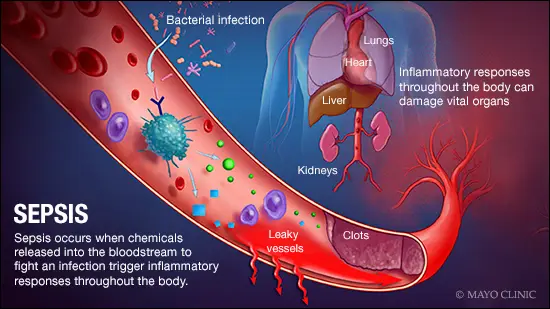
Sepsis occurs when the body’s response to an infection damages its own tissues. When these infection-fighting processes turn on the body, they cause organs to function poorly and abnormally.
As sepsis worsens, blood flow to vital organs, such as your brain, heart and kidneys, becomes impaired. Sepsis may cause abnormal blood clotting that results in small clots or burst blood vessels that damage or destroy tissues. If sepsis progresses to septic shock, blood pressure drops dramatically, which can lead to death.
Nearly 270,000 people in the U.S. die each year as a result of sepsis, and one-third of people who die in a hospital have sepsis, according to the Centers for Disease Control and Prevention.
Signs of sepsis
To be diagnosed with sepsis, you must have a probable or confirmed infection, and all of these signs:
- Change in mental status.
- Systolic blood pressure — the top number in a blood pressure reading — less than or equal to 100 millimeters of mercury, or mm Hg.
- Respiratory rate higher than or equal to 22 breaths per minute.
Signs of progression to septic shock include:
- The need for medication to maintain systolic blood pressure greater than or equal to 65 mm Hg.
- High levels of lactic acid in your blood, which means that your cells aren’t using oxygen properly.
Treatment
Early, aggressive treatment increases the likelihood of recovery.
A number of medications are used to treat sepsis and septic shock, including antibiotics, corticosteroids, painkillers and sedatives. Supportive care, including oxygen and dialysis, and surgery to remove the source of the infection, also may be needed.
People who have sepsis require close monitoring and treatment in a hospital ICU. Lifesaving measures may be needed to stabilize breathing and heart function.
COMMENTS:
The hospital is a dangerous places to be, and the most common cause of death there is sepsis. Sepsis is an underappreciated killer, and it’s getting more common because people are aging, devices are more commonly implanted into the body, immunosuppressive treatment is being used more commonly, and hospital acquired infections are increasingly resistant to treatment.
Sepsis can be caused by an overwhelming infection with bacteria, but can also be caused by viruses, fungi, and severe trauma. Low blood pressure is a common problem, and is associated with change in mental status, and increased breathing rate in raising a red flag for sepsis. Endotoxins play an important, if confusing, role. Endotoxins derive from Gram negative bacteria, but the most common bacterium causing sepsis is the gram positive staphylococcus aureus. With sepsis, though,the gastrointestinal tract may become more leaky, and Gram negative organisms may thereby gain access to the blood stream.
A ccmmon test to detect sepsis is the serum lactate, which becomes elevated if oxygen utilization is diminished, such as in sepsis. There is also a direct test for endotoxin in the bloodstream, performed by using LAL, or Limulus amebocyte lysate. This substance, derived from the cells of the blood of the horseshoe crab, is very sensitive to endotoxins, and coagulates in its presence. This test is also used to detect endotoxins in Biological products and devices, making horseshoe crab is quite valuable.
Maintaining general health, keeping up on your immunizations, wishing your hands, keeping cuts and burns free from infection, ovoid smoking, controlling diabetes and avoiding hospitals whenever possible are useful preventative techniques.
—Dr. C.

