Painful, stiff joints are almost the rule as we get older, it seems. Both osteoarthritis and rheumatoid arthritis contribute to that eventuality. Osteoarthritis typically worsens as we get older, whereas rheumatoid arthritis starts in middle age.
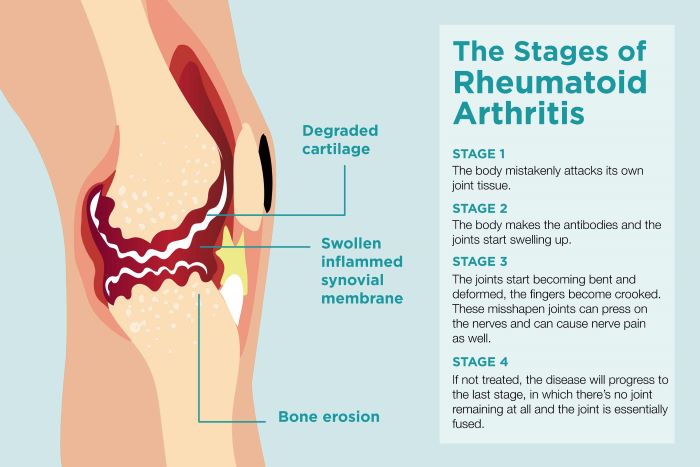
Rheumatoid arthritis is much more severe than osteoarthritis, since it is an autoimmune condition with an episodic inflammatory component. A recent medical study of different blood substances found that the “metabolome” has many markers for exacerbation of rheumatoid arthritis.
The main test currently being used to show exacerbation is CRP, C-reactive protein. Rheumatoid factor tests, such as anti-CCP, are used to confirm the diagnosis.
Rheumatoid arthritis tends to involve the small joints of the hand, and osteoarthritis the larger joints, such as the hips and knees. I go a bit against the grain, having diagnosed osteoarthritis of my fingers and toes, more typical of RA, but, even at the age of 89, my large joints are still in good shape, even with a lot of walking. Since walking is thought to increase the perfusion of joint fluid to nourish the knee cartilages, perhaps I should say BECAUSE of walking. Running tends to wear the knees and hips out, because of high impact on the joints.
The inflammation of rheumatoid arthritis tends to wax and wane, but during an exacerbation can be quite incapacitating. The interleukin TNF seems instrumental in causing these flares, and antibodies directed towards TNF, such as etanercept, has been a helpful treatment. This injection is also given for other inflammatory, autoimmune conditions such as psoriasis, particularly psoriatic arthritis, and the inflammatory bowel diseases.
Almost half the people who have rheumatoid arthritis also experience signs and symptoms in other tissues, such as the skin, eyes, heart, and lungs. It is truly a systemic, autoimmune disease.
For more information please consult the following mayo clinic article on rheumatoid arthritis.