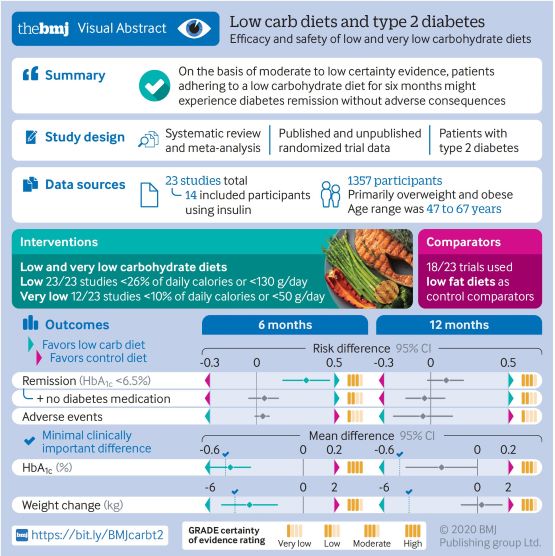
HEALTH STUDY: ‘LOW CARB DIETS’ – TYPE 2 DIABETES REMISSION IN 6 MONTHS


Dietary patterns with a higher proinflammatory potential were associated with higher CVD risk. Reducing the inflammatory potential of the diet may potentially provide an effective strategy for CVD prevention.
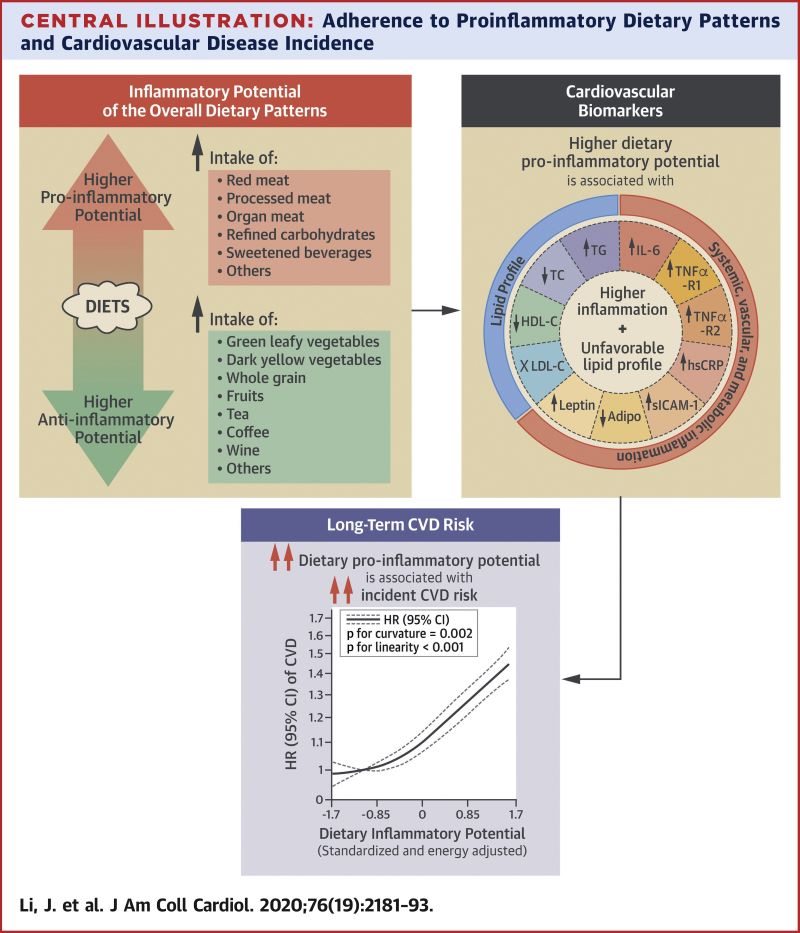
Inflammation plays an important role in cardiovascular disease (CVD) development. Diet modulates inflammation; however, it remains unknown whether dietary patterns with higher inflammatory potential are associated with long-term CVD risk.
From Phys.org/Univ. of Michigan (June 9, 2020):

