflammatory treatments might have negative effects on pain duration.
Tag Archives: Lower Back Pain
Back Pain: The Causes & Symptoms Of Sciatica
Sciatica refers to pain caused by the sciatic nerve that carries messages from the brain down the spinal cord to the legs. The pain of sciatica typically radiates down one side from the lower back into the leg, often below the knee. The most common cause is a bulging (“herniated”) disc in the lower back. Discs are tire-like structures that sit between the bones of the spine. If the outer rim of the disc tears, usually due to routine pressure on the lower back, the jelly-like inner material can come out and pinch or inflame the nearby nerve. Sciatica is most common in people 30 to 50.
How do you know if it is sciatica?
The key to diagnosing sciatica is a thorough history and a focused exam. Sciatica symptoms are often worse with sitting or coughing and may be accompanied by numbness or tingling in the leg. A physical exam can confirm that the sciatic nerve is involved. If there is muscle weakness or diminished reflexes in the involved leg, an imaging test such as a back MRI can be useful and help guide a decision for early surgery.
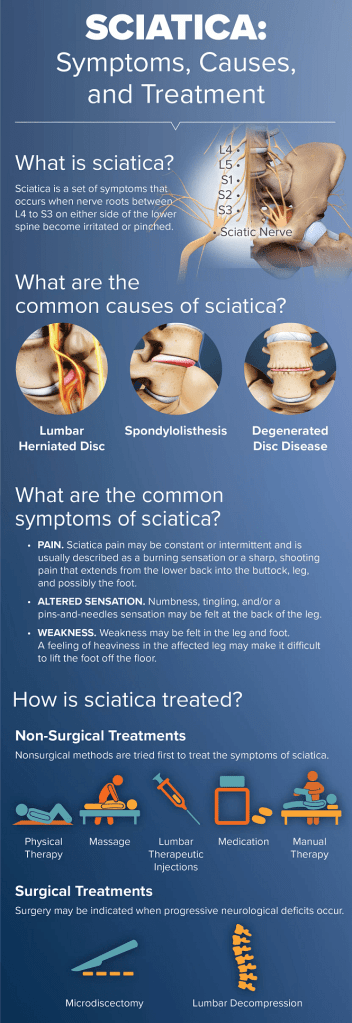
INFOGRAPHIC: “SCIATICA – SYMPTOMS & TREATMENT”