Mayo Clinic (March 30, 2023) – Spinal stenosis happens when the space inside the backbone is too small. This can put pressure on the spinal cord and the nerves that travel through the spine. Spinal stenosis occurs most often in the neck, called cervical spinal stenosis, and in the lower back, called lumbar spinal stenosis.
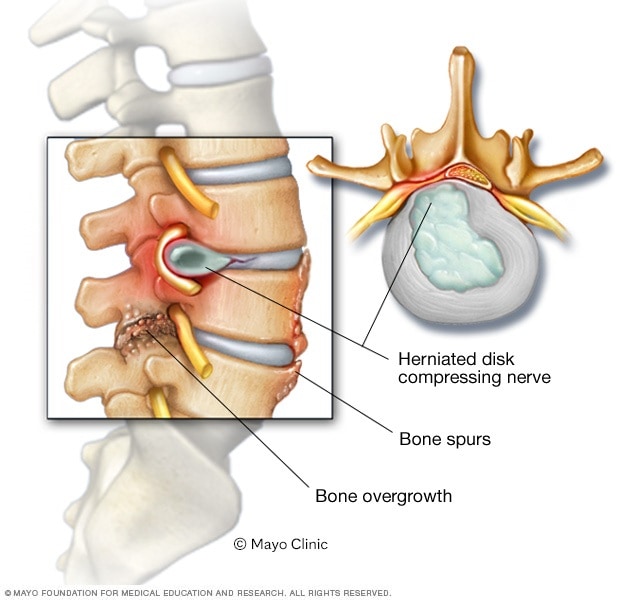
The most common cause of spinal stenosis is wear-and-tear changes in the spine related to arthritis. Most people with spinal stenosis are over 50. Younger people may be at higher risk of spinal stenosis if they have scoliosis or other spinal problems.
Symptoms
Spinal stenosis often causes no symptoms. When symptoms do occur, they start slowly and get worse over time. Symptoms depend on which part of the spine is affected.
Spinal stenosis in the neck can cause:
- Numbness
- Tingling or weakness in a hand, leg, foot or arm
- Problems with walking and balance
- Neck pain
- Problems with the bowel or bladder
Spinal stenosis in the lower back can cause:
- Pain or cramping in one or both legs that happens when you stand for a long time or when you walk
- Back pain
Treatment
Treatment for spinal stenosis depends which part of the spine is affected and the severity of your symptoms.
Nonsurgical treatment can include:
- Medication.
For control of pain, your health care professional might prescribe nonsteroidal anti-inflammatory drugs, antidepressants, anti-seizure drugs or opioids. - Physical therapy.
A physical therapist can teach you exercises that can build up your strength and endurance, maintain the flexibility and stability of your spine, and improve your balance. - Steroid shots.
Your nerve roots can become irritated and swollen at the spots where they are being pinched. Injecting a steroid medication into the space around the pinched nerve can reduce the inflammation and relieve some of the pain. Repeated steroid injections can weaken nearby bones, tendons and ligaments, though. That’s why a person often must wait many months before getting another steroid injection. - Removal of thickened ligament tissue.
Sometimes, the ligament at the back of the lumbar spine gets too thick. Needlelike tools inserted through the skin can remove some of the ligament. This can create more space in the spinal canal to reduce pressure on nerve roots.
Surgeries to create more space within the spinal canal may include:
- Laminectomy.
This surgery removes the back part, or lamina, of the affected spinal bone. This eases pressure on the nerves by making more space around them. In some cases, that bone may need to be linked to nearby spinal bones with metal hardware and a bone graft. - Laminotomy.
This surgery removes only part of the lamina. The surgeon makes a hole just big enough to relieve pressure in a specific spot. - Laminoplasty.
This surgery is done only on spinal bones in the neck. It makes the space within the spinal canal bigger by creating a hinge on the lamina. Metal hardware bridges the gap in the opened section of the spine.