“On a high-sugar diet, we find that the fruit flies’ dopaminergic neurons are less active, because the high sugar intake decreases the intensity of the sweetness signal that comes from the mouth,” Dus said. “Animals use this feedback from dopamine to make predictions about how rewarding or filling a food will be. In the high-sugar diet flies, this process is broken—they get less dopamine neuron activation and so end up eating more than they need, which over time makes them gain weight.”
It is well known that consuming food and drink high in sugar is not great for us, but scientists are continuing to unravel the intricacies of how the sweet stuff drives negative health outcomes. The latest finding comes from researchers at the University of Michigan, who through studies in fruit flies have found that excess amounts of sugar can shut down crucial neural circuits linked to regulating satiety, possibly leading to overeating in humans.
COMMENTARY
SUGAR IS A POISON.
A novel illustration of sugars’ lethality was the Georgia sugar refinery explosion in 2008, which killed 14 people. Finely ground sugar is flammable.
Sugar appeared early in civilization, but it was expensive, sparing all but the wealthy of its’ depredations, mainly tooth decay. Only with the post WWII expansion of wealth was it consumed excessively to produce the diseases of overeating. The developed world now consumes over 70 pounds of sugar per person, amounting to over 250 CALORIES PER DAY!
This article shows how SUGAR acts like a DRUG In its INTERFERENCE with the DOPAMINERGIC Reward system. The neurons send less signal, so you need MORE SUGAR to satisfy.
The metabolic systems through which overeating and sugar causes the OBESITY, DIABETES, VASCULAR DISEASE and Early DEMENTIA are convoluted.The best detailed explication is in the NEJM article in intermittent fasting, a healthful practice that is the polar opposite of overeating.
Two very important metabolic mechanisms are discussed, the mTOR system and the Sirtuin system. These systems are important for NUTRIENT SENSING and repair, and conserved in all animals. They worked just fine in our early ancestors.
It seems that primitive man was not blessed (or is it cursed) with easy overabundance or food, and actually spent hours or days in Hunger. When times were good, his body put on muscle, and stored fat against the hard times to come. This is called ANABOLISM. When times were bad, his body went into repair mode, and used the fat for energy. This is called CATABOLISM.
Anabolism has evolved expressly for Young Animals, where extra food is welcome for Growth. After the growing and Reproductive years, our Bodies’ evolutionary “warrant” expires, since the genes it carries have already been spread. Our older bodies are left to deal with machinery more suited to an earlier vibrancy. Our metabolism didn’t evolve to deal with the calories we shove into our aging Bodies. Many mechanisms beneficial in the young prove harmful later on. This divergence has been called “ antagonistic pleiotropy”.
Whatever the explanation, the observation remains: if adults eat more than they can use, they gain weight. With insufficient exercise, this weight is fat. With excessive fat, the joints, blood vessels, liver, heart and brain suffer, and lifespan is shortened.
RETHINK YOUR LIFESTYLE AS SOON AS POSSIBLE. AVOIDING SUGAR, and ALL THINGS CONTAINING SUGAR is as good a place as any to start. You will be rewarded by being able to fully taste and enjoy the natural sweetness of many REAL FOODS, and afforded a longer life to partake in this pleasure.
From The Lancet Diabetes & Endocrinology (June 2020):
Our findings show that the intensive lifestyle intervention led to significant weight loss at 12 months, and was associated with diabetes remission in over 60% of participants and normoglycaemia in over 30% of participants. The provision of this lifestyle intervention could allow a large proportion of young individuals with early diabetes to achieve improvements in key cardiometabolic outcomes, with potential long-term benefits for health and wellbeing.

Type 2 diabetes is affecting people at an increasingly younger age, particularly in the Middle East and in north Africa. We aimed to assess whether an intensive lifestyle intervention would lead to significant weight loss and improved glycaemia in young individuals with early diabetes..Between July 16, 2017, and Sept 30, 2018, we enrolled and randomly assigned 158 participants (n=79 in each group) to the study. 147 participants (70 in the intervention group and 77 in the control group) were included in the final intention-to-treat analysis population. Between baseline and 12 months, the mean bodyweight of participants in the intervention group reduced by 11·98 kg (95% CI 9·72 to 14·23) compared with 3·98 kg (2·78 to 5·18) in the control group (adjusted mean difference −6·08 kg [95% CI −8·37 to −3·79], p<0·0001). In the intervention group, 21% of participants achieved more than 15% weight loss between baseline and 12 months compared with 1% of participants in the control group (p<0·0001). Diabetes remission occurred in 61% of participants in the intervention group compared with 12% of those in the control group (odds ratio [OR] 12·03 [95% CI 5·17 to 28·03], p<0·0001). 33% of participants in the intervention group had normoglycaemia compared with 4% of participants in the control group (OR 12·07 [3·43 to 42·45], p<0·0001